Hurricanes are ocean’s reaction to the climate change especially in subtropics. When low pressure zones form over the ocean surface the nidus for hurricane is sown .It gradually intensifies to form deadly cyclones.The maximum damage is done when it encounters the land . The following image depicts how the hurricane Katrina caused havoc in the southern US coastline .

Hurricane katrina .Click to view animation
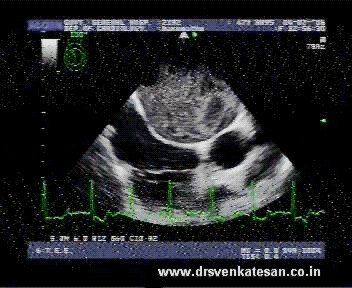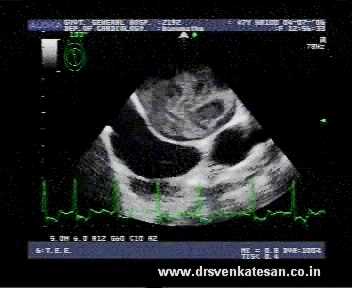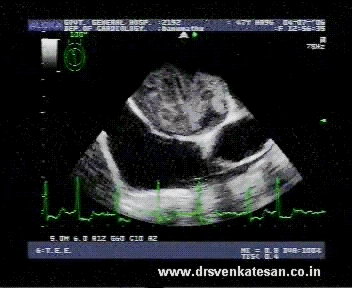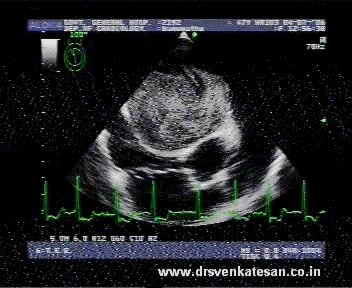
When the human blood stream is interrupted by any pathological hurdle it gets agitated . It encounters both turbulence as well as a slow flow phenomenon . Virchow taught us centuries ago , slow flow , a vessel wall defect and an abnormal blood combine to create a clot. This is what happens in mitral stenosis . What appears as a mild turbulence gathers momentum and becomes a storm .The eye of the storm has the least velocity and it forms the core of the future clot.
What is left atrial jelly ?
A pre- clot stage with impending clot formation may be referred to as a jelly . The exact duration for a contrast to get converted to clot is not known.It depends host of factors from hemodynamic and rheological factors. It is believed every clot must be preceded by at least a brief period of auto contrast.
Is there a intrinsic defect in blood in those patients who have spontaneous contrast ?
Yes , there has been excess fibrinogen in these patients. http://www.ncbi.nlm.nih.gov/pubmed/11744141
Can we dissolve spontaneous contrast ?
It may be possible with intensive anti coagulation. Ultrasonic dessication may be a modality that could be developed in future.
Is the presence of spontaneous echo contrast a contraindication to do PTMC/CMC ?
Some centers do believe so. Currently intensive anticogulation , meticulous preparation with special precautions during procedure will reduce embolic manifestation.
Reference