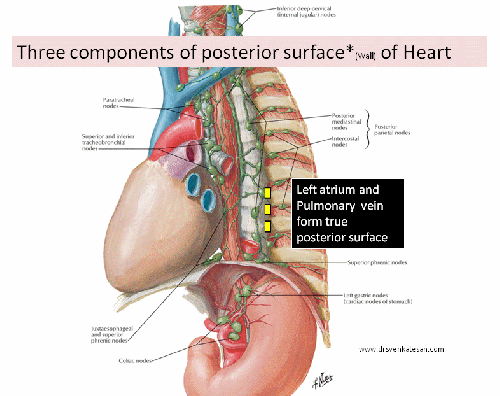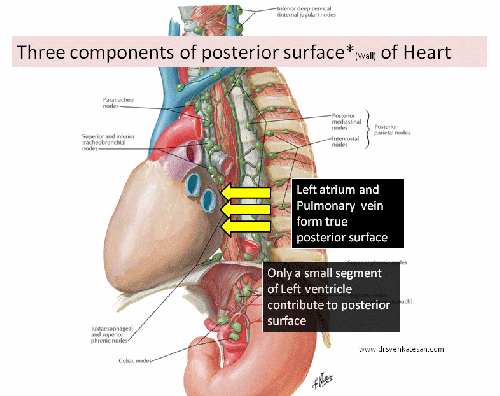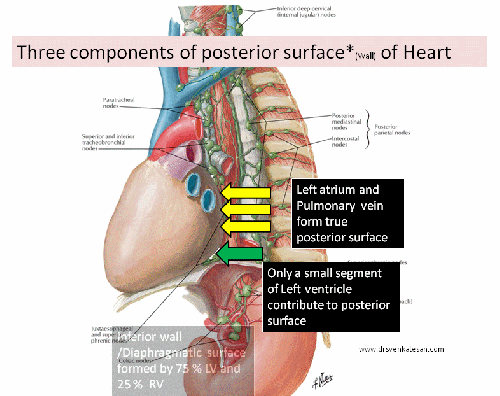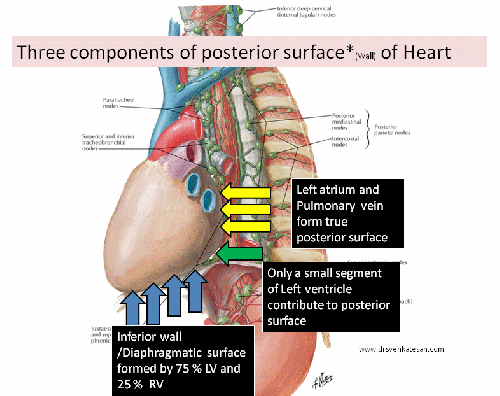
BMS, the original stent technology with meticulous metallurgy and design has been silently replaced by the drug eluting stent (DES) for over a decade. DES was introduced to bail out BMS from perceived high rates of restenosis . It was a fundamental flaw, we failed to give due weightage to the multiple variables like operator expertise, lesion morphology, patient factors that determined the restenosis rate .
There was never a single study done in large scale that compared a well deployed BMS with a poorly deployed BMS/ DES in terms of restenosis rate.This would have clearly quantified the technical component in the restenosis rate that brought pseduo -bad name for BMS in early days.
Without applying mind, wrong questions were asked and tested. No body could refute a “novel concept” , when some big names in industry suggested we must involve an anti cancer drug to prevent cell growth and neo-vascularisation and hence restenosis. But , in reality the technology of DES essentially complicated the metal behavior by adding a drug and drug adhesive agent(Polymer) to the otherwise inert metal. Further , the , metallurgy engineers had to restart / reduplicate from the scratch since we had already well developed stent technology for BMS . The manipulation was to add a drug to the metal.
The irony of DES lies in the fact it Intentionally allowed to interfere /damage the endothelial healing and make the extended anti-platelet mandatory. Still , DES was able to rule the world backed up by hyped data with bloated reduction in restenosis rate. (Now we realise the true benefits of DES are nil or at best marginal or even harmful in certain subsets of ACS .Read NORSTENT Trial linked below )
Yes DES has a concern , but its not the drug you know !,
Off late , since the polymer was assumed as culprit, variety of new generation stents with disposable /Non durable /Zero poylmer were developed. Still, polymer could not be proven as true culprit , some have started blaming the drug again. Recently, It led to one famed DES based on Paclitaxel (which has a pride of place in the Land mark SYNTAX study ) exited the human domain with disgrace . (I wonder can we conclude then SYNTAX study is also become invalid !)

This study done with over 9000 patients concluded like this . . .

The DES industry was (is) so powerful it could easily shrug the challenge of truth that came out briefly in early 2000s when DES got hit with increased acute complications.
Now, in 2016 NORSTENT study again showed us BMS is as good as DES in all walks of CAD. Let us see what happens , still its very unlikely mature cardiologists do not trust BMS.
*I have a belief (Paranoid or not time will tell !) one of the reasons DES are strongly promoted is to sustain DAPT market alive and kicking for a long haul !
Scenerio in India is frightening.
While the developed countries have DES usage rate around 65 % , India leads the world with DES constituting 95% (NIC registry 2017) of all deployed stents.What a way for a poor country to tackle CAD , which doesn’t even have prompt prehospital Aspirin for bulk of their ACS patients, ready to waste its resources in DES.

India , a country Infested with an unregulated health industry became the perfect battle ground for abusing the stents. With direct collusion with the large hospital managements the issue got exploded recently .The Govt was compelled to come out with urgent restrictions and price control in the use of stents.
Funny world this. World’s richest economies are worried about the cost and want to phase out inappropriate therapy whenever possible, its absolute arrogance most of us feel shamed to keep BMS in their cathlab.
Final message
A good metal based flexible ,trackable , thin struted BMS should be the default choice for coronary stenting .( We used have one , now it vanished !)It avoids unnecessary prolonged DAPT .Most importantly one BMS costs 25 % of the cost of DES . . . think of 4 critical proximal LAD lesions of a poor man can be fixed at the cost of one DES , that’s definite way forward. Govt of India can pass another regulation in this regard. If you think NORSTENT is NONSENSE let us atleaset insist for a large scale Indian study for BMS /DES and Cardiological society of India has much work to do !
Future for BMS . . . looks bright !
While the superiority of DES is being increasingly questioned , the concept of surface modified BMS is being tested .This I believe is a face saving way to bring back the BMS in lieu of DES. There is a distinct possibility of many of the new generation DES going the BVS way in the near future.
Reference
1.Hassan AK1, Bergheanu SC, Stijnen T, van der Hoeven .J Late stent malapposition risk is higher after drug-eluting stent compared with bare-metal stent implantation and associates with late stent thrombosis.Eur Heart 2010 May;31(10):1172-80.
2.Zhang K1, Liu T, Li JA, Chen JY, Wang J, Surface modification of implanted cardiovascular metal stents: from antithrombosis and antirestenosis to endothelialization.J Biomed Mater Res A. 2014 Feb;102(2):588-609.
3. https://www.pcronline.com/eurointervention/114th_issue/volume-12/number-17/350/ultra-hydrophilic-stent-platforms-promote-early-vascular-healing-and-minimise-late-tissue-response-a-potential-alternative-to-second-generation-drug-eluting-stents.
4.Drug-Eluting or Bare-Metal Stents for Coronary Artery Disease NORSTENT Investigators N Engl J Med 2016; 375:1242-1252
Post-ample : Only For non believers ( who think this article is near rubbish )
I am very much convinced DES should be superior for the simple reason it elutes a drug and the whole world believes it works !
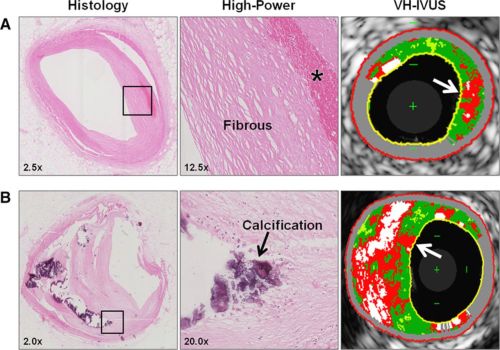
Do you know, what these drugs do, and what they are expected to do ! In this elegant study by Hassan AK1 Eur Heart J. 2010 May;31(10):1172-80. Its proven with IVUS , DES is many fold likely to cause late stent apposition than BMS.( Thus carrying the risk long term ) Reason is simple , patchy and incomplete endothelisation on the luminal side and pathological metal vessel wall interface in abluminal promoting late mal-apposition.