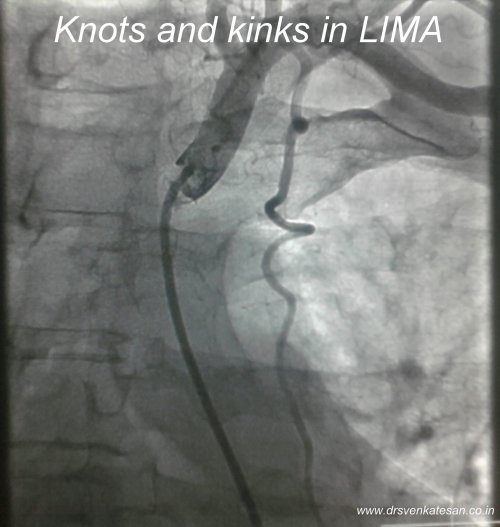
Can you diagnose inferior MI with poor R waves ?
No , you need a “Q ” that’s for sure ! Do not diagnose inferior MI without a q wave . ( The luxury of diagnosing MI without q waves is available only for LAD region )
Any axis deviation ( even 30 degrees) from base line can alter the inferior lead qrs morphology to a great extent. R wave amplitude is primarily determined by the initial septal depolarisation . So if the inferior septum is intact it will never allow to inscribe a q wave . Further , limb leads are bi polar leads and they are sum-mated potential reflected along the entire bottom half of the torso . Hence it is not reliable to attribute significance to presence or absence of r wave (Unlike chest leads).
The lung and diaphragm exert not only electrical insulation but also mechanical alteration of septal profile with phases of respiration.
Counter point
Not really . . . you do not need a Q waves to diagnose inferior MI , electrically diminutive R is same as “Q”
There is an alternate way of reasoning too . R wave is muscle , We diagnose LVH with tall R waves so muscle loss should be equivalent to R wave loss .We have innumerable examples where low voltage R waves are recorded in inferior leads after a well documented inferior MI.
How do you diagnose old inferior MI by ECG ?
- Near normal ECG with degeneration of q waves and regeneration* of R waves
- Residual T wave inversion
- Simple low voltage inferior leads
- Slurred or notched qrs complex in 2 3 AVF
- Rarely with atrial abnormalities and AV nodal prolongations
The concept of regenerated R is well established . And it brings to the age-old debate of R with live muscle Q is dead muscle
Regeneration is salvaged muscle (Natural salvage , awakening from hibernation etc)
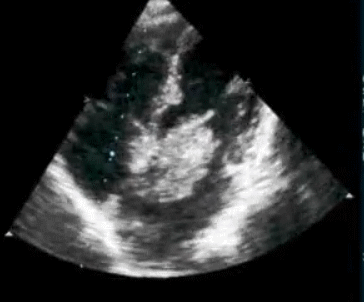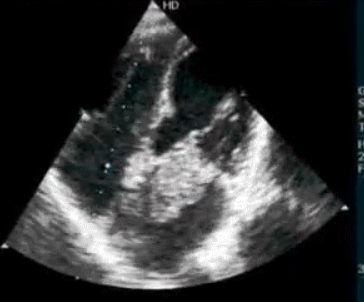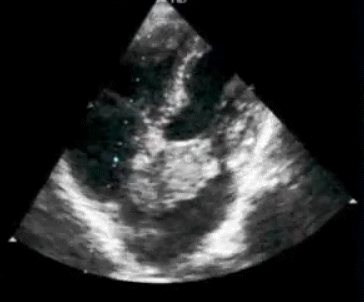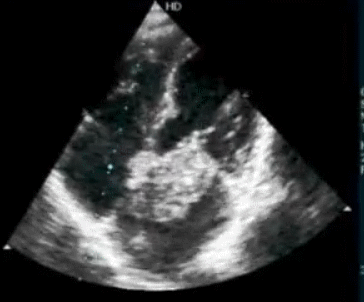
How good is Echocardiogram in diagnosing old Inferior MIs ?
Surprisingly , echocardiography do not help much either .Technically inferior transmural MI is expected to leave a residual wall motion defect. But many times it do not. Many non q inferior MI (Is there such an entity ?) do look perfectly normal by echo .
The primary reason for this is , infero-posterior surface is anatomically remote and it makes wall motion analysis difficult .Newer tissue motion analysis (Velocity vector imaging) could aid us better.
Some times a trivial or mild mitral regurgitation is the only sign of old inferior MI as the pap muscle lags behind in it’s functional recovery while free posterior wall is fully salvaged and contracting well .
Final message
It needs that extra bit of of knowledge to expose our ignorance.
Even in this maddening scientific era we have valid reasons to go back to fundamentals of R wave and Q wave genesis in MI , where clarity is lacking .