November 6, 2008 by dr s venkatesan
During CABG arterial grafts are always preferred over venous grafts , for the simple reason the grafted vessel has to carry arterial blood and not the venous blood. Saphenous veins are tuned to carry venous blood at low pressure.The mean coronary arterial pressure is around 40mmhg and this will damage the saphenous venous endothelium more quickly. The reocculsion rate at 10 years for venous grafts can reach 60%.

Left internal mammary artery (LIMA) is the most commonly used arterial graft. This is usually anastamosed with LAD. The lumen of LAD & LIMA are more or less equal and they match well in character also !
The other advantage of LIMA graft is , blood tends to flow both during systole and diastole in a smooth fashion.. Since the venous graft which hangs from the root of aorta , the ostium of venous graft lacks the hemodynamic benefits of coronary sinus . (We know the coroanry sinus acts like a reservoir for the smooth release of blood flow into coronary arteries.)
Finally , the most important feature of LIMA is
It is a live graft
LIMA’s proximal origin from subclavian is left intact, so LIMA acts as a live vessel with it’s vasa vasorum intact , which means the endothlium derived relaxing factor (EDRF-Nitric oxide) secretion is not interrupted.This makes the LIMA an excellent graft , self protected against reocclusion.One may call it a drug eluting graft !
What is the patency rate for LIMA ?
LIMA patency rates at 10 years is nearly 90 % .But the graft patency depends on many factors , like diabetes, age, gender, surgical technique ,(Now , beating heart CABG is very popular , where the LIMA patency is said to be slightly lower than conventional CABG) Sequential LIMA grafts, free LIMA graft ( Which loses the advantage of being a live graft) have relatively lower patency rates.
What are the other arteries used in CABG ?
Other arteries that could be used are radial artery, right internal mammary artery, and gastro epiploic artery.The patency rates of all these arteries far less than LIMA .

A surgeon testing LIMA flow before Anastomosing it to LAD.

Image courtesy Dr.Mannoj Aggny .You tube
Posted in cardiac surgery, Infrequently asked questions in cardiology (iFAQs) | Tagged annals of cardio thoracic surgery, beating heart surgery, bmj, bye pass surgery, bypass surgery, cabg, cardaic surgery, cass study, ctsnet, ctsnet.org, edrf, endothelium derived relaxing factor, gastro epiploic artery, graft, jama, lancet, lima, live graft, nejm, nitnitric oxide, opcam, radial artery, saphenous venous graft, triple vessel disaese | Leave a Comment »
November 5, 2008 by dr s venkatesan
Coronary artery by pass graft surgery has become the most common cardiac surgery done world over ever since it was first introduced by Favalaro in 1969.The common indications are, triple vessel disease and left main disease in any of the following situationsE.
Elective CABG(Non emergent)
1.Chronic stable angina
Either emergent or elective
1.Unstable angina
Emergency CABG*
1.Acute myocardial infarction.-Cardiogenic shock
2.Failed thrombolysis
3.Failed primary PCI
4.Complications during routine PCI(Cath lab crashes ! etc)
5.As an associate procedure after a mechanical complication during MI (Septal rupture, Acute MR etc)
*In emergency situations even a single vessel disease would require a CABG
Hybrid CABG
Combining CABG and PCI in the same patient is followed in very few centres .(Example LAD graft and RCA angioplasty)This is done in patients who have co morbid conditions who can not tolerate prolonged surgical times.Further there can be situations one lesion is very ideal for PCI while for other grafting is the only solution.
Controversial CABG
1.CABG as a primary revascularisation in STEMI*
(Rarely done now , almost obsolete , primary PCI has almost replaced it . . . but it is still useful if performed within 6 hours of MI )
2.Incidentally detected CAD* following routine coronary angiogram.
( *CABG for incidentally detected asymptomatic CAD is increasing in many parts of world )
Inappropriate CABG
If it’s triple vessel disese it must be CABG -CASS study (1980s)
Coronary artery surgery study (CASS) still has considerable influence among the cardiology community in the decision making process for CABG , even though it is many decades old .There has been a phenomenal development in both medical as well as interventional techniques since CASS . (Thrombolysis, Statins, ACEI, PCI DES to name a few) .
When CASS study was done many decades ago,it was believed triple vessel disese constitute a homogeneous population and carry the same clinical significance . For example a 90% proximal LAD , 50% RCA and 50% OM technically qualify for a CABG and unfortunately , some of them are subjected to it even in 2008 ! Now we clearly know, it is not the number of diseased vessels that is important, but it’s location, severity , LV function, presence or absence of diabetes . Finally , the presence of revascularisation eligible myocardium must be documented in all post MI patients . (Technically referred to viable & ischemic myocardium ).
Currently , with the PCI & medical management has grown so much, CABG should be reserved only for, critical triple vessel disese , with at least one proximally located lesion (Mostly LAD or Left main ), especially in diabetic individuals.
Posted in cardiac surgery, cardiology -Therapeutics | Tagged annals of cardio thoracic surgery, bari, bmj, by pass, cabg, cass study, chronic stable angina, drsvenkatesan, drug eluting stent, favlaro, graft, jama, lancet, lima, nejm, nstemi, pci, revascularisation, stemi, stent, viable myocardium | Leave a Comment »
November 5, 2008 by dr s venkatesan
This is a hemodynamic concept paper by Libanoff in 1968 published in circulation.This paper elegantly proved that the rate of fall of pressure across the mitral valve will predict the mitral valve orifice. This key paper formed the foundation on which Liv hatle developed the echocardiographic pressure half time .This pressure half time derived mitral orifice area ( 220/PHT) is key parameter world over for assessing severity of mitral stenosis non invasively .
Click on the link get this article .This article is available free fulltext from circualtion web site

Posted in Uncategorized | Tagged libanoff, liv hatle, mitral stenosis, mitral valve, pressure half time | Leave a Comment »
November 3, 2008 by dr s venkatesan
Is it true , once a patient is labelled as a hypertensive he remains hypertensive life long ? Is it possible to withdraw antihypertensive drugs permanently ?
- Systemic hypertension is the most common clinical entity and it forms the bulk of the physician consultations world over.
- The anti hypertensive drugs are one of the most commonly prescribed medication by the medical professionals .
- It is estimated , the major chunk of revenue to pharma industry is contributed by antihypertensive drugs.
- SHT , is being maintained as a major , global cardiovascular risk factor , by periodically refixing the target blood pressure to lower levels by various committees.
- The terminology of pre hypertension for blood pressure between 120-140 was hugely controversial and some societies refused to accept this entity.
Is there a case for withdrawal of anti hypertensive agents among our patients ?
Yes , in fact there is a strong case for it.
While on the one hand there is a sustained effort ( By whom !) to increase the drug usage , very early in the course of hypertension , there is also a silent progress in our knowledge , regarding withdrawl of anti hypertensive agents in all those undeserving patients .
It is estimated 42% *of the so called hypertensives especially elderly can be successfully weaned of anti hypertensive drugs with out any adverse effect.( Mark R Nelson BMJ. 2002 October 12; 325(7368): 815.)
What are the situations where we can successfully with draw anti hypertensive drugs?
- The most common group of patients are the ones, where the anti hypertensive drugs are started prematurely , with out giving an option for non drug life style approach.These patients and their physicians continue to believe , anti HT drugs are sacred and essential !
- There is another major group of patients who have had a temporary elevation of BP due to a stressful environment.These patients get drugs permanently for a temporary problem . These patients need to be reassessed.
- Some of the elderly patients, with the onset of age related autonomic dysfunction ,these drugs are poorly tolerated and even have disastrous effects .In this population it is desirable , to wean off the anti HT drugs and switched over to life style medication whenever possible.
Final message
Essential or primary hypertension is not a permanent disease, in bulk of our population. It reflects the state of the blood pressure on a day to day basis and is a continuous variable. All patients who have been labelled as hypertensives( Either by us or others) should be constantly reviewed and considered for withdrawal of the drugs if possible.
* Note this rule does not apply in all secondary hypertensions, during emergencies, uncontrolled hyper tension with co existing CAD /diabetes /dyslipidemias etc .
Please refer to these forgotten Landmark articles
Does Withdrawl of Anti hypertensive Medication
Increase the Risk of Cardiovascular Events?
The TONE study

Source: The American Journal of Cardiology, Volume 82, Number 12, 15 December 1998 , pp. 1501-1508(8)
http://www.ncbi.nlm.nih.gov/pubmed/9874055
Conclusion of TONE study
The study shows that antihypertensive medication can be safely withdrawn in older persons without clinical evidence of cardiovascular disease who do not have diastolic pressure > or = 150/90 mm Hg at withdrawal, providing that good BP control can be maintained with nonpharmacologic therapy
Some of the references for successful withdrawl of antihypertenive drugs
1.Nelson, M; Reid, C; Krum, H; McNeil, J. A systematic review of predictors of maintenance of normotension after withdrawal of antihypertensive drugs.
Am J Hypertens. 2001;
14:98–105.
[PubMed]
2.
Wing, LMH; Reid, CM; Ryan, P; Beilin, LJ; Brown, MA; Jennings, GLR, et al. Second Australian nationalbloodpressure study (ANBP2): Australian comparative outcome trial of ACE inhibitor- and diuretic-based treatment of hypertension in the elderly. Clin Exp Pharmacol Physiol. 1997;19:779–791.
3.
Lee, J. Odds ratio or relative risk for cross-sectional data.
Int J Epidemiol. 1994;
723:201–203.
[PubMed]
4.
Lin, D; Wei, L. The robust inference for the Cox proportional hazards model. J Am Stat Assoc. 1989;84:1074–1079.
5.
Veterans Administration Cooperative Study Group on Antihypertensive Drugs. Return of elevated blood pressure after withdrawal of antihypertensive drugs.
Circulation. 1975;
51:1107–1113.
[PubMed]
6.
Medical Research Council Working Party on the Management of Hypertension. Course of blood pressure in mild hypertensives after withdrawal of long term antihypertensive treatment.
BMJ. 1986;
293:988–992.
[PubMed]
7.
Alderman, MH; Davis, TK; Gerber, LM; Robb, M. Antihypertensive drug therapy withdrawalin a general population.
Arch Intern Med. 1986;
146:1309–1311.
[PubMed]
8.
Blaufox, MD; Langford, HG; Oberman, A; Hawkins, CM; Wassertheil-Smoller, S; Cutter, GR. Effect of dietary change on the return of hypertension after withdrawal of prolonged antihypertensive therapy (DISH). J Hypertension. 1984;2(suppl 3):179–181.
9.
Mitchell, A; Haynes, RB; Adsett, CA; Bellissimo, A; Wilczynski, N. The likelihood of remaining normotensive following antihypertensive drug withdrawal.
J Gen Intern Med. 1989;
4:221–225.
[PubMed]
10.
Myers, MG; Reeves, RA; Oh, PI; Joyner, CD. Overtreatment of hypertension in the community?
Am J Hypertens. 1996;
9:419–425.
[PubMed]
11.
Stamler, R; Stamler, J; Grimm, R; Gosch, F; Dyer, R; Berman, R, et al. Trial of control of hypertension by nutritional means: three year results. J Hypertens. 1984;2(suppl 3):167–170.
12.
Takata, Y; Yoshizumi, T; Ito, Y; Ueno, M; Tsukashima, A; Iwase, M, et al. Comparison of withdrawing antihypertensivetherapy between diuretics and angiotensinconverting enzyme inhibitors in essential hypertensives.
Am Heart J. 1992;
124:1574–1580.
[PubMed]
13.
Whelton, PK; Appel, LJ; Espeland, MA; Applegate, WB; Ettinger, WH; Kostis, JB, et al. Sodium reduction and weight loss in the treatment of hypertension in older persons: a randomised controlled trial of nonpharmacological interventions in the elderly (TONE).
JAMA. 1998;
279:839–846.
[PubMed]
14.
Heart Outcomes Prevention Evaluation Study Investigators. Effects of an angiotensin-converting-enzyme inhibitor, ramipril, on death from cardiovascular causes, myocardial infarction, and stroke in high-risk patients.
N Engl J Med. 2000;
342:145–153.
[PubMed]
15.
Howes, L; Krum, H. Withdrawing antihypertensive treatment. Curr Therapeutics. 1988;November:15–20.
16.
Fotherby, MD; Harper, GD; Potter, JF. General practitioners’ management of hypertension in elderly patients.
BMJ. 1992;
305:750–752.
[PubMed]
17.
Jennings, GL; Reid, CM; Sudhir, K; Laufer, E; Korner, PI. Factors influencing the success of withdrawal of antihypertensive drug therapy.
Blood Press Suppl. 1995;
2:99–107.
[PubMed]
Posted in Cardiology - Clinical, Cardiology-Land mark studies, Infrequently asked questions in cardiology (iFAQs) | Tagged allhat, amlogard, ascot, cardiology, hyper tension, jacc, jama, journal of hypertension, lancet, lancet. nejm, nejm, pharma insustry, shep, systemic hypertension, tomh, tone study | Leave a Comment »
November 2, 2008 by dr s venkatesan
Which is the most important factor that determines thrombolysis failure in STEMI ?
- Thrombus load .
- Drug efficiency
- Time delay
- Presence of a mechanical lesion
- Hemodynamic instability
Answer : 3 .(Though all 5 factors operate )
Failed thrmbolysis occur in about 40-50% after streptokinase and slightly less with TPA and TNK-TPA . Delayed arrival and late thrombolysis are most common cause of failed thrombolysis. As the time flies , the myocardium gets damaged and the intra coronary thrombus gets organised .Both these processes make delayed thrombolysis a futile exercise.
Not all STEMI patients have large thrombus burden. There need to be a critical load of thrombus for thrombolytic to be effective
Some may have a major mechanical lesion in the form of plaque fissure, prolapse and it simply blocks the coronary artery mechanically like a boulder on the road . The poor streptokinse or the rich Tenekteplace ! nothing can move this boulder .The only option here is emergency PCI .
How will you know when the patient arrives in ER with STEMI whether his/ her coronary artery is blocked with soft thrombus or hard mechanical boulder ?
It is impossible to know.That’s why primary PCI has a huge advantage. But still thrombolysis is useful as some amount of thrombus will be there in all patients with STEMI.Lysing this will provide at least a trickle of blood flow that will jeep the myocardium viable and enable us to take for early PCI.
Final message
The commonest cause for thrombolytic failure is the time of administration and the degree of underlying mechanical lesion . So it does not make sense to blame streptokinase always !
Posted in Cardiology -Interventional -PCI, cardiology- coronary care, Infrequently asked questions in cardiology (iFAQs) | Tagged bmj, cardiology, coronary, drsvenkatesan, failed thrombolysis, jacc, lancet, nejm, nstemi, stemi, streptokinase, tenekteplace, thrombolysis, tpa | Leave a Comment »
November 2, 2008 by dr s venkatesan
Hypertension is considered a major cardiovascular risk factor.Hypertension can have multiple physiological and pathological effects on heart . The common response to raised arterial pressure is the hypertrophy of the left ventricle ( LVH). This can increase the risk of heart failure in few ( Mainly diastolic failure) It is a leading cause for stroke and less often a coronary event.
What links Hypertension and coronary artery disease

Coronary artery disease is almost synonymous with atherosclerosis. There is no separate entity called hypertensive coronary artery disease. But HT can accelerate the process of atherosclerosis. It is widely understood, hypertension can cause physical endothelial damage and functional impairment of endothelial function.The physical damage ie enothelial disruption , or erosion is a very uncommon phenomenon . So currently there is sufficient clinical experience HT is considered dangerous for coronary artery only if it is with the company of diabetes and hyperlipidemia. (This will seem controversial as it is against the findings of iconic Framingham trial!)
What the medical community refers to hypertension , may not be really so inside for the coronary arteries.
The relationship between brachial cuff blood pressure and the intra coronary pressure has very little linear relationship. So one should recognise it is the intra coronary hypertension that has a immediate impact on the coronary events. Now only , we are beginning to understand the complexities of the relationship between HT and CAD. If we analyse a series of individuals HT per se is not a very serious risk factor for CAD* , but it is a number one risk factor for stroke.
Why HT in isolation often result in stroke , rather than a MI ?
While HT is notoriously common to result intracerebral hemorrhage, the same HT would not cause intramyocardial bleeds . Why ?
What is protecting the myocardium against this complication ?
The exact mechanism is not clear.Acute surges of blood pressure can increase the risk of stroke many times but rarely precipitate a coronary event( But may cause a LVF) . The reasons could be the coronary endothelial shearing stress is less than the cerebral blood vessels.Both cerebral and coronary circulation has auto regulatory mechanism . The coronary auto regulation is more robust in that it does not allow intra coronary pressures to reach critical levels .There is no clinically relevant intra myocardial hemorrhage reported even during malignant hypertension.
*But a high intra coronary pressure can sometimes result in spontaneous coronary dissection and plaque fissure .Lipid mediated injury is vey much facilitated in a high pressure environment.
Has Controlling blood pressure to optimal levels , reduced the overall CAD morbidity and mortality ?
The answer is yes, ( But not an emphatic yes ! ) Some studies had been equivocal. It is very difficult to say , how much benefit is attributable to BP reduction per se and how much is attributable to indirect effect on atherosclerosis prevention.
Hypertension during ACS
High blood pressure during an episode of unstable angina or STEMI can increase the myocardial oxygen demand and worsen the ischemia. It requires optimal control with nitroglycerine ( Preferably ) or beta blocker and ACE inhibitors.Even though HT is commonly associated with ACS, one can not be sure the ACS is preciptated by HT. Many times the sympathetic surge during an ACS keeps the blood pressure high.It is a common experience the blood pressure suddenly dropping to normal or hypotensive levels once the pain and anxiety is controlled.
Hypertension during thrombolysis
High blood pressure is a relative contraindication for thrombolysis.It need to be emphasised here, It is the the fear of stroke that make it contraindicated .The heart can tolerate thrombolytic agents delivered at high BP .In fact logically , hemodynamically and also practically it is obseved , thrombolytic agents administered at relatively high blood pressure (140-160 systolic) has better thrombolysis than a patient who is lysed at 100mmhg.
The coronary pressure head which contain the thrombolytic agent (streptokinase and others ) need to have pressure jet effect on the thrombus.So the mean coronary perfusion pressure becomes a critical determinant of success of thrombolysis.
It is a paradox of sorts , very high blood pressures are a relative contraindication for thrombolysis and at the same time normal pressure patients fare less well to thrombolysis.
Final message
Hypertension continues to be a major cardiovascular risk factor.It has direct and indirect effects on the heart.Generally HT is more of a risk factor for stroke than CAD.A slightly high BP ( Just around the upper limits of normal or just above it ) has a hemodynamic advantage during thrombolysis.(Class C evidence )
Posted in Cardiology -Interventional -PCI, cardiology -Therapeutics, cardiology- coronary care, Infrequently asked questions in cardiology (iFAQs) | Tagged acs, auto regulation, bmj, coronary angiogram, coronary risk factor, failed thrombolysis, hypertension, intra cerbral hemmorhage, intra coronary hypertension, intra coronary pressure, jacc, lancet, left ventricualr hypertrophy, myocardium, nejm, nstemi, stemi, streptokinase, stroke, systemic hypertension. cva, thrombolysis | Leave a Comment »
October 31, 2008 by dr s venkatesan
Why is criticism of newer scientific technologies always frowned upon or rather considered indecent ?
In science you don’t require politeness , we only require correctness.This is especially true in medical sciences. But this is easier said than practiced in the scientific community . In any scientific conferences the only a couple of minutes or few lines are allotted for the customary negative issues and the limitations of the study.
Unscrutinised science can no longer be called as science ! it can only be termed as pseudo science!
It is believed skepticism is a powerful dampener for the scientific growth.May be it was true in the earlier era of pre industrial world. But those days science was growing only with passion for discovery and an un contaminated mind.But now too many conflicts have cropped in.
What is positive thinking ? and What is negative thinking in science ?
To be continued . . .
Posted in Uncategorized | Leave a Comment »
October 31, 2008 by dr s venkatesan
What is herd behavior ?
It is a behavioral pattern where in animals and humans in large numbers , tend to behave in the same way at the same time without application of mind .
Herd behavior in human societies
Herd behaviour describes how individuals in a group can act together without planned direction. The term pertains to the behaviour of animals in herds, flocks, and schools, and to human conduct during activities such as stock market bubbles and crashes, street demonstrations, sporting events, episodes of mob violence and even everyday decision making, judgement and opinion forming. This is very much applicable to medical profession also.(Ref:Wikipedia)
Herd behaviour in animals and human how they are different ?
“surprise ! surprise ! There is very little difference noted , according to Hamilton”
A group of animals fleeing a predator shows the nature of herd behavior. In the often cited article “Geometry For The Selfish Herd,” evolutionary biologist W. D. Hamilton said each individual group member reduces the danger to itself by moving as close as possible to the center of the fleeing group. Thus the herd appears to act as a unit in moving together, but its function emerges from the uncoordinated behavior of self-seeking individuals.
Among humans for example when panicked individuals confined to a room with two equal and equidistant exits, a majority will favor one exit while the minority will favor the other.
Medical professionals as a herd

The practicing habits of medical professionals move , symmetrically as a herd . When a top journal or a opinion leader utters something every one tend to move in that direction .
If a herd leader says a particular treatment is great, every one will say yes . If he says nay every one will say nay !
No one will really question the direction they move ? Unless the correction occurs from within the herd. No external forces usually are effective.Herding is also benefitial many times as rapid propogation of scientific facts needs such behavior ,but it needs constant scrutiny.
Herd behavior example 1 : The most typical example is the drug prescribing pattern of anti hypertensive agents over the past half century.The movement from diuretics to beta blocker , from beta blockers to calcium blockers and to ACE inhibitor and again to diuretic , then to ARBs and currently shying strongly away from beta blockers, in between have a brief encounter with alpha blockers and finally back to diuretics.
If a particular physician by his insight , had clinged onto diuretics ( Away from the herd ) for over three decades he is a real exemption , although branded old timed and unscientific , he has been the most scientific medical professional indeed !
Herd mentality example 2 : Every one says so ! so it must be true ! Hormone replacement therapy good or bad goes with the leader of the herd .
Herd mentality example 3: Very few cardiologists will be ready to agree the fact that , simple digoxin and diuretic ,ACEI, beta blocker, administration could be as effective as the costly cardiac resynchronisation therapy in atleast some of patients with wide QRS cardiac failure ( As we know up to 30 % wide QRS CHF population do not respond to CRT)
Defying Herd mentality resulted in major break throughs in medicine
When every one was saying beta blocker was harmful in CHF one person from Briton defied it ( Wagenstein, and now beta blockers are the mainstay in the management of CHF! )
There are hundreds of treatment modalities popularised by such herd behavior
Who is the watch dog , whether science is moving in the correct direction ?
Read this land mark article how medical research can be distorted by such learned behavior and how scientific research should not be done .
Click on the image .

This post is not intended to hurt anyone . It reflects , human beings are not fully evolved yet , in the onging process of evolutionary biology.
Posted in cardiology-ethics | Tagged annals of internal medicine, bmj, cardiology, drsvenkatesan, ethics in medicine, herd behavior, lancet, medicine, nejm | Leave a Comment »
October 27, 2008 by dr s venkatesan
CRT , cardiac resynchronisation therapy is being projected as a revolutionary treatment for cardiac failure , where a failing heart is rewired electrically through multiple leads and make it contract more effectively.The success rate of CRT was highly variable.The basic question here is, there should be a significant documentation of desynchronisation prior to CRT , for resynchronisation to be effective. Further , the sites of myocardial stimulation ( Coronary sinus/LV epicardial) , dose of electricity and the sequence of stimulation and the electrical delay are very critical. Achieving this into perfection is not a simple job and is real rocket science ! ( If we can achieve 5 % of what the normal purkinje network do within the LV we can term it a huge success.) Let us hope we catch up with nature . Finally , it is ironical the sites of LV pacing , electrophysiologists select currently is infact not selected by them but pre selected by the patients coronary venous anatomy ! .So as on date , one can imagine how scientific this treatment could be !
Initially it was adviced for patients with only wide qrs later for even normal qrs patients.When people started using it indiscriminately insurance companies started to rethink and thus came the RETHINQ study in NEJM and brought a full stop to CRT in normal qrs CHF.
How to identify who will benefit from the costly CRT ?
It is a million dollar question. So millions of dollars were spent to identify the correct tool to identify the true responders to CRT.Echo cardiography with sophisticated methods tissue doppler, tissue tracking and , 3 D echo ,velocity vector imaging were done .These methods are not only costly but also time consuming and hugely expertise driven.
Does all this efforts with advanced echo techniques worthwhile ?
This simple question was addressed in PROSPECT study in circulation
Click to read the article
Posted in Cardiology - Electrophysiology -Pacemaker, Cardiology -Interventional -PCI, cardiology -Therapeutics | Tagged bmj, cardiac failure, cardiac resynchronisation therapy, care hf, circulation, combo device, CORONARY SINUS, coronary veins, cpmanion, CRT, desynchronisation, echocardiography, electrophysiology, ICD, jama, lancet, lv epicardial pacing, madras medical college, medtronic, miracle, nejm, prospect, resynchronisation, rethinq, st jude, tissue tracking | Leave a Comment »
October 20, 2008 by dr s venkatesan
The superior aspect of coronary sinus and a portion of the left atrium share a common wall .Embryological defects in this area result in a communication between left atrium and coronary sinus. This defect descriptively called as unroofed coronary sinus .This entity is most commonly associated with persistent left SVC. Extreme form of unroofing is some times termed as absent coronary sinus.

How to diagnose it ?
A high degree of anticipation is necessary in all patients with ASD or LSVC. A dilated coronary sinus in routine echocardiography warrants full investigation. A contrast echocardiography with agitated saline injection in left cubital vein will clinch the diagnosis as contrast enters LA after opacifying the dilated coronary sinus. During right heart catheterisation catheter course entering coronary sinus and advancing into LA through the fenestrations (Unroofing) will confirm the defect.
How do you classify unroofed coronary sinus ?
The morphologic type of URCS was classified as Kirklin and Barratt-Boyes
Type I, completely unroofed with LSVC;
Type II, completely unroofed without LSVC;
Type III, partially unroofed midportion;
Type IV, partially unroofed terminal portion
What is the clinical relevance of this entity ?
This entity should be suspected in every patient with persistent LSVC, ( and LSVC should be suspected in every patient with ASD). The hemodynamics is that of an ASD but if sufficient mixing of LSVC blood and LA blood takes place the child will have mild cyanosis.Some times when the coronary sinus is totally absent it will present as a typical dusky ASD picture which can closely mimic a TAPVC clinically.
Surgeons have a greater role in recognising and treating this entity. A typical repair will be done like this
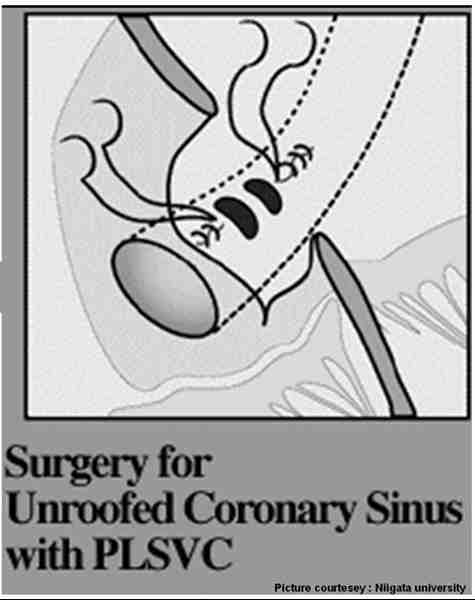
Links to some of interesting articles on this topic
Raghib circulation 1965
Posted in cardiology -congenital heart disease, cardiology congenital heart disese | Tagged ATRIAL SEPTAL DEFECT, cardiology, congenital heart disese, contrast echocardiography, CORONARY SINUS, coronary sinus asd, cyanosis in asd, dilated coronary sinus, drsvenklatesan, madras medical college, PERSISTENT LEFT SVC, ucla, unroofed coronary sinus | 1 Comment »
« Newer Posts - Older Posts »












