Medical research can be divided into few broad categories
- Basic science research in animal models
- Basic science research in Human
- Clinical : Bedside- observational
- Clinical: Epidemiological
- Community based long term data analysis
- Interventional -Drug /Device/Surgical
*Logically the top 5 should constitute the bulk of research , in reality last one wins the race with considerable ease . Why ?
The important issues that confront today’s medical research starts right from the “Aim” of the research , methods , materials statistics, and goes on to ethical issues , conflicts, futility , gimmicks 0f publication , marketing and ultimately left for human assimilation .
(Read a related article in this blog can Aim of a study be wrong ?)
Data(s) won’t lie . . .humans do !
Science is nothing but collection of facts , rechecking the facts , and finally confirming , they are indeed facts. So medical data collection becomes vital . Data, if properly collected , wont lie. Bias is always an issue in prospective trials. Further , and whenever and wherever scientifically motivated human beings interact with data the later becomes a vulnerable target and get manipulated for various reasons . (Read the famous article on data torturing in NEJM : I will link it soon ) So blinding becomes mandatory and it should be total as some studies tend to gain vision half way through !

Image courtesey : Jupeter images
Simplicity of observational studies.
We give undue importance to RCTs . What we fail to understand is RCTs are required only in selected situations in medical research (New drugs and interventions ) Meanwhile , we can do wonders with retrospective observational data. These data can not be manipulated as the events have occurred already and those people who collect or record the data wouldn’t know this data is going to be utilized for a study (This , in fact is equivalent to 100 % natural blinding and constitute a real world study )
Observational study can involve patient behavior , disease behavior , community impact, drug action, investigation modality , etc . . .etc . Your mind is the limit . Cost of doing a observational study is less but the impact on the society can be great .
Observing skills are the biggest causality in modern medical times , This was only scientific weapon of our ancestors had , which they used in an exemplary fashion .( Recall how Heberden described angina and Harvey taught us about circulation without even ECG and X RAY chest )
Fraud in medical research
Wherever big money is flowing corruption and fraud is unavoidable . . .at the least . . . we should recognize it
( Many journals just point out this possibility by simply displaying message of conflicts .They do not bother more than that . . . just a warning message )
Now in the modern scientific world , even as the genuine contributions from our ancestors left to stare the back of us , we try to indulge in all sort of unpleasant things.
In an audit against fraud in medical research , it was found most of the fraudulent research happened with drug and device trials and few in basic science involving genetics and molecular medicine . It was rare to identify fraud in research involving purely clinical and epidemiological analysis .
Drug trials need to be prospective . Vested interest can play havoc in prospective data .There is a thing called steering committee in all major studies . . . we do not know what does the word steering really mean .
There has been many occasions even well conducted studies turn out be fraudulent . Now we realise many such studies are struggling to prove its worthiness .
In fact it is argued every study before getting published should undergo a global , independent trial monitoring board for genuineness of the study . (Not the customary peer review !)
Final message ( Sorry its a long one !)
We have a huge problem here . I am afraid we haven’t even understood , what we mean by medical research !
For today’s youngsters medical research means doing sophisticated tests in nano- labs , human genome mapping , space age imaging modalities or involving a multi- billion dolor drug trials . This is absolute falsehood.
What we need to do is “search” , ” search” , search again (That is why it is called re-search ) for all those elusive problems our patients face .Not only in their body , in their home , in their community, etc . Every patient teach us few points, observing and learning new things and publishing is also an important aspect of research .One can do a instant research in the crowded OPD of a hospital , in the wards , (What is the profile of fever pattern in a winter season in your hospital ? does it reveal a new viral epidemic ?)
An ideal research should identify a problem and suggest a practical solution to a given problem .There are millions of such issue waiting for our attention in the bed side. But what is happening currently ? Current medical research is largely direction less , fueled by vested interest , makes sure it avoids all genuine problem areas !
Many studies happen based on flimsy scientific basis .We are still wasting our time to increase human HDL levels. ( Not with standing the famous Torcetrapib fiasco ) .Hundreds of thousand of dollars are pumped into this research even after realising only the endogenous HDLs generated by natural methods like exercise are the really good HDL !)
While we do million dollar research with a dubious risk factor called high sensitive C reactive protein , there is no takers against number one killer disease of human kind namely “The poverty” (WHO ICD codeZ59.5 )*
Let us prey God to instill common sense to all of us . Patients suffer with disease and we suffer from irresponsibility or reduced responsibility ! It makes us happy at-least few forces like Lancet , British medical journal etc are fighting lone war against this ailment medical science is suffering .
*Please note : http://www.icd10data.com WHO labeled poverty as disease many years back without much fanfare ! It is rarely mentioned in any graduate student** medical text in whom our future lies . I do not know whether Wars and terrorist acts been included as disease or not !
**Our students rattle about about the exotic tick borne Lyme disease happening once a year in remote hills , while most will stare blank when asked how to diagnose and treat nutritional anemia with which millions suffer every day !
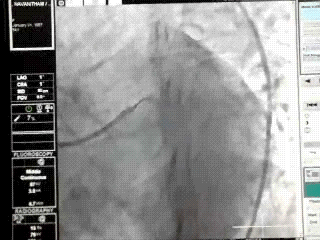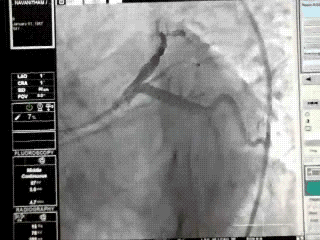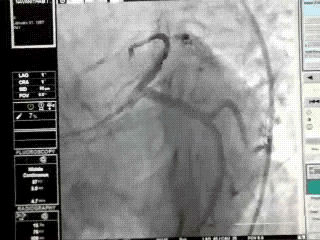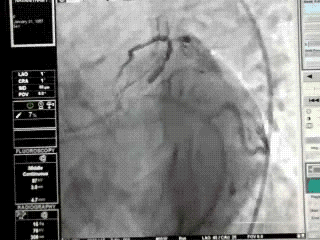
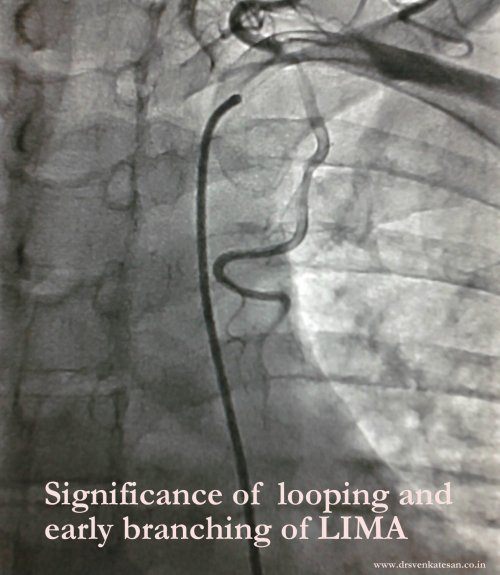
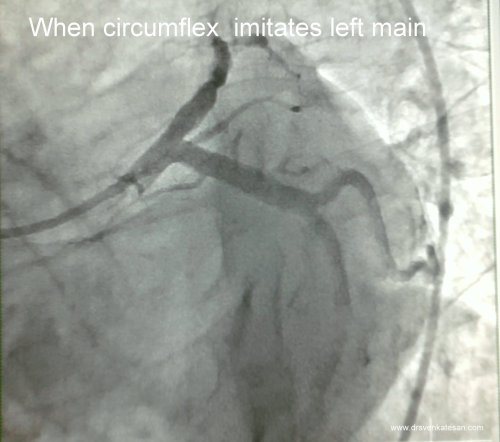 When left circumflex equals the size of left main the pattern is distinctly unusual.
When left circumflex equals the size of left main the pattern is distinctly unusual.