Posted in Uncategorized | Tagged dr s venkatesan, hdl and atherosclerosis, human atherosclerois, mechansim of atheroscerosis, venkat quotes | Leave a Comment »
I recently came across an unusual LIMA arterial branching pattern .
Random thoughts
- A naturally dividing LIMA faciliates multiple sequential grafting of LAD or diagonal branches.
- As branches steal the LIMA flow it is not good for the patient
- Surgeons struggle to clip the branches.
- A branching LIMA has tendency to have small diameter (As in the above patient )
I need a surgeons Input here.
Posted in cardiac surgery | Tagged cabg, lima graft, sequential lima graft, terminal lima branching | 1 Comment »
By statistics cardiomegaly often implies ventricular enlargement (especially left ventricular) .Right ventricle generally do not enlarge the CT ratio until late stages .
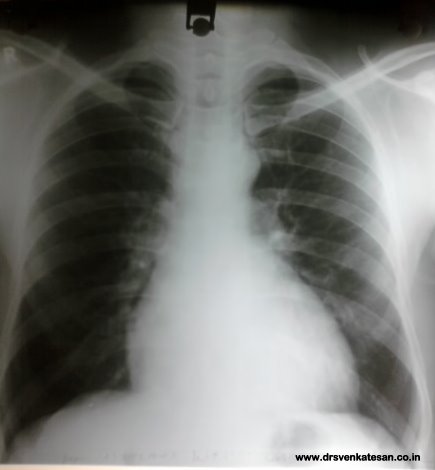
More important is the impact of right atrial enlargement on the CT ratio. Here was a patient referred to echo lab for evaluation of cardiomegaly
The x-ray chest was suggesting a definite LV enlargement. To my surprise the LV was perfectly measuring a normal dimension .
The right atrium was huge and measuring more than 5 cms . This increased the CTR.
The following illustration tries to create echo equivalent of transverse CT diameter by rotating apical 4 chamber view by 90 degrees.

The right and left atrium was significantly dilated . This patient had atrial fibrillation and the atrial enlargement was due to chronic AF.
Final message
Cardimegaly in X- ray chest do not necessarily mean ventricular enlargement.
Pure atrio-megaly especially right atrial enlargement can dramatically increase the CT ratio.
This is not a big discovery , still fellows need to reinforce this fact , as mistakes are most often committed in well known things !
Posted in valvular heart disease, X ray | Tagged cardiomegaly, in x ray chest pain, lv configuration, rv configuration | Leave a Comment »
Beta blockers are vital drugs to limit infarct size and facilitate myocardial salvage. Myocyte death is prevented by reducing MVO2.These concepts originated in early 1980s when thrombolysis was not in vogue .Studies like MIAMI and BHAT were considered landmarks.
Later on , when IV thrombolysis came in a big way the importance of beta blockade in STEMI suffered a little , still it held on to their benefits.
The real problem arose when few enthusiastic cardiologists introduced early multiple blouses of IV beta blockade in the setting of Acute STEMI without realising the potential danger. (In all probability man kind must have lost many thousands of lives with this aggressive beta blocking protocol world over for nearly a decade !)
Fortunately we woke up and in early 2000 , a massive study called COMMIT was initiated to answer convincingly the utility value of routine early IV bet blockade. Rest is history . It clearly showed us the what we were fearing was indeed true. An unacceptably excess cardiogenic shocks were reported in the early IV beta blocker arm .In the same period of time the concept of primary PCI exploded and the BBs were pushed to sidelines
It is a different story altogether . . .
While the funny world of cardiology showed the door for routine early beta blockers in STEMI , it made a stunning U turn in the management of CHF , after being dumped as an absolute contraindication for so many years !
Still COMMIT fails to answer many queries
- Beta blockers in LBBB /RBBB – Probably need to be avoided.
- Beta blockers in bifasicular block – Should be an absolute contradiction
How do you know tachycardia in STEMI is due to high sympathetic activity or cardiac reserve ?
Young men with persistent tachycardia will do well with beta blocker started within 24 hours .
Unless there is s3 or basal rales all tachycardia are to be considered as purely inappropriate and adrenergic
Tachycardia in elderly, women, and diabetic especially the blood pressure hover around 100mmhg is more often a compensatory phenomenon.Meddling the heart rate with BB is vested with a risk.
Finally , if you have a doubt do a rapid echo , if the EF is > 45% one can safely administer BBs
Should we discontinue BBs in those who are already taking it ?
Continuing the beta blocker is thorough the STEMI phase is adviced .(Unless specific contraindication exists )
Beta blocker following primary PCI
The beneficial effect of early Beta blocker even in post thrombolytic era is blunted, it goes without saying primary PCI almost nullifies these effects.
still , beta blockers is to be introduced after a successful primary PCI in all patent for long-term protection.
Final message
Do not rush into start beta blocker routinely following STEMI . The risk is not worth taking !
Reference
ACC/AHA guidelines on Betablocker and STEMI
The following is taken from the above guidelines When not to administer IV beta blocker seems to be more relevant !
Class 3 recommendation for Beta blocker in STEMI (Evidence A)
1. IV beta blockers should not be administered to STEMI patients who have any of the following: 1) signs of heart failure, 2) evidence of a low output state, 3) increased risk* for cardiogenic shock, or 4) other relative contraindications to beta blockade (PR interval greater than 0.24 seconds, second- or third-degree heart block, active asthma, or reactive airway disease). (Level of Evidence: A)
*Risk factors for cardiogenic shock (the greater the number of risk factors present, the higher the risk of developing cardiogenic shock) are age greater than 70 years, systolic blood pressure less than 120 mm Hg, sinus tachycardia greater than 110 bpm or heart rate less than 60 bpm, and increased time since onset of symptoms of STEMI.
Posted in Uncategorized | Tagged acc aha guideline in stemi, atenolol and metoprolol iv in stemi, beta blcokers in stemi, cardiogenic shock in stemi and beta blocker, commit beta blocker, commit study, compensatory tachycardia in stemi, EARLY IV BETA BLCKER, lvf and beta blocker, stemi guidelines | 1 Comment »
I recall the guilty days during my fellowship where many lives were lost due to delayed or faulty intubation in patients with cardiogenic shock. If only these devices were available those days . . .
It is ironical , why we took such a long time to make a scope to see a structure just beneath the oral cavity , while we were able to see remote duodenum and jejunum with video scope some 25 years ago !
Another device , which will come as handy would be the rapid bed side measurement of Aortic dimension .
It doesn’t require an expertise of a sonographer I believe .
Both these innovation come from Verathan
Reference
Video Laryngoscope & Aortic Scan
http://www.verathon.com/products/glidescope/avlsingleuse.aspx
Posted in Technology | Tagged aortic scanner, cardiology technology, modern cpr, rapid intubation cpr, verathan, video laryngoscope | Leave a Comment »
Cardiac arrhythmias by nature connote a serious implication ,especially so with ventricular ones. Here is an arrhythmia which arise from the ventricle by excessive automaticity , fires independently , still very benign compared to others ventricular arrhythmias.
Why AIVR is a stable arrhytmia ?
Primarily due to its low rate.
Since it is a reperfusion arrhythmia the outcome is good.
Mechanism
It is not due to reentry , it is thought to be due to enhanced automaticity without pathological intra-myocytic calcium spikes (Like true VT )
Absence in surface ECG does not mean it is not existent. In-fact there is some evidence to call this arrhythmia as a form of ventricular parasystole.
Focus of arrhythmia
Since it is a reperfusion arrhythmia it has to arise somewhere from re-perfused myocardium.
The fact that it can occur in both RCA and LCA reperfusion indicate the focus can be in any of the ventricle .
Usually it follows the reciprocal rule of bundle branch block pattern (RBBB in LV focus LBBB in RV focus.)
Septal AIVR can have either RBBB or LBB morphology. Usually left axis is noted .
How to differentiate it from non sustained VT ?
- Ventricular rate in AIVR should be between 60 -110 .(Note -The inherent ventricular rate is 35/mt .There is three fold acceleration )
- Basic idoventricular rhythm is about 35. Three times accelerated
- Characteristically AIVR starts with an escape beat rather than an ectopic beat .
AIVR is common in RCA or LCA reperfusion ?
It is supposed to be more common in infero-posterior MI as sinus slowing is an important predisposing factor for releasing the idio ventricular rhythm.
AIVR after primary PCI
Is not reported much as current interventional cardiologists do not bother much to watch about this arrhytmias
Other causes for AIVR
- Myocarditis.
- Digoxin toxicity
Management
(The commonest issue with AIVR could be . . . Nurses /Fresh interns may mistake it as VT and pressing the false alarm ! )
- Rarely requires treatment .
- Atropine ,Isoprenaline to increase sinus rate.
Posted in cardiology -ECG, cardiology -Therapeutics, cardiology- coronary care, Cardiology-Arrhythmias, Uncategorized | Tagged accelerated idioventricular rhythm, aivr, reperfusion arrhythmias, slow vt | 1 Comment »
What will be the pulmonary capillary wedge pressure ( PCWP ) in grade 1 LV diastolic dysfunction ?
- Significantly elevated
- Marginally elevated
- Usually Normal
- It depends upon age, LA size and LV function.
Answer is 3 . (Of course it depends on 4 ) Normal PCWP is 4-12mmhg
Are these patients with grade 1 LV diastolic dysfunction are at risk for acute pulmonary congestion at times of stress ?
Probably not ( in most )*
The grade 1 LV diastolic dysfunction or defect is the most used (abused ! ) echo terminology .The diagnostic simplicity of this condition namely a simple documentation of “a”velocity more than “e” , has made it as an epidemic in echo labs world wide. After all , it reflects a simple fact that left ventricle has summoned the atria for assistance (Which is all the more physiological at times of stress !)
When does this physiology becomes pathology ?
As long as the atria is doing its job of assisting the LV without any fuss , the mean pressure of LA(PCWP) is maintained within normal level . Only if the atrial function is stretched beyond the limits , PCWP begins to raise. It can happen in a variety of ways . Most commonly it happens elderly hypertensive /Diabetics especially with LVH .
It can also occur in healthy individuals when they become physically deconditioned. (Left ventricle goes for disuse and find it difficult to relax)
Final message
Isolated grade 1 LV diastolic dysfunction in people > 40 years generally do not indicate a serious abnormality.
Only if they have DM/HT and myocardial disease they need to be evaluated further.
One practical clue is , if LA size is normal one can rule out significant diastolic dysfunction.
Caution
* In elderly population , when they undergo any major surgery , presence of even grade 1 LV diastolic dysfunction can be a marker for peri -operative LVF and lung congestion .
Posted in cardiac physiology, Cardiology - Clinical, Cardiology -unresolved questions, echocardiography, Uncategorized | Tagged left atrail pressure in diastolic dysfunction, pcwp in grade 1 diastolic dysfunction | Leave a Comment »
Choosing a pacemaker is not a child’s play . It is a complex game played by cardiologists , electro-physiologists and their ill-informed
patients. The superiority of dual chamber pacing over single chamber pacing was never convincingly proven.
Still . . . usage of dual chamber pacing is steadily increasing over the years for various reasons.
“Every thing hangs around a key word called quality of life . DDD pacemaker is supposed to enrich life due to their AV synchrony “
World health organization says quality of life of homo-sapiens are determined by at least few dozen factors .They are mostly non medical.
How an extra lead at a cost of 2000 dollars more , is going to provide that elusive “quality of life” to all those poor patients with bradycardia in this world , which . . . they any-way lacked even in their best of times !
Scientifically also there is a major flaw in calling DDDR as physiological pacemaker
Posted in Cardiology - Electrophysiology -Pacemaker, Cardiology quotes, medical quotes, Quotes | Tagged choosing a pacemaker, dddr vs vvi paceamker, pathological pacing, physiological vs unphysiological pacing, single vs dual chamber pacing | Leave a Comment »