An attempt is made to look for individual components of cell viability .See the table below. It is a generalized statement for understanding purpose only. Various imaging modalities assess the overall physiology of myocyte function (however they test an individual component of a cell more than the other) We may believe an unit of cell would die in “one-go” at times of ischemic injury.Reality is much complex.There is considerable variation in intracellular survival mechanisms . A cell can die in a regional fashion with residual signs of life scattered across among the different organelles. The quantum of damage to Nucleus /mitochondria may appear determine the recovery . The reverse can also happen .What is the purpose of mitochondria respiring if contractile element is totally damaged ? It becomes a “vegetative cell”. The gross discrepancy we are witnessing in myocyte cell function recovery with reference to both acute and chronic reperfusion is attributable to this gap in our knowledge.
Posted in stress doubtamine echo, Viability assessment | Tagged doubtamine stress spect demri thallium, Hibernating vs stunned myocardium, myocyte viability, pet scan, vegetative myocyte, viable vs non viable myocardium | Leave a Comment »
It is believed (assumed ?), medical science is propelled by constant quest for knowledge and improvement in basic and clinical science that eventually would transform into better patient care and favorably impact global health standards. We know the field of medicine is growing in an unimaginable pace.It’s obvious any growth if uncontrolled or not properly guided is at risk of deviation from the main goal and ultimately turn malignant and destroy the system which it’s supposed to guard.
How many times we realise the current treatment we administer would soon become obsolete and even become dangerous ? What is the point in replacing treatment A by B , and then B is pulled over by C or D and suddenly finding A is better than either C or D (and still we hesitate to fall back on A because its an oldie!)
Still ,this is what we call as practicing ” State of the art medicine” How about a person who defies state of the art , and able to fore- see the futility which is threatening to be the norm in modern medicine. Then,who is really Ignorant ?
I stumbled upon this wonderful writing on this issue by ex BMJ editor by Richard Smith. Mind you , this was published way back in 1992, when the boom of futile ” Human Health shopping” was just about to explode !
Link to The ethics of Ignorance
Post-amble
Don’t get confused .Noble professionals are licensed to practice with whatever is published as science as long as their intentions are deemed to be genuine .Harm arising out of practicing what’s considered best as on today is acceptable in the court of law.
Meanwhile , its a tragic truth, If you do not follow the herd , you are at risk of being punished even for goodness committed by you. Wisdom and conscience can never win a legal battle ! If you have the courage try practice them !
Posted in Medical ethics | Tagged ethics of ignorance, medical ethics | 1 Comment »
Heart and kidney work in tandem and share a close functional relationship during health and disease.Progressive cardiac failure causes kidney function to deteriorate,what we call it as cardio -renal syndrome.Similarly, progressive renal disease inflicts either a reversible /irreversible LV dysfunction .The mechanism of LV dysfunction has not been fully decoded. It is primarily biochemical mediated but at later stages it can be irreversible and structural damage can occur.
We believe uremic micro molecules leaking from plasma into cardiac Interstitium (Myocardial proteinuria ?) are somehow responsible for the progressive LV dysfunction. Now , we have new evidence for albumin – carbon interaction possibly at myocardial level due to formation of carbamino albumin (C-alb) .
This paper from Kidney International (2015) 87, 1201–1208; highlights this new finding .
 Elevated C-albumin is a new marker for this unique , still not fully understood entity “Uremic cardiomyopathy”.
Elevated C-albumin is a new marker for this unique , still not fully understood entity “Uremic cardiomyopathy”.
Further reading
Posted in Cardio Nephrology | Tagged biochemistry of cardiac failure, c-alb, c-albumin, carbamylated albumin, dialysable lv dysfunction, mechansim of lv dysfucntion in ckd, uremic cardiomyopathy, uremic lv dysfunction | Leave a Comment »
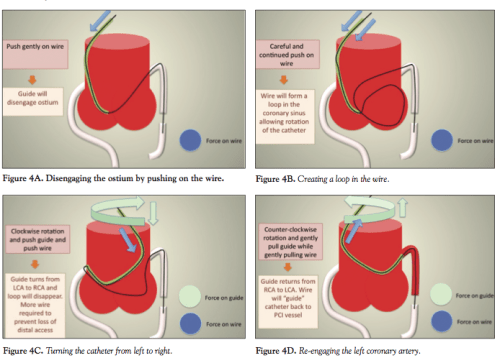
Radial coronary interventions has become a global norm .Even complex procedures are being accomplished with ease adding on to the patient comfort and low risk for access site complications.However !occasionally we need to have multiple access sites to know the detailed real time contra lateral coronary anatomy is desirable .This becomes vital in the retrograde approach for CTO.
Want to have a quick glimpse of RCA flow while one is attempting LAD PCI without additional puncture ?
How about doing a contra-lateral angiogram with the same guiding catheter and wire in-situ within the ipsilateral ostia ? Here is an Innovation.
Of course ,the same concept can be used in femoral angiogram as well.It could reduce procedural time, adds more efficiency of the hardware system handling. One can’t ignore the idea as well as the comment of the author, who says the trick is only for an advanced Interventional cardiologist.
Reference
Posted in Chronic total occlusion, Radial Interventions, Tips and tricks in cath lab | Tagged cath lab tips, contralateral coronary angiogram, radial tips and tricks, radial vs femoral angiogram, retrograde appraoch for cto | Leave a Comment »
STEMI occurs due to acute occlusion of a coronary artery (ATO) which needs emergency opening at the earliest, ideally within 3 hours , or up to 12h . The opening shall be either by pharmacological / catheter means or both. After 24 hours opening a ATO has questionable benefit unless the patient is hemodynamically unstable or symptomatic.
What is a CTO ?
Traditionally we believe 3 months is the period to call a coronary occlusion as chronic.(Previously it was 6 months) This time frame was considered appropriate based on our understanding of the infarct process , that may take up to 3 -6months for complete healing of infarct .This 3 month period is arbitrary as the chronology of intra-coronary lesion organisation is different from myocardial infarct healing. Its worthwhile to note the chronicity of a coronary lesion and its morphology is nothing to do with the quantum of myocardial damage it inflicts .This is because in many patients with STEMI who present late , the ATO progresses to CTO silently without any clinical demarcation or progressive myocardial damage.
If 24 h is the cut off point for opening the ATOs to accrue any meaningful benefit , can we call all ATO’s beyond 24 h as physiological CTO equivalents ?It doesn’t make sense isn’t ? But , consider this , how do you call an occluded coronary artery between 24 h t0 say 2 weeks or 2 weeks to to 3 months ? Sub acute total occlusion (STO) ? .Some experts have argued to remove CTO as an entity from acute coronary setting .This can’t be done as chronicity has to set in for ACS lesion as well. Obviously , we have a nomenclature issue here. We require a new terminology to differentiate CTO related to ACS and CTO related to chronic coronary syndromes.
Therapeutic implication
The moment we diagnose a true chronic total occlusion , not only the urgency of intervention but also the indication to open becomes questionable in an otherwise asymptomatic population.
An ironical situation often arises , when we can’t technically open a ATO in a one week old STEMI .However , the same lesion one may open after 3 months as it has acquired a new name by now as CTO , which is perceived a lesser guilty act of violating the sacred PCI guidelines !
Posted in Uncategorized | Leave a Comment »
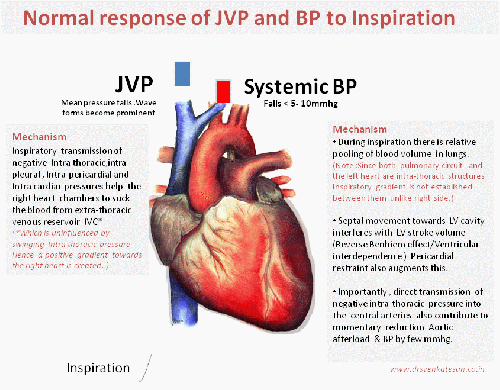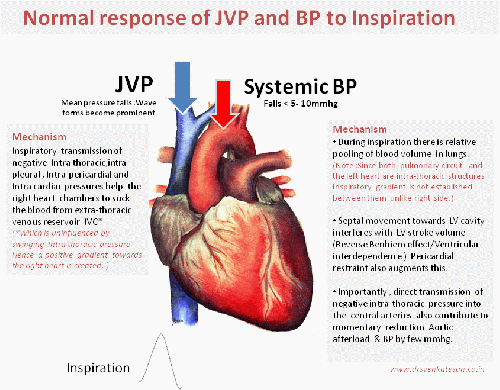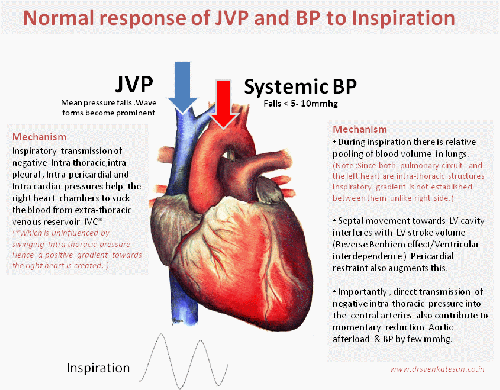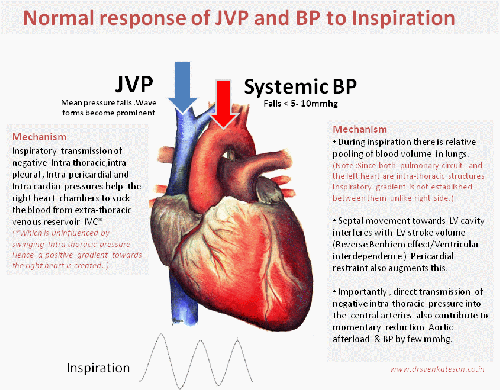
Image modified from http://www.anatomygallery.info
That’s normal . . . what happens during pathological states ?
There are important diseases that restricts entry of blood into right heart chambers. They can occur either in an acute (Tamponade) or in chronic fashion like constrictive pericarditis and restrictive cardiomyopathy.These entities show distinctive impact on JVP and systemic pulse.
The two pathognomonic signs are Kussmaul sign and pulsus paradoxus* that go hand in hand in most situations.Inappropriate elevation of JVP with inspiration is termed as Kussmaul sign , while exaggerated fall in systemic BP with inspiration is called Pulsus paradoxus.The later is the arterial counter part of Kussmaul sign in JVP .However, there can be dissociation between these two signs occasionally.
* Pulsus paradoxus is a term originally used by Kussmaul when he noted heart sounds were retained while pulse dissappeared in patients with cardiac tamponade .Later we realised the loss of pulse was linked to inspiratory cycle of respiration. To make this sign objective sphygmomanometery criteria was formulated which measured the difference between inspiratory and expiratory korotkoff’s sounds .
Coming up next
Why Kussmaul sign is often absent in Tamponade while its arterial counterpart pulsus paradoxus may still be conspicuous ?
Posted in Clinical cardiology, Jugular venous pulse, pericardial disease | Tagged bernhiem effect, effect of inspiration on jvp, kusmals sign, kusmaul sign, kussmal's sign, Kussmaul sign, pulsus paradoxus, Reverse bernheim effect, ventricular interdependence | Leave a Comment »
Right ventricle,being a venous chamber has distinct anatomical and physiological features to carry out this function.RV has a complex shape, its triangular in long axis and crescent like in short axis , thin (<5mm) more distendable .Contraction of RV begins slightly early but ends later than LV (30ms )
RV receives blood from RA and ejects in to PA in a sequential manner .The inflow, body and outflow contract somewhat like intestinal peristalsis. This is facilitated by the incremental delay in the electrical depolarization of right ventricle.In physiological conditions, the later half of QRS is responsible for RV activity and RVOT is the last to contract. (This intrinsic electrical and mechanical delay in RV contraction is a physiological inter ventricular desynchrony . One should be aware of this when planning cardiac resynchronisation therapy in cardiac failure. )
Click over the image for an animation of RV contraction.

Image courtesey Oxford spcialist hand book in cardiology :Echocardiography Paul Leeson , Second edition ,.Oxford university press 2012 Multi media .
Note:LV is a fairly elliptical and strongly muscular pump and contracts in a single go with maximum force.(dp/dt).
Final message
Though both right and left ventricle originate from same straight heart tube , developmentally the right ventricle evolves for a different form and function . Now,we realise there are lots of sharing of parental muscle fibers that engulfs and bonds both chambers.(Mind you ,This is the fundamental mechanism of ventricular interdependence.Of course ,IVS is a common wall shared lifelong by both chambers without any (sibling related?) hemo-dynamic dispute !
3D echocardiography and MR imaging has helped us to understand the RV morphology better and exciting articles written by pioneers are available free for those who are interested.
Reference
Posted in Anatomy of heart, Right ventricle | Tagged best articles on right ventricle, cardiac peristalsis, physiological inter ventricualr desynchrony, Right ventricle anatomy and physiology, right ventricular sequential peristaltic contraction | Leave a Comment »
These two quotes on practice of medicine are close to my heart , one from Voltaire , a non medical man (a French poet ) and the other from ,one of the greatest medical professional of our times, William Osler .
It is amazing ,how the thinking pattern of a philosopher and a true scientific professional living centuries apart are almost in sync with a great medical reality !
Posted in medical quotes, Two line sermons in cardiology | Tagged great medical quotes, medical quotes | Leave a Comment »
J point is a critical point in the ECG when the ventricles hand over the baton in the electrical relay race from depolarization to repolarization .This the time the sodium channels extinguish itself and the potassium current begins its activity from Phase 0 to 1 .
If the potassium channels activate little early and snatch the baton prematurely from sodium , we get early repolarization pattern .When this happens , the J point of ECG show a conspicuous wave called J wave , originally denoting Junctional wave between QRS/ST segment (Now perceived as Jitter waves ?) The other implication of premature K+ activity is , lifting up of ST segment , making it the most common cause of non ischemic ST elevation.
* J wave in hypothermia is referred to as Osborne wave and may not be not related to ERS(Ref.4)
The Ito current is responsible for the phase 1 of action potential (AP), where a rapid outward k + ion flux take place and draws the dome of AP . The dynamics of Ito is complex .It depends upon the density of epicardial K + channels , which are clustered in a heterogeneous manner .There seems to be a concentration gradient along the epicardium and endocardium , making the wave appear prominent in some. This is especially true in healthy, athletic male population where we have some evidence for androgen to play a role on how these channels will behave.Here comes the overlap between Brugada syndrome and ERS as well.

Image source : http://www.research.chop.edu
The subset of patients with J wave pattern were recently shown to have increased risk of primary VF due to phase 2 reentry , when they develop ACS. (Rather J wave pattern was more common in patients who had primary VF following STEMI(Ref 1).This resulted in a spate of worrying articles .Now we know , the fear is largely unfounded ,the risk is far less.
Current thinking is, persons who have asymptomatic ERS pattern with prominent J waves should not be investigated electro-physiologically . (Please remember , every human heart can be induced to VF in EP lab if appropriately stimulated ! )
In fact , I used to tell the young men who harbor prominent J wave , as a marker of healthy heart rather. Let us not fear them with a remote risk that could be as negligible as risk of intercontinental flight crashing into the ocean !
References
Posted in Brugada syndrome, cardiology -ECG, Cardiology-Arrhythmias, early repolarisation syndrome, ECG -Basics | Tagged brugada syndrome and ers pattern overlap, ers pattern, Fear of J waves in ECG, j point in ecg, j wave beingn waves, j wave syndrome, Jitter waves in ecg, junctional point in ecg | Leave a Comment »
Have you felt like this query any time in your office ?
If “Yes” is your answer, then you are not alone .There was a unique conference that took place in 2010 to answer the same query in Rome , Italy on behalf of Italian cardiology society , where this entity is researched more than any other place.Its worth going through this.
Reference
Posted in Brugada syndrome, Cardiology - Electrophysiology -Pacemaker, early repolarisation syndrome | Tagged brugada syndrome, consensus conference brugada syndrome, how to follow up brugada pattern ecg, suspected brugada syndrome | Leave a Comment »