October 9, 2008 by dr s venkatesan
During acute ischemia the most immediate requirement for the heart is
A.Blood
B.Oxygen
C.Glucose
D.High energy ATPs
E.Free fatty acid
Answer : A will be considered by most , as correct answer . A can provide B to E . But it is also a fact heart can survive without A.
Myocardium requires energy first ! it does not in fact bother about from where it is coming at the time of crises.It may be right if you restore the coronary blood flow all other components (B-E) are made available to the heart .
The heart can survive off the coronary circulation with only chemical support during cardiac surgery and also a during heart transplantation explanted donor heart survives on a ice box during transit and till it is transplanted into the recipient heart
But ironically we spend much of our energy and efforts in restoring blood flow.One need to spare a thought about the quality of blood also . This is especially important in the setting of ischmia where a metabolic centric approach will add further benefit.

Energy based approach to ischemia : Is it relevent ?
Heart is a fascinating mechano biological organ pumping millions of gallons of blood .Fuel for this is self generated on a continuous basis from the circulation blood .So the key to human survival is the coronary blood flow that supplies the fuel and nutrients to the heart. When this key supply line is under threat during acute coronary syndrome cardiologist have the only option of restoring the compromised blood supply by any means . But during chronic ischemia there is no urgency. There has always been an option of enriching the blood with energisers like ATPs, glucose, hemoglobin etc .Providing energy support to the failing heart has never captured the imagination of cardiac physicians until recently.Still most are skeptical about the concept of biochemical ischemia.
Click to download full PPT presentation
Metabolic manipulation of CAD( Will be available shortly)
Posted in Cardiology - Clinical, Cardiology -Interventional -PCI, cardiology -Therapeutics, cardiology- coronary care, Infrequently asked questions in cardiology (iFAQs) | Tagged acs, angina, atp, biochemical ischemia, cardiac failure, chronic stable angina, coronary, fatty acid, glucose, ischemia, ketoacid, metabolic modulation, mitochondrial energetics, myocardial energetics, ranalozine, trimetazidine, unstable angina | Leave a Comment »
October 9, 2008 by dr s venkatesan
Humans have roughly 5 to 6 liters of blood at any given time in their body . Out of this*
50% (2500ml) is located in the systemic venous compartment.
18% is within the pulmonary circulation participating in the vital oxygenation
12% (500-600ml) is within the cardiac chambers.
8% is in the arterial tree of the body.
5% is within the capillaries.
2% is in the aorta.
* Source : Best & Taylor Physiological basis of medical practice 1966, 8th edition
What is the implication of this predominantly venous distribution of blood at rest ?
- A competent venous tone is essential for the human beings to maintain the erect posture.
- Bulk of the cause of syncope in humans is due to peripheral mechanism like loss of vascular tone and resultant venous pooling.
- The concept of venous reservoir is so important in emergency situations like hypotension as simple elevation of legs is equivalent to infusing 500 -800 ml of intravenous saline .
- Similarly during acute left ventricular failure trunk elevation and legs dangling down can reduce the pulmonary congestion very significantly and reduce pulmonary capillary wedge pressure (LVEDP)
Autonomic dysfunction and venous insufficiency
Autonomic dysfunction and resultant orthostatic hypotension is directly related to venous reservoir dysfunction.Increasing effective circulatory volume by elastic stockings or administration of mineralocorticosteroids like fludrocortisone (.5mg/day ) can be useful in this condition
Posted in Cardiology - Clinical, cardiology -Therapeutics, Infrequently asked questions in cardiology (iFAQs) | Tagged autonomic dysfunction, blood volume, bmj, capillary, cardiac output, cardiology, drsvenkatesan, effective circulatory volume, fludrocortisone, heart, Hemodynamics, lnacet, lvedp, nejm, ortho static hypotension, pcwp, physiology of circulation, pulmonary edema, syncope, venous circulation, venous insufficiency, venous pooling | Leave a Comment »
October 9, 2008 by dr s venkatesan
Glucose is the molecule of life ,burnt every second inside the body at the energy store house called mitochondria. Heart , the most active organ in the body gets bulk of it’s energy supply from fatty acids, glucose and a little from keto acids. Under anerobic conditions this energy substrates shifts towards glucose .
We are rarely inclined to think that heart can ever suffer from hypoglycemia ! But hypoglycemia can have distinct direct and indirect effects on heart. In fact indirect effects due to activation of adrenergic activation is more obvious.An episode of hypoglycemia can precipitate an arrhythmia . Glucose potassium insulin infusion




Final message
Hypoglycemia , can be a trigger of ACS .This aspect is poorly recognised and studied.
Posted in Cardiology - Clinical, cardiology- coronary care, Infrequently asked questions in cardiology (iFAQs) | Tagged acs, acute coronary syndrome, angina, cardiac arrhythmias, cardiology, diabetes mellites, drsvenkatesan, hypoglycemia, jama, lancet, nejm, tiggers | 1 Comment »
October 7, 2008 by dr s venkatesan
Ventricular fibrillation is invariably fatal if not treated . When can atrial fibrillation be fatal ?

Atrial fibrillation is relatively a benign arrhythmia especially when it occurs in isolation with structurally normal heart.This is sometimes referred to lone atrial fibrillation . Even otherwise, atrial fibrillation is rarely fatal except in few situations.But AF commonly destabilises the patient who have baseline valvular or myocardial disease.(Post MI, dilated cardiomyopathy etc)
There are few situations where AF can be life threatening
- In patients with WPW syndrome*where , AF enters into a electrical short circuit , downhill to enter the ventricle and make it fire at the same rate as that of atria . ( ie 400-600) and result in ventricular fibrillation.Note , even here it is the VF that kills not , AF per se.
- AF in acute MI often precipitates LVF , but rarely fatal.
- In patients with critical aortic stenosis, or hypertrophic cardiomyopathy, sudden onset of AF can result in acute cardiac failure.
- AF is often a terminal event in primary pulmonary hypertension
While atrial fibrillation is less likely to cause death , it is a highly morbid arrhythmia .It is one of important cause of stroke in elderly as well as young !
Posted in Cardiology - Electrophysiology -Pacemaker, Infrequently asked questions in cardiology (iFAQs) | Tagged atrial fibrillation, cardiac arrhythmia, cardiology, drsvenkatesan, ECG, electro physiology, heart rhythm, nejm, pace, ventricular fibrillation | 1 Comment »
October 6, 2008 by dr s venkatesan
 Usually in the the vascular system both artery and vein go together .It is an irony in pulmonary circualtion these two never go together .Another paradox is that pulmonary artery carries the most deoxygenated blood and pulmonary vien carries the purest form of blood in the entrie body , probably God has kept them widely seperated as communication between them seriously affect the physiology.
Usually in the the vascular system both artery and vein go together .It is an irony in pulmonary circualtion these two never go together .Another paradox is that pulmonary artery carries the most deoxygenated blood and pulmonary vien carries the purest form of blood in the entrie body , probably God has kept them widely seperated as communication between them seriously affect the physiology.

Posted in cardiology-Anatomy, Infrequently asked questions in cardiology (iFAQs) | Tagged pulmonary artery, pulmonary vein | Leave a Comment »
October 3, 2008 by dr s venkatesan
Ventricular tachycardia is considered as one of the most dangerous cardiac arrhythmia .Rather , it is the label VT that spreads more fear than the arrhythmia itself. It is a fact many patients with VT walk into hospital , still VT will always be a sinister arrhythmia as long as it carries a risk of degenerating into ventricular fibrillation.
What determines hemodynamic stability in VT ?
- Origin and location of VT
- The ventricular rate
- Presence or absence of AV dissociation
- Impact on mitral inflow pattern
- Associated left ventricular dysfunction or valvular heart disease.
- VT in the setting of acute coronary syndrome.(Ischemic VT)
- Inappropriate drug selection
Origin and location
VTs originating high up in the ventricle( High septal VT,Proximal VTs) have more organised ventricular contraction and they are more stable.Distal VT originating in the myocardium away from the conducting system has chaotic myocyte to myocyte conduction.These are very unstable.
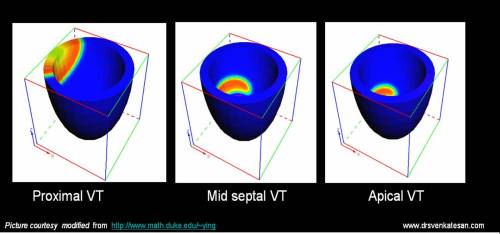
The term fascicular VT is nothing but VTs originating in the His bundle and it’s branches( Can also be termed Septal VT ).These VTs are also stable and some of them respond well to calcium blockers indicating that they are very close to the AV junction and carry the properties of junctional tachycardia. QRS width gives a rough estimate about the location of VT. Narrower the VT higher it’s origin.( But remember even in VT , qrs can further widen on it’s way downhill !)
LV dysfunction.
This is probably the most important determinant of the outcome in VT. Patients with severe LV dysfunction (EF <30%) fare badly .Hence the land mark concepts from MADIT 1& 2 demanded ICDs in these patients.The most common clinical setting is dilated cardiomyopathy.SomE of them have bundle branch re entry(BBR).This particular VT can be stable for many hours.
Ventricular rate.
Usually VT has a rate between 120-200.Higher the rate of VT more the chances of instability .This rule is also not always true as fascicular VT can be well tolerated at high rates.So location of VT focus and LV dysfunction usually over rides the impact of ventricular rate.
Mitral inflow pattern
Proper left ventricular filling is the key to hemodynamic stability in VT. In proximal, septal,fascicular, LVOT VTs doppler studies suggest (ACC /AHA Type C evidence : Personal observations in CCU during VT) near normal preservation of bi modal filling of mitral valve inflow.In ischemic myocardial VT the mitral inflow profile is critically affected . There is no distinctive forward filling was observed .In fact at rapid rates a short pulsatile MR jets are noted instead.
Associated valvular diseases
It is obvious, aortic and mitral valve disorders can aggravate the hemodyanmic instability.
Final message
The clinical behavior of ventricular tachycardia is widely variable and dependent on multiple factors.
Associated LV dysfunction and structural heart disease ultimately determine the outcome.
Posted in Cardiology - Electrophysiology -Pacemaker, cardiology- coronary care, Infrequently asked questions in cardiology (iFAQs) | Tagged bmj, fasicular tachycardia, heart rhythm, Hemodynamics, ischemic vt, jama, lancet, lvot vt, myocardial VT, nrjm, pace, ventricular tachycardia, verapamil sensitive vt | Leave a Comment »
October 3, 2008 by dr s venkatesan
Even as cardiology community is preoccupied with systemic hypertension & CAD , pulmonary arterial hypertension(PAH) is a much neglected , still an important clinical cardiac problem encountered . The irony is self evident , there are half a dozen methods to grade systemic hypertension not even a single stadardised grading available for pulmonary arterial hypertension. The WHO working group defined pulmonary hypertension few decades ago and was not clinically graded .The only grading available is based on the pulmonary vascular biopsy changes (Heath Edwards)
Currently PAH management has gone through revolutionary changes. There is an urgent need for grading this entity .This will facilitate to diagnose , manage and assess the efficacy of the currently available treatment.
Developing countries like ours have a great number of PAH due to rampant rheumatic heart disease. A simple study was done in 100 patients with PAH .Bulk of the study population had RHD .Few had primary pulmonary hypertension .Systolic , diastolic, and mean pressure was assessed by doppler echocardiographic analysis of tricuspid regurgitation (TR) and pulmonary regurgitaion(PR) jets. TR jet provided the systolic PA pressure , PR jet provided mean as well as diastolic PA pressure .TR jet was available in all patients. PR jet was available only in 60 patients .Hence the diastolic andmean PA pressure data has been extrapolated in some and was plotted in a scatter diagram. Five equal quintiles were divided. Patients in first and 2nd quintiles were graded 1 and third and 4th quintile were graded 2 , 5 th was graded 3 respectively. From this cut off points for various grades of PAH were identified .The top 3% of patients with highest PAP were graded as grade 4 and all of them had supra systemic PAH.
The following grading is suggested for PAH*
 *This is a preliminary attempt to grade PAH. This could be applicable mainly in rheumatic heart disese and primary pulmonary hypertension .Further refining of methodology is required.PAH grading may be little different in congenital left to right shunts.
*This is a preliminary attempt to grade PAH. This could be applicable mainly in rheumatic heart disese and primary pulmonary hypertension .Further refining of methodology is required.PAH grading may be little different in congenital left to right shunts.
Posted in Cardiology - Clinical, Infrequently asked questions in cardiology (iFAQs) | Tagged annals of internal medicine, bmj, cardiology, chest, drsvenkatesans, eisenmenger, grading of pah, grading of pulmonary hypertension, jama, lancet, lungs, mitral stenosis, nejm, pah, pulmonary arterial hypertension, pulmonary hypertension, rabinovitch, rubin | 1 Comment »
October 2, 2008 by dr s venkatesan
Palpitation is one of the common symptoms for which cardiac patients are referred. Like dyspnea , palpitation can either be a physiological expression of normally beating heart or a dangerous pathological state of the heart. This makes this symptom unique and warrants careful evaluation.  By definition palpitation is abnormal awareness of ones own heart beat. Heart is a mechanical organ with multiple mobile anatomical structures. There is constant blood flow in multiple directions . Apart from this the heart has it’s unique translational, rotational movement . These intrinsic movements combined with proximity to chest wall generate vibratory motion signals .These signals are generally dampened by the encircling pericardial space .The neural signals responsible for perception of palpitation is not clear. If the heart hits against the chest wall it is the somatic nerves from the chest wall that carries the signal. Vibrations generated within the heart chambers, and and the valves are carried by the myocardial and intravascular sensors.( Autonomic)
By definition palpitation is abnormal awareness of ones own heart beat. Heart is a mechanical organ with multiple mobile anatomical structures. There is constant blood flow in multiple directions . Apart from this the heart has it’s unique translational, rotational movement . These intrinsic movements combined with proximity to chest wall generate vibratory motion signals .These signals are generally dampened by the encircling pericardial space .The neural signals responsible for perception of palpitation is not clear. If the heart hits against the chest wall it is the somatic nerves from the chest wall that carries the signal. Vibrations generated within the heart chambers, and and the valves are carried by the myocardial and intravascular sensors.( Autonomic)
What are causes of palpitation?
Cardiac
- All hyperdynamic circulatory states. It may be generated from either right or left ventricle or both.
- Regurgitant lesions ( Mainly Mitral and aortic regurgitation)
- MVPS*
- Congenital heart disese ( Mainly left to right shunts-ASD/VSD/etc)
- Apart from this patients with prosthetic heart valve, and pacemaker patients can feel their heart beats.
- Cardiac arrhythmia .Both tachycardia, and bradycardia . Ventricular ectopic beats are the very common cause .( It is often described as missed beat)
* Mitral valve prolapse, a very benign condition, over diagnosed in the last few decades raised considerable anxiety and palpitations for the patients (mainly after the diagnosis ! ).Now the cardiology community has sought to underplay this entity with strict diagnostic criteria.( Thickened mitral leaflet ,presence of MR both must be present to label a patient as MVPS)
Non cardiac
- Physiological
- Anxiety state
- Anemia
What is the relationship between ejection fraction and palpitation?
What is the significance of palpitation that occur during rest ?
Palpitation occurring at rest indicate more often a pathology.It is invariably due to an cardiac arrhytmia either tachycardia or bradycardia. Intelligent patients can give accurate information about the regularity of rhythm , any extra beats or missed beats . Atrial fibrillation, VPDs could be diagnosed by history alone in them !
If palpitation is associated with visible chest pulsation what is the likely diagnosis ?
If significant visible pulsation over chest wall pulsations are seen in young adults it could simply mean a hyper dynamic circulation and thin chest wall. Pulmonary arterial pulsations is not normally felt in left 2nd inter costal space.If felt one has to rule out shunt lesions like ASD or pulmonary hypertension.
“ASD is the commonest cause of right ventricular palpitation “
Posted in Cardiology - Clinical, Tutorial in clinical cardiology | Tagged anxiety state, asd, bmj, bradycardia, cardiology, clincal cardiology, drsvenkatesan, hyper kinetic circulation, lancet, nejm, palpitation, Tachycardia | Leave a Comment »
October 2, 2008 by dr s venkatesan

Amlodipine , the most popular anti hypertensive drug used world wide has an very important action on coronary blood flow.When nifedipine was introduced three decades ago it was known for it’s powerful anti anginal properties. Subsequently amlodipine was introduced with almost similar action. But over the years, amlodipine was projected primarily as anti hypertensive drug and gradually many of the physicians are made to believe it is a drug that should be used only if the blood pressure is high.The fear of reflex tachycardia in few was exaggerated.
In fact a cross section of today’s general physicians were queried about amlodipine and none of them acknowledged using this drug as an anti anginal drug. And few of them went to the extent of withdrawing amlodipine if it was used for the purpose of angina relief !
Why amlodipine’s anti anginal action is in doldrums ?
The single word answer is unfortunate! Marketing bias ,coupled with the fact that mainstream cardiology texts have ignored this aspect.
Final message
Amlodipine , can still be used as a antianginal drug especially in a patient who has angina with associated bradycardia , significant LV dysfunction . Some reserve amlodipine and nifedipine exclusively for vasospastic angina where beta blockers alone are theoretically contraindicated .
Posted in Cardiology - Clinical, cardiology -Therapeutics, Infrequently asked questions in cardiology (iFAQs) | Tagged amlodipine, amlogard, angina, beta blckers, bmj, calcium channel blockers, cardiology, chronic stable angina, diltiazem, drsvenkatesan, jama, lancet, nejm, nifedipine, prinzmetal, unstable angina, vasospastic angina, verapamil | Leave a Comment »
October 1, 2008 by dr s venkatesan
.

It is a well known fact squatting is a simple compensatory posture adapted by children with cyanotic heart disease during exertion to get relief from breathlessness. The children with tetrology of Fallot and related conditions have baseline hypoxia due to right to left shunting .This gets aggravated during exertion. Squatting promptly relieves this exercise-induced worsening of dyspnea. The oxygen saturation improves immediately after assumption of squatting posture. The exact mechanism by which squatting relives the dyspnea is not clear.
Apart from squat induced po2 raise there is a fall in the concentration of pco2 and raise in blood Ph that pacify the sensitive respiratory centers,thereby bringing down the tachypnea

Hemodynamics of squatting has two phases
- Immediately ( First 15 seconds) after squatting there is a sudden drop in venous return.
- Sustained squatting for 1-2 minutes result in steady increase in venous return, raised systemic vascular resistance.

Both these effects help the children with TOF. The initial trapping of highly desaturated blood in the lower extremity gives a quick relief as soon as the child assumes this posture. In the next 15 seconds or so the systemic vascular resistance increases and bring the aortic after load sufficiently high to divert the blood into the pulmonary artery.
The net effect of squatting is there is a transient or sustained (as long as child squats) increase in pulmonary blood flow and this is made possible by the relative reduction of right to left shunt as the aortic and systemic resistance is raised by this posture.
Other explanations
There is one more possible effect of squatting. By, compressing abdomen (Knee chest) cause a mechanical push on the splanchnic blood pool into the aorta which has high o2 saturation. This is thought to provide immediate relief to brain hypoxia and avoid the vicious respiratory/ hemodynamic cycle
What is the clinical inference from squatting in cyanotic heart disease?
Squatting implies there should be a large VSD, associated with a delicate right to left shunting very much dependent on the degree of pulmonary stenosis or ( any RVOT obstruction) and the systemic vascular resistance.
How common is squatting history in pulmonary atresia with VSD ?
It can occur with collaterals are sparse.The mechanism of relief is slightly different.
The likely mechanism of relief with squatting in Pulmonary Atresia, VSD is two fold.
1. The Initial relief is due to trapping of deoxygenated venous blood in squat posture, which is similar to TOF
2.The sustained benefit is due to raised systemic vascular resistance which favors more flow across MAPCAs from Aorta.
The second one has no authentic reference , but its a hemodynamic plausiblity as there is zero RVOT flow in PA with VSD.
What are the other cyanotic heart diseases in which squatting is reported ?
- Tricuspid atresia
- Double outlet right ventricle with pulmonary stenosis
- Any combination of large VSD and RVOT obstruction
- Rarely in Eisenmenger syndrome*10%)
*Mechanism of squatting episodes in Eisenmenger is tough to explain. But, it does give relief. The most plausible mechanism is the raise in SVR with squatting tilts temporarily a favorable QP/QS as PVR -SVR ratio falls .(Venous return component doesn’t operate here as in squatting of TOF) It should be noted squatting is mainly reported only in VSD Eisenmenger.. ASD/PDA -Eisenmenger is extremely rare or doesn’t occur. This is understandable as Interventricular communication has to be present to shift in QP/QS with a response to a rise in SVR.
Squat equivalents
Assuming a squat position has cultural issues. Grown-up children may avoid these public places. Standing with legs crosse is a common posture. In fact, the mother holding a crying baby in a chest with knees folded promptly prevents a spell . This can be called “squatting by proxy”
*Though squat equivalents do give relief from dyspnea they are given less significance in terms of diagnostic value of TOF
Reference
1.Paul R. Lurie ,Postural effects in tetralogy of Fallot The American Journal of Medicine Volume 15, Issue 3, September 1953, Pages 297-306
2. Warren G. Guntheroth. M.D.Beverly C. Mortan. m.Venous return with knee-chest position and squatting in tetralogy of Fallot American Heart Journal Volume Volume 75, Issue 3, March 1968, Pages 313-318
Posted in Cardiology - Clinical, Infrequently asked questions in cardiology (iFAQs), Tutorial in clinical cardiology | Tagged cardiology, cyanotic heart disease, drsvenkatesan, heart, how does squatting help in eisenmenger syndrome, lancet, mechanism of squatting in Eisenmenger, nejm, squatting, squatting in vsd asd pda eisenmenger, tetrology of fallot, ventricualr septal defect | 2 Comments »
« Newer Posts - Older Posts »
















