Left atrial clot is a traditional contraindication for performing PTMC. This rule was formed in the early days of PTMC.
PTMC recently celebrated its 25th birth day . In India it was first done by GB Pant hospital by Kallilulah in early 1980s.
Now most centers do it routinely like a diagnostic angiogram. Even fellows can do it with ease. (If allowed !)
We have learnt the nuances of septal puncture , maneuvering the transpetal needle and the balloon catheter within the LA in the last two decades.it is also becoming clear how the IAS anatomy behaves in various LA and RA sizes and pressures . So , the experts (Read again . . .experts !) have relaxed the rule of the PTMC game !
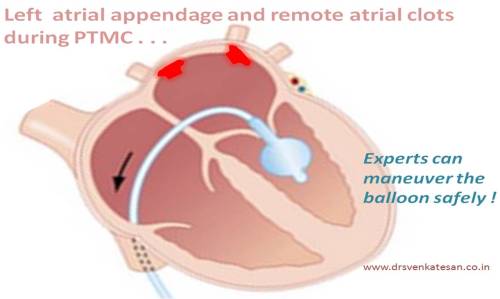
PTMC can safely be done if the LA clot is confined to the appendage .Even clots abutting just out of LAA appendage may be tried if you have the expertise akin to Dr Manjunath and his team from the garden city of India .(Jayadev institute , Bangalore probably has the largest talent pool for PTMC , In fact they have classified the LA clot according to size and location .) Read the reference below.
If a cardiologist is allowed to meddle the LA filled with clot , why not a surgeon do a CMC in the presence of LA clot ?
I believe old generation surgeons did it. I am told few surgeons have specail talents to deliver LA clot off pump and complete a successful CMC with lateral thoracotomy . Fresh un organised clot can be flushed out of LA .
But currently doing a CMC with LA clot is considered unscientific . Further surgeons often consider CMC as an inferior Job .They love to go on pump and replace mitral valve with a slightest provocation . It need be realised a half functional native valve is at any time better than an artificial valve . In developing countries CMC would make lot of sense when we confront with small LAA clots . One can do 5 CMCs at the cost of one mitral valve . Surgeons comments are welcome.
What will happen if LA cot gets accidentally dislodged ?
A stroke or a systemic vascular event may occur , but it depends upon the embolus size .Up to 2mm clot debri can easily cross the cerebral microcirculation and escape a major stroke.Showers of micro emboli can cause a lacunar infarct or vascular dementia.
By the way , I am curious to know what will happen to these clots after successfully opening the mitral valve by PTMC* ?
PTMC can not be claimed as a cure as long as the patient harbors the clot in a precarious location . So it needs intensive oral anticoagualtion (or even heparin ) and many times we have observed these small clots disappear .
*Logic would suggest an LA clot with a closed mitral valve could be much safer ! many times we have seen large LA clots struggle to get past the mitral valve because of critical stenosis.
A video of mobile LV clot from our institute . http://www.youtube.com/user/venkatesanreddi#p/u/40/zHdPtm32YZQ
Here there is no chance of PTMC , however good you are !
Future innovations
- Distally protected PTMC
- Either you should trap it and remove it or desiccate it into minor particles.
- Basket in root of aorta to capture the clot in transit may be a good concept to try.

What happens to LA clot following long term oral anticoagulations ?
Most disappear according to a study from JIPMER , Pondicherry , India .

http://www.ncbi.nlm.nih.gov/pubmed/14686666
Excellent PTMC data from Pakistan and Sudan
If you want to learn about PTMC please note the experts are not in Cleveland clinic or from Great ormond street
they are from the remote third world locations .
http://www.sudjms.net
http://www.ayubmed.edu.pk
Read Full Post »









