Some say medicine is a funny science . . . it is true at times. It will remain so , as long as we convert a fact into a myth and a myth into a fact at our convenience . It is often fueled by the whims and fancies of modern research ! This phenomenon is happening in a regular fashion for many decades now.
The number one killer disease of heart is the atherosclerosis . Atherosclerosis means hardening of arteries. The advent of coronary calcium score with CT scans , it became a craze among many physicians . (It was replaced later by 64 /128 slice MDCT with unprecedented commercial over tones !)
How can we conquer the atherosclerosis ? when the enigma of calcium in coronary artery is yet to be solved.
The next few decades will be crucial as we are trying to find answer to the following question .
Is coronary calcium good , bad or neutral in CAD ?
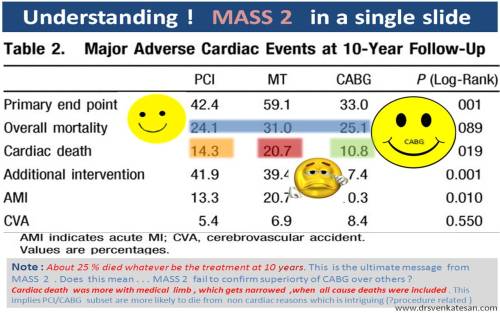
This article in American journal article begins the new year 2011 with good news for people , who show some calcium in their plaques.
What makes a plaque vulnerable ?
Plaque contents , it’s distribution and consistency make it vulnerable. Soft spots formed by lipids may result in plaque cracks and fissure. Semi solid , mixed , gel like soft plaques are dangerously prone for rupture . Oxidation of LDL, LDL liquefaction and tissue metalloprotinase , thickness of fibrin caps , all promote softening. If none of above mechanism is operative in a given patient , the plaque becomes stiff and hard.
Calcification is the ultimate in hardening . Calcified plaque is resistant to mechanical deformation.If stiff plaques are less vulnerable , hard plaques ( ie calcified plaques ) must be least vulnerable . Calcification can be called an end result of coronary atherosclerosis.
So , calcified coronary artery can be referred to as a failed mission of atherosclerosis .It is equivalent to death of atherosclerosis and denotes the end process of this dreaded disease process.
Calcification tames atherosclerosis in it’s own den
What is the implication of a stiff hard, sharp calcified plaque lining (or even projecting ) in the coronary lumen ?
As this study has shown , calcium in the walls of coronary artery is innocuous . Of course , calcium should not be dense and obstruct the blood flow . This will require intervention. Many consider , calcium as a foreign body in the coronary artery . But the prevalent understanding is , presence of non obstructive calcium is often a non issue or in fact a welcome issue in some.
After all , millions of human beings happily roam around with the hardest possible substance lining their coronary artery called stents.
Caution about calcium
This article does not portray calcium as a healing molecule in CAD . In the realistic senseit is too complex to make such a generalization. The message is , calcified lesions are less likely to result in acute coronary events than soft , non calcified lesions.
It is well known , calcium can be problematic for the interventional cardiologists .It makes life tough for them in deploying stents. Calcium rich lesions exerts radial force in a diagonally opposite direction and interferes with stent approximation.
It is also believed localised , sharp calcium crystals may tear a plaque and cause plaque dissections. This happens if the calcium is lying in an eccentric fashion overhanging the shoulder region of the plaque abutting a soft spot.
Final message
It is now clear , why calcium score in CT scans failed miserably to predict high risk subsets of CAD. In spite of repeated studies the researchers failed to show a positive correlation . The studies are flawed as they were trying to look for a positive correlation which is non existent . In fact , the above study seems to suggest calcium score may indeed predict low risk individuals!









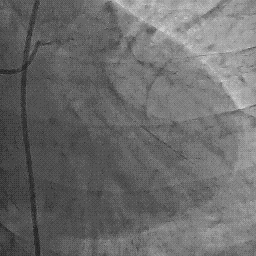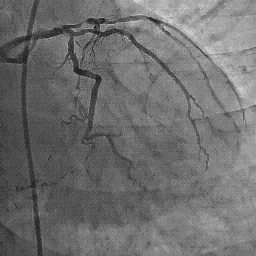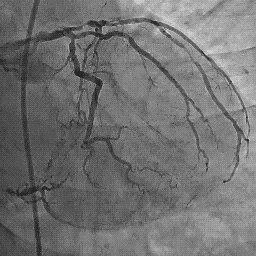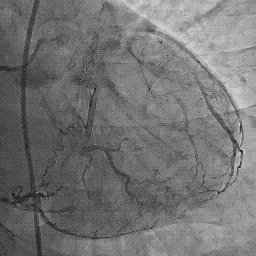
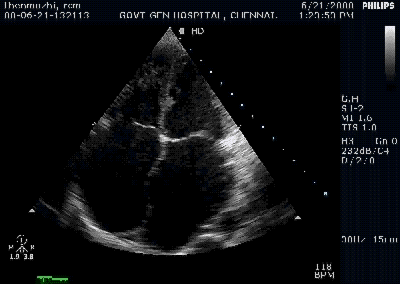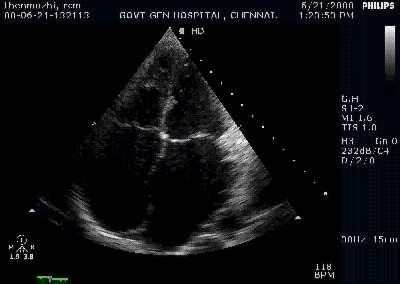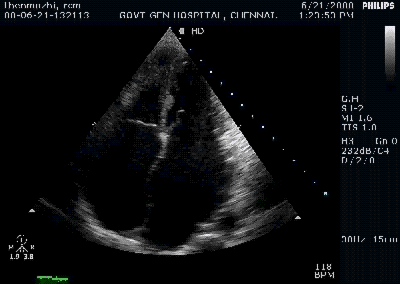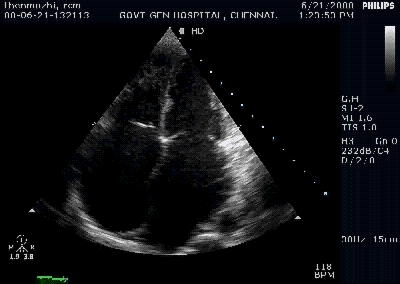 y
y