Mystery surrounding the Inherited cardiomyopathies are getting unraveled . Now ,we have a unique entity of cardiac muscle disease due to Desmoplakin mutations which affects the cardiac intercalated disks. They are Naxos disease and Carvajal syndrome.
Heart has a skeleton too
We know skeletal muscles need a bone for its attachment . If we think cardiac muscle can work independently . . . we are mistaken !
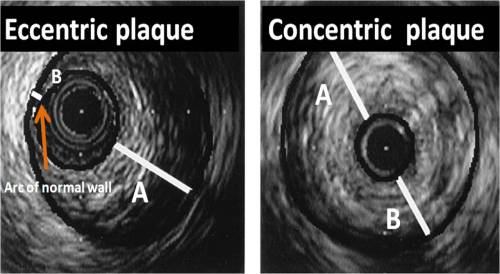
Heart is not a simple mass of muscle.It has a fibrous skeleton around which the muscle is spun around. Myocytes not only need to stick with one another, it has to be packed over the cardiac fibrous skeleton systematically.
The cardiac gums that do this job need to be under strict quality control . After all , these muscle sticking proteins need to be serviced constantly throughout life span of heart. It is simple to understand ,when there is breakdown of this process , protein to protein disconnection takes place . It results in cardiomyopathy.
Thus many of the cardiomyopathies are not primary disorder of cardiac myocytes as such . They can be termed as disorder of myocyte adhesion to cytoskelton.
These present as cardio cutaneous syndromes .(Skin share similar adhesion molecules)
Carvajal syndrome
This is due to mutations of plakoglobin family of protein . Involves desmoplakin , a defective desmosomes and disruption in myocyte adhesion which promote abnormal myocardial stretch , dilatation later fibrosis and progressive cardiac failure. Non compacted LV can be a feature in carvajal syndrome. Recurrent VT/VF demands an early ICD therapy.
Natural history
- Woolly hair at birth
- Cutaneous changes at appear at the age of one year.
- Cardiac involvement occur in adolescence
- Can overlap with ARVD
How is Carvajal syndrome different from Naxos disease.
It has
- Predominant LV involvement.
- Fatty infiltration uncommon
Reference
http://www.ncbi.nlm.nih.gov/pubmed/14761782
http://circ.ahajournals.org/cgi/reprint/116/20/e524.pdf
From cell biology to Inter cellular biology
For over a century biologists were concentrating research inside the human cells .Now we are more interested in the inter cellular planes. It remains an ultimate mystery how the zillions of cells are sticked together in an orderly fashion without fighting each other with a perfect anatomical and physiological harmony.
Understanding the molecular basis of cell adhesion will help us decode the pathological states in which inter cellular disintegration is the hall mark !
A review article on the topic.








 t
t