A middle-aged man was rushed to cath lab with extensive antero- lateral STEMI . Primary angioplasty was planned.The coronary angiogram showed a critical LAD and a total LCX lesion just beyond the bifurcation . Both lesions looked irregular and hazy . RCA had insignificant lesions . Patient was stable hemo-dynamicaly .
The moment we saw the angiogram, we knew , we had a real problem on hand ! . First of all , It looked a complex lesion for a pPCI .(A brief thought about an emergency CABG creeped in, but was dropped with enthusiastic residents voted unequivocally in favor of PCI . Of course , to be frank we didn’t have a CABG team ready either ! )
So the plan was : To open the IRA . . . & forget the non IRA ( for the time being ) which is the current management mantra as on 2012 !
Trouble from unusual quarters ! By the way . . . which is the IRA ?
Even as the consultant was initiating the rituals with wires and balloons to tackle the LCX , some one behind the consultant mumbled “why can’t the LAD be the IRA ” After all , it also has a critical lesion and mind you we are dealing a case of anterior MI !) . That mumble was loud enough to create buzz of confusion in cath lab .
Now everyone quipped , ” IRA is what ?
Is that the critical mid LAD lesion ?
(or ) Is it the total LCX (or ) Both ?
Logic would suggest in the setting of STEMI any total occlusion should be considered as IRA . Of course , one can not be dogmatic about it. When a patient is having anterolateal MI both LAD and LCX can contribute to the MI .
What about proposing a new concept of “Double IRA” ?
When multiple plaques are activated suddenly in unstable angina , it is possible for multiple IRAs to occur in STEMI as well . But this issue is rarely discussed in literature .
Other possibilities
The 100 % lesion in LCX could still be the primary culprit and a thrombus migration into LAD might have resulted in infarct extension into anterior wall .
Further , confounding may occur if a patient with chronic total occlusion develop a SEMI . It makes it really difficult to identify the IRA.
When the supposedly gold standard coronary angiogram fails to identify the IRA , what shall we do ?
Go to the basics . The good old ECG might help .
(Please beware in a patient with pre- existing multi-vesel CAD , none of the ECG algorithms work to localise IRA !(Especially the famous Wellen’s miserably fails ! )
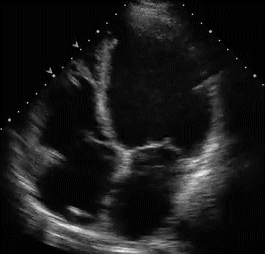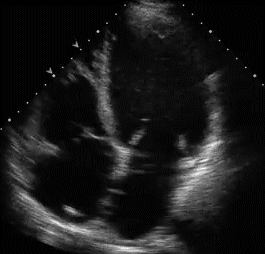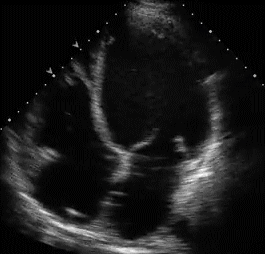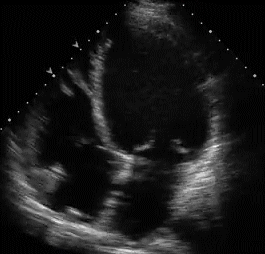
Still unclear ? Look for the wall motion defects in echo . An echo cardiogram (Need to be meticulous ) will help match the dysfunctional segment with IRA.
Wall motion defects are notoriously error prone in ACS for two reasons.
- We do not have easy and accurate methods to differentiate ischemic wall motion defect from infarct related wall motion defects.
- Tethering artifacts , differential behavior epicardial vs endocardial ischema on contractility will confound the issue .
So what is left ?
One need to go back to the CAG again . Have a critical look at the lesion once more. Look for thrombus or eccentric /unstable lesions . If present it is going to be the IRA in 90 % of times. Let it be a wild guess in the remaining 10 % .
There is also a practical solution . Poke the lesions with your favorite guidewire ! . The one that gives way easily is likely to be the IRA !
Finally, if the confusion still prevails ,
Stent both the lesions. That’s what , was done to this patient . Many would have thought , this should have been the default approach instead of scratching our heads to identify the IRA , wasting crucial minutes !
Final message :
Current guidelines do not recommend pPCI for non -IRA at the same sitting of IRA pPCI . However the issue of IRA “too close to call “ is rarely addressed.I do not know how commonly this issue is encountered in angiographic core labs that deal huge loads of pPCI world wide .
Our early experience suggest the problem is real , unique and definitely not rare .
What is your take ? We argue guidelines committee to specifically address the issue of uncertain IRA as a branch point in the pPCI decision making tree !