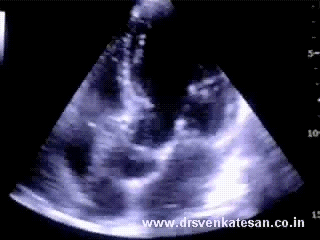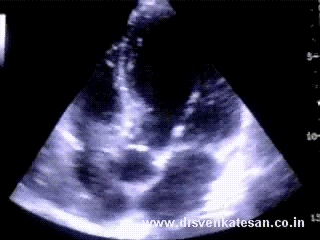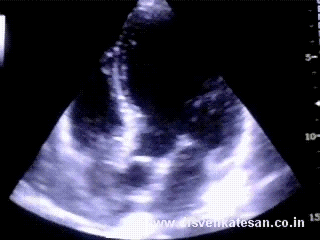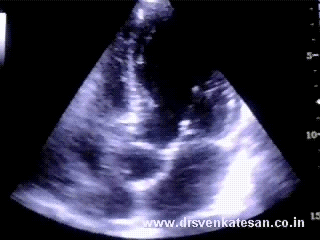
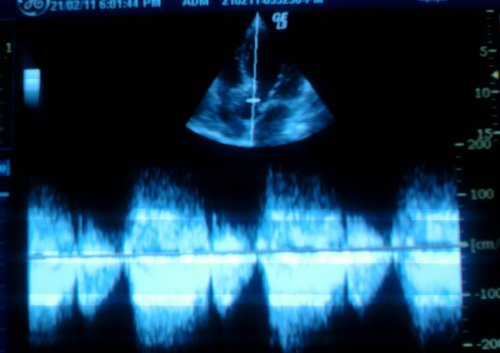
Human atria is a rough terrain infested with peaks and troughs like the Himalayan range . The two atria together has a minimum of ten entry or exit points . Cardiac arrhythmias are something similar to the uneven earth plates triggering an earth quake. Like the earth surface there are areas in the atria with high seismic activity !
It is now discovered there are nine vulnerable points in human atria that can initiate focal electrical activity at times of hemodynamic/ischemic/metabolic stress .
The common causes for Focal /Ectopic atrial tachycardia are
- Hypoxic AT -COPD ( Probably the most common cause .If persistent it will degenerate to MAT- AF )
- Structural atrial disease
- Hypertensive heart
- CAD
- Valvular heart disease
- Drug induced
Note , all these vulnerable points are located either in the junction of an anastomosis with a venous structure or valve or septum.
Further, these sites are often the embryological fusion points making it still more vulnerable due to tissue defects.
Why free wall of atrium is a less common focus ?
They are relatively smooth, lack ridges and joints. Unless the walls of atria are diseased focal tachycardias are less common from these sites .
Other forms of Focal atrial tachycardias
Indian perspective and Rheumatic atrial tachycardia.
In developing countries focal atrial tachycardia in rheumatic heart differ very much from the tachycardia described above. In fact many of the rheumatic atria present straight away to atrial flutter or fibrillation.
Pulmonary vein focus should rarely be considered in atrial tachycardia that occur in RHD.
Post operative tachycardias
Surgical scars can result in what is called Incisional tachycardia.(Especially after complex atrial surgeries like Sennings, Glean/TCPC etc )
Multi focal atrial tachycardia .
This is nothing but a focal tachycardia which tend to fire from different angles towards different targets often lead to a chaotic atrial rhythm . Digoxin and DC shock paradoxically aggravate this arrhytmia.
Atrial epicardium/pericardium interface as a focus
When pericarditis is the predisposing event then it can emanate from anywhere from epicardial surface .
Since left atrium is only partially covered by pericardium it is not logical to assume pericarditis related AT arise from RA epicardium.
Atrial tachycardias in congenital heart disease.
Complex atrial anomalies, SVC type ASDs, PAPVCs can give raise to abnormal electrical focus
Reference
An excellent original work from Royal Melbourne Hospital, Melbourne Australia.
A must read . . . http://content.onlinejacc.org/cgi/reprint/48/5/1010.pdf
//


 t
t