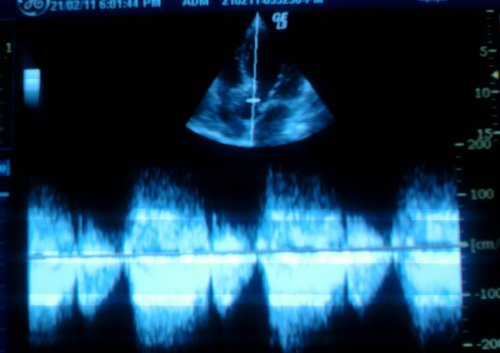
Aortic stenosis is the commonest valvular heart disease in elderly. Severe aortic stenosis requires early aortic valve replacement . Severity of aortic stenosis is best assessed by echocardiogram. ( Cath studies are rarely indicated now) Mean Doppler gradient across the aortic valve (dPm) is the widely used parameter to assess severity.Americans believe in a cut off value of 40mmhg while Europeans want it to be at 50 mmhg . Obviously, these numbers 40/50 become vital as it determines the critical decision of replacing the aortic valve which carries up to 4-10 % mortality.
Even as we realize , Doppler gradients are so important , we also need to know , how fragile ( and vulnerable ! ) are the Doppler equations , especially when it is critically dependent on the angle , flow, heart rate , the LV contractile force and associated MR etc. These errors are over and above the the technical simplification of Bernoulli equation which ignores many accessories like viscous friction , proximal velocity etc .Mind you . . .with this battered Doppler modality we make a critical operative decision !
Here comes the ace . . . Shall we term it as as negligence in clinical echocardiography ?
Apart from the above factors , a single important critical determinant of pressure gradient across AV is the mean pressure in the Aorta itself . The mean LVOT gradient = LV cavity pressure -Systemic blood pressure.Echo derived gradient tells us only the pressure difference across the valve.It does not reveal how much is contributed by raise in LV cavity pressure and how much is contributed by the change in systemic pressure.
How many cardiologists would measure the simultaneous blood pressure while recording LVOT gradient in AS ? ( To be precise it should be measured in the same cycle )
If Aortic mean pressure is high as in systemic hypertension LV pressure must raise considerably higher . The contractile capacity of LV is tested here. A hypertrophied LV easily achieves this. If the LV fails to elevate it’s intra -cavitory pressure sufficiently high the LVOT gradient may never reach the 40 /50 mmhg range that is required to label aortic stenosis as severe.
Many hypertensive patients exactly experience this situation . The left ventricle of many of the hypertensive patients fail this stress test and result in low gradient AS. Note , this happens in spite of having normal EF.
The link between systemic hypertension and aortic stenosis is a complex one. The after load becomes double here.There is a strong vascular valvular interaction. The following effects are seen.
The effect of SHT on AS
It is well known HT initiates the Aortic stenotic process by damaging the valve and also result in progression.
Transient elevation of systolic pressure can result in increase aortic orifice , and a fall in gradient.
The effect of AS on SHT
Once the AS becomes severe , the systolic blood pressure may be reduced. (This not a rule ) If the mechanism of HT is increased vascular tone (Which often is the case ) systolic BP will remain high .
Effect of AVR
Surprisingly , many times the blood pressure normalises after AVR.The mechanism is not known.
Role of Anti HT drugs.
Fixed vasodilators are thought to be contraindicated as sudden fall in systolic blood pressure against a fixed obstruction is detrimental. ACEI may be tried cautiously.(SCOPE AS study )
Reference
The following are the excellent article on the topics .All provided free by the “Heart” Journal
Final message
In the evaluation of Aortic stenosis ignorance continue to prevail over our knowledge. The Gorlin’s the Hakki’s, and the Hatle’s formulas have made the calculation of aortic valve area look like a child’s game (Which is not !)
Referring all patients with a mean gradient > 50mmhg to the surgeon for AVR (or now a TAVI) may be the easiest option for the cardiologists (but definitely not an intelligent one ). Even as we struggle to decode the intricacies of isolated AS , one can guess the complexity when SHT adds on to AS .
Understanding the hemo-dynamics in AS in association with prevailing blood pressure is vital. It is a more scientific way of doing echocardiography . Every cardiologist should give their input as they encounter hypertensive patients with AS.
It would appear , an AS patient developing HT at a later age and a HT patient developing AS later are two different poles in the hemodynamic spectrum.
 t
t