December 14, 2008 by dr s venkatesan
One of the important principles of post PCI care is, we need to be very careful till the metal struts are fully endothelialised . This is of vital importance as improper endothelialisation is a powerful trigger and nidus for a imminent thrombosis and acute coronary syndrome.

It is a billion dollor irony , the much hyped DES does exactly what we don’t want ! and still it’s usage is increasing world wide . The drugs (Anti cancer agents) which coat the DES are the villains as it prevents the metal struts from being endothelialised and keep the metal surface raw and vulnerable , while the much maligned bare metal stents allow this natural endothelialisation process without any interruption ! So right now it is mandatory to administer dual antiplatelet agents life long( life of the stent !) for the patients with DES.
Just look , at the following image of a stent in vitro at 30 days follow up


Posted in Cardiology -Interventional -PCI, cardiology -Therapeutics, Infrequently asked questions in cardiology (iFAQs) | Tagged acc.aha, bare metal stents, cypher, drug eluting stents, endothelium, europcr online, paclitaxel, ptca, scai, sirolimus, tct md, xience v | 1 Comment »
December 14, 2008 by dr s venkatesan
Let us not forget the basics !
- HT management has been made easier with the availability of many good drugs , at the same time it has become a complex issue with as many classification and guidelines.
- The management of HT has evolved over the decades. Now we have realised HT is not a simple number game . Reducing the blood pressure to target levels is not sufficient and is not the primary aim !.
- In fact we now know controlling the numbers alone is never going to work , combined risk factor reduction is of paramount importance.
- HT per se is less lethal but when it combines with hyperlipidemia and diabetes or smoking it becomes aggressive.The blood lipids especially the LDL molecule enjoy the high pressure environment , penetrate and invade the vascular endothelium.
- ASCOT LLA study has taught us, for blood pressure reduction to be effective and reduce CAD events one has to reduce thier lipid levels also.So , for every patient with HT there is not only a target BP but also a target LDL level .

Final message
The tip for better vascular health is , all hypertensive patients should keep their lipids to optimal levels and all hyperlipidemia patients should keep their BP as low as possible .
“Keep your LDL as low as your diastolic blood pressure and let us keep it around 70 -80
Posted in cardiology -Therapeutics, Cardiology hypertension | Tagged allhat, ascot, atherosclerosis, bmj, coronary artery disese, diastolic blood presssure, hyperlipidemia, hypertension, jacc, jama, lancet, ldl, lipids, mayo clinc, nejm | Leave a Comment »
December 12, 2008 by dr s venkatesan
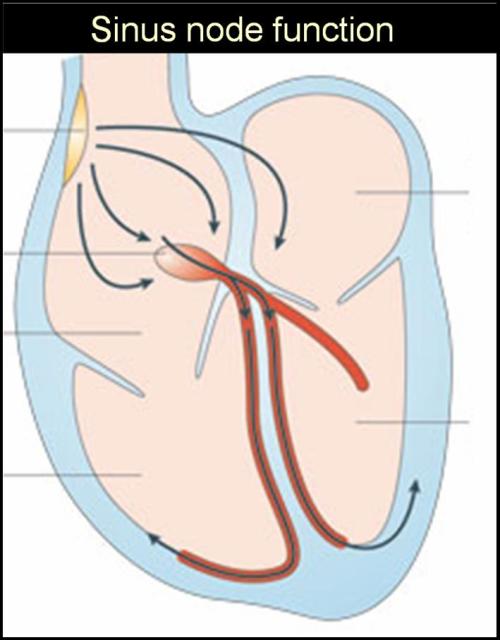
Sinus node as the pacemaker , orchestrates the rhythm of life . It has to fire for the entire life time of a person.It can not afford to take any rest ! But it can pause a little bit , of course that pause could be less than 15% of it’s basic sinus length. This variation of sinus cycle length is called sinus arrhythmia.This is physiological. When it exceeds 15 % of the previous sinus cycle it is referred to as sinus pause.
Have a look at this ECG

What follows a long pause ?
By strict terms of definition a sinus pause should be followed by a delayed , next sinus beat only. A sinus pause , many times is followed by JPD – Junctional escape beat.This situation should be ideally referred to sinus arrest as the sinus node is taking too much of rest and it is not able to wake up from the slumber and it needs assistance form the junctional pace maker.
So even though sinus pause and sinus arrest is used many times interchangeably, it should be avoided.
What are the electrophysiological mechanisms of sinus pause ?
- Simple sinus bradycardia . The commonest mechanism is the increased vagal tone. This occurs more often in young athletes. Eventhough increased vagal tone conveys a innocuous meaning , at times this can also be symptomatic and require intervention.
- Sinus node exit block.
- First degree, second degree, complete SA block can occur as in AV node.
First degree SA block can not be diagnosed by surface ECG. Third degree SA block is same as sinus arrest and subsidiary pacemaker will function in these patients. Second degree SA block is usually diagnosed when the sinus pause is in the multiples of resting sinus cycles. If the pauses are not in exact multiples sinus arrest is diagnosed. All these arrhythmia’s are collectively called sinus node dysfunction(SND)
How do you manage these patients?
Sinus node disorders can occur in number of systemic diseases*. It needs to be ruled out.
- Infiltrating diseases like amyloidosis, hypothyroid states can result in SND.
- Drug induced SND like beta blocker and calcium blockers are fairly common and should be excluded
- Some congenital heart disease (SVC ASD) can involve sinus node.
- Ischemic SA node disease is rare but can occur following infero posterior myocardial infarction
- Sinus node disorders are very often related to degenerative atrial diseases associated with HT, cardiomyopathy etc
*The list is not exhaustive
A very important association is noted with atrial fibrillation as a part of tachy brady syndrome .The link between SND and AF is obvious as atrial pathology is the common denominator in both ! This will be discussed later.
When is a pause significant ?
Any pause that is producing significant symptoms is significant.This depends upon the overall hemodynamic compensation of the patient.Young, and fit can even tolerate three second pause without symptoms.Underlying heart disease makes even a smaller pause symptomatic.But generally a 3 second or more pause is almost always pathological .Pauses can be up to 5 seconds ( a 5 second pause actually means a heart rate of 12/mt , obviously it can not go on for a minute, a patient will develop a syncope). A 3 second pause corresponds to 20/minute.
How will you evaluate a patient with sinus pause ?
There are sophisticated electrophysiological studies (EP) available like sinus node ECG ,sinus node function studies like sinus node recovery time, activation time etc. But these are generally of academic interest.
If a patient is symptomatic (syncope) because of bradycardia he requires a pacemaker and EP study is redundant . Similarly , if he is totally asymptomatic in spite of pauses , again EP study is not indicated.
Only for patients in the grey zone, further studies are indicated .This would include a extended holter, loop recorders, event monitors etc.
Another important issue to consider is , before putting a pacemaker patient”s symptom must be correlated with their arrhythmia.
What is the overlap between sinus node dysfunction and neuro cardiogenic syncope ?
SND can occur as an overlapping syndrome with neurocardiogenic syncope.(NCS ).NCS is also a very common cause of syncope .In NCS there are two limbs .Cardio inhibitory and vasodepressive. The cardio inhibitory form can exactly mimic an SND. In a given patient it is very difficult to pinpoint which of this limb is dominant.Head up tilt test(HUT) might help in few. If a patent’s symptoms are due to inappropriate vasodilatation pace maker may not reduce the symptom of dizziness or syncope.
Management
- There is no ideal medical therapy* available as on date
- Withholding all drugs which might aggravate bradycardia is of paramount importance.
- Pace maker is the specific treatment in all symptomatic patients.
*Aminophyline tablet may be useful in some patients .It acts by antagonising adnosine receptors in SA node.Other drugs which can incrase the heart rate in the short term include Orcipranaline(Beta 2 stimulant /Alupent ) Probantheline(M 1 blocker)
The key issue is to avoid unnecessary pacemaker implants in patients who have insignificant pause.
Which pacemaker is ideal in SND ?
The need for dual or single chamber pacemker will be taken by the electrophysiologist .Atrial based pacemaker (AAI) is preferred as it gives physiological pacing .But a simple ventricle based VVI pace maker is good enough in vast majority of patients. This takes care of future risk of AV block also. DDD pace maker is the most physiological pacemaker and it is supposed to provide better quality of life. But it has an issue of insertion and maintenance of two leads, multi parameters to be programmed.It should switch to appropriate modes at different times.(Like VVI mode during atrial fibrillation etc).Trouble shooting needs expertise , while VVI is simple, safe , and just effective as well .(In this turbulent world, quality of life is a too trivial an issue to be determined by a DDD maker)
Posted in Cardiology - Electrophysiology -Pacemaker, cardiology -ECG, Cardiology-Arrhythmias, Cardiology-Coronary artery disese | Tagged alupent, aminophyline, bradycardia, ddd pacemaker, drsvenkatesan, dual chamber pace maker, electrophysiology, neuro cardiogenic syncope, orciprenaline, pace maker, sa block, sick sinus syndrome, sino atrial block, sinus bradycardia, sinus node dysfunction, sinus pause. sinus arrest, syncope, theopace study, vvi pace maker | 4 Comments »
December 10, 2008 by dr s venkatesan
It is now mandatory for all journals to declare the conflict of interest by the authors who are involved in medical research .The purpose apparently is to make all transactions or links between the researchers and their funding agencies transparent .Even major journals do not go beyond this . Some ensure it , to appear in the first page of the article.
What does the the journals tend to convey to the reader by publishing the conflicts of interest ?
- Does it mean the article in question may have a bias or indeed have a bias ? and readers are warned hereby !
- Do they send across a message that the article may not be really a genuine one and the judgement is left to the the consumers of the articles ?
How often a journal article is rejected purely on the basis of conflicts of interest ?
Most of journal articles are rejected for poor methodology, statistical analysis and so forth .We don’t know how often a paper is rejected due to a conflict issue per se.If this could happen ,bulk of drug trials would face a torrid time from the editors.
Why , even the leading scientific journals never indulge in grading the significance of the conflict ?
Here is an example .


The much hyped drug trial on Hypertension “ACCOMPLISH” was published in the world’s most prestigious medical journal recently .It left it to the readers to have their own assessment on the conflict issue.
The consequence of not , grading and investigating about the conflicts could have serious global health implications both financially and academically .
This study was designed, formulated, completed and published with a single hidden aim of neutralising the land mark trial of ALLHAT which recommended diuretics as a first line drug in HT.Apparently diuretics are very cheap , effective generic drugs.
Is it a scientific rule that the latest evidence , should always prevail over the older evidence ?
No. Science can never have such a rule ! The question is how good and genuine is the evidence.
Just because an evidence is current , it does not attain a scientific sanctity !
Posted in bio ethics, Cardiology - Clinical, cardiology -Therapeutics, cardiology-ethics, Cardiology-Land mark studies | Tagged accomplish, allhat, annals of internal medicine, bioethics, bmj, conflict of interest, diuretics, drsvenkatesan, drug trials, ethics, jama, jnc 7, lancet, nejm | Leave a Comment »
December 9, 2008 by dr s venkatesan
One of the important principles of medicine is “Diagnosis should always precede treatment”
This quote , though appear reasonable , can not be practiced always especially in emergencies, where we have to first stabilise the patient without a prior diagnosis .(Like administering IV fluids in hypotension , acetaminophen for fever , etc)
Modern medicine considers treating a patient without a diagnosis as unscientific.
But, it is a well recognised fact , millions of decision in everyday medical practice is not based on scientific diagnosis but on clinical acumen and empirical therapy . There are many instances wherein , we are never near the diagnosis even after exhaustive investigations.

Ironically , in this era of evidence based medicine , when we are unable to conclude , we are forced to do the most funniest thing , namely converting patient’s symptom itself as disease entity and be happy in labelling them. Like , Motion sickness , poly-arthritis, , chronic fatigue syndrome, adult respiratory distress syndrome , pre mature ejaculation, fever of unknown origin , attention deficit disorder , etc (The list is endless . . .)
This happens because physicians always feel guilty if they are unable to label a patient with a disease entity.
Is the guilt justified ? Not necessarily so ! Symptomatic treatment without diagnosis is the most dominant theme even today (Fever, pain etc ).So don’t feel unduly negative* when one is not able to fit a patent’s symptom into a disease entity but ensure he gets relief from his symptom.
*Except of course , one has to rule out a serious disorder.
Comments welcome
Posted in bio ethics, cardiology-ethics, general medicine | Tagged annals of internal medicine, bio ethics, cecil, conflicts, davidson, diagnosis, doctor, ethics, harrisons, health care, jama, lancet, medical errors, medical science, medical student, medicinehippocrates, mmodern medicine, nejm, principles of practice of medicine, pseudo science, who | Leave a Comment »
December 9, 2008 by dr s venkatesan
Hypertension is the most common clinical cardiovascular entity.Left ventricular hypertrophy (LVH) is an important consequence of HT.In fact, it is considered as a end organ effect or damage. Others being brain, kidney, and peripheral vascular disease.Knowing about LVH is important because it has been linked to increased cardiovascular events.
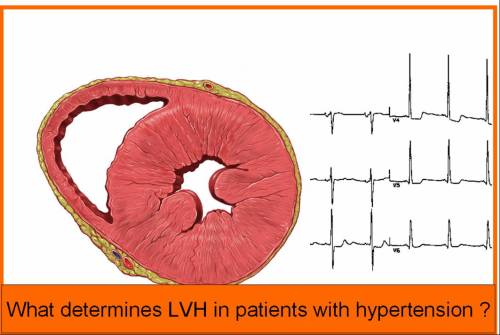
Though LVH is considered as a close companion of HT it is surprising only a minority (15-30%) show evidence of LVH .Some experienced clinicians (Level C evidence) quote even lower < 10 % .Traditionally LVH was detected by ECG and now it is replaced by echocardiography.
What determines the LVH ?
It will be suprising to note , answer to this question is still not clear .
- Is it the duration of elevated blood pressure ?
- Is it the absolute level of blood pressure ?
- If so , is it the systolic BP , diastolic BP or the mean BP ?
- Or is it related to the etiology of HT ?
- There has been no significant correlation between the above parameters
When we don’t know the answer to a question in medicine , the answer will generally will be inside the genes !
So in HT also the major determinant of LVH is in the genes that determine the myosin heavy chain response .
and also ACE gene polymorphism.ACE genes are involved in the expression of growth factors within the myocardium.
An excellent study on the issue http://www.nature.com/jhh/journal/v17/n3/full/1001523a.html#tbl1
It implicates , gender, age, race etc in the genesis of LVH
Final message
So , the myocardium does not respond with LVH in all patients with HT.It happens only in a minority* .Duration of HT can be an important determinant , but the major factor is the alteration of genetic switches within the myocytes How this switches are going to behave , is largely inherited .Regression of LVH is also not uniform again implying lesser role for hemodynamics. (Some studies revealed ACEI have maximum regression of LVH , later disputed )
*LVH is more consistently seen in hypertension due to reno vascular or parenchymal disorders .It is also an observed fact , a combination of diabetes and HT is more likely to result in LVH.
The other major issue that needs explanation in HT/LVH is , how much of LVH is due to myocyte hypertrophy perse and how much is contributed by interstitial cell hypertrophy(Non myocytic hypertrophy)
This issue will be discussed soon
Posted in cardiology -Therapeutics, Cardiology -unresolved questions, Infrequently asked questions in cardiology (iFAQs) | Tagged acc.aha, ace inhibitor, ameriican journal of hypertension, bmj, drsvenkatesan, hypertension, jama, kaplan, lancet, lvh, myocyte, myocytic hypertrophy, nejm, non myocytic hypertrophy, reanl hypertension, regression of lvh, sweeny, systemic hypertension | Leave a Comment »
December 9, 2008 by dr s venkatesan
This paper was presented in the just concluded 60th Annual scientific sessions of cardiological society of India , Chennai.India
POSITIVE ALLEN’S TEST FOLLOWING RADIAL CORONARY ANGIOGRAM
Venkatesan sangareddi , G.Gnanavelu, R.Alagesan,V.Jaganathan.
Department of cardiology, Madras Medical College, Chennai.
Radial artery has become the major access site for the interventional cardiologist in recent years. Radial approach has provided increased patient comfort and less access site complication. Many of the complications are unique to radial approach mostly due to anomalies of origin, and course while others are hardware related .Unlike femoral arterial access , compromise of blood supply to hand is never considered a threat because of dual blood supply to hand .But the fact is that, it could be sub-clinical and the hand is rarely assessed for vascular insufficiency after a radial procedure.
The aim of the study is to assess the impact of radial procedures on the blood flow to hand . 20 patients who had undergone routine radial coronary angiogram formed the study population. All patients had negative Allen’s test prior to the procedure. The mean procedure time was 25mts (18-45) .Standard hardwares were used. Difficulty in crossing at forearm and subclavian was observed in 4 patients. Extravasation of dye in forearm was observed in two. Allen test was done 24 hours after sheath removal and repeated 48 hours after the procedure . 4 patients showed positive Allen test at 24hrs. One patient regained Allen negativity at 48hours. The incidence of positive Allen test at 24 hours is 20%. The compromised blood flow was correlated with the procedure time, and a difficult catheter course .
We propose, radial procedures especially , when prolonged has a potential to compromise palmar arch flow .This phenomenon is either permanent or transient and may be attributable to enhanced endothelial tone and sheath related injury. Irreversible compromise of blood flow to palmar arch may also occur in radial dominant hands. Further enhanced sympathetic tone can spill over to ulnar artery as well .
It is concluded, interventions through radial route has hitherto unreported adverse effect of “Post procedural positive Allen test” . It implies , radial procedures could convert a dual blood supply pattern of the hand to ulnar dependent uni-modal blood flow in a significant subset of patients. This is important to recognise, as it precludes further radial procedures in the same patient.
Final message
Hand function could be as vital as our heart’s , please handle with care to avoid this complication
Click on the slide to download PPT presentation

Posted in Cardiology -Interventional -PCI, cardiology- coronary care | Tagged acs, allen test, arrow, cath lab, palamar arch, pci, radial coronary angiogram, radialforce.org, ulnar artery | 1 Comment »
November 30, 2008 by dr s venkatesan
The science of medicine has evolved over 2000 years since the stone age days.It has currently reached a glorious era with cutting edge scientifc technology .Today one can map the entire human genetic blue print and intervene in the disease even before they manifest .One can keep dying people alive for years with multi organ transplantation. Modern medicine has taught us how human sufferings can be prevented and life can be prolonged (with or without purpose !)
The term conservative management conveys two different
meanings for medical professionals.

For other group of physicians

Ever since the days of application of leech over the head for treating migraine and a crude knife abdominotomy for emergency exit of babies from pregnant mothers in distress , healer’s mind has always perceived “something has to be done urgently when some body suffers” this sort of reaction is probably inherited and is related to the primitive flight or fight response .
This may be true in some of the emergencies but it is untrue in many of the non emergencies.
Unfortunately , our mind finds it difficult to differentiate between these situations . With constant exposure to dramatic medical breakthroughs , modern day physician is made to believe “Some thing is always better than nothing when illness strikes. Human body is a wonderful machine which has it’s own service station ! in the form autoregulation and the meticulous homeostatic mechanisms. Only if the disease process overwhelms, it needs intervention.( Typical example:In the routine viral fever , you don’t adminster Acyclovir or other antiviral for all of them !)
The problem with early aggressive approach is, it fails to give an oppurtunity for the body’s natural defence forces to respond. Further , we will never ever know how the administered treatment is going to fare vis a viz the natural response.( With due respects to RCTs). While the field of medicine has so much evolved , our thought process, especially the aspect of clinical reasoning has always been lagging behind .It is now considered as inferior or even unscientific treatment if some one follows a conservative approach to a problem even if it provides same outcome of that of an invasive or aggressive approach ( The classical example is PCI for chronic stable angina The COURAGE study).
The other major issue is the hazards of unwarrnted invesitigations , drugs and procedures
Classical example:No one knows how much morbidity or mortality the routine Swan ganz catheter caused when it was rampantly used for over two decades to monitor central venous pressure .It is estimated that in modern medicine there are at least few drugs or devices in each speciality waiting for the same fate as that of the swan ganz catheter.
No body knows when it will be exposed .Our EBM will take it’s own time . . .Till that time humanity need to suffer.
This thinking is not new The concept “First do no harm is over 2000 years old”

Questions in search of answers
Does law of conservation of energy applicable to human body and medicine ?
Can we defy death with modern medicine ?
Final message
- Conservative management is still a great medical concept in many situations and one should not allow it to die by the whims and fancies of the modern scientific forces.
- Whatever you do on the patent’s body do it , only if it is going to helpful for him /her. If you are unsure Whether a given treatment is going to help or not ask this question to an expert .
- The widely prevailing dogma of aggression is always better than non aggression has absolutely no evidence.
- So approach a clinical issue disease by disease , individual by individual.
- Now , in this era high tech medicine , It is lot more tougher to choose a conservative path as the pressure to do more and more looms larger ! It is easier to follow the crowd than a path of your own .
- Always remember it needs a stronger mind to act according to our conscience !
Posted in Cardiology - Clinical, Cardiology -Interventional -PCI, cardiology -Therapeutics, cardiology- coronary care, Infrequently asked questions in cardiology (iFAQs) | Tagged annals of internal medicine, conservative management, davidson, ethics, first do no harm, harrisons, hippocrates, history of medicine, jama, lancet, medicine, nejm, primum non nocere | 3 Comments »
November 14, 2008 by dr s venkatesan
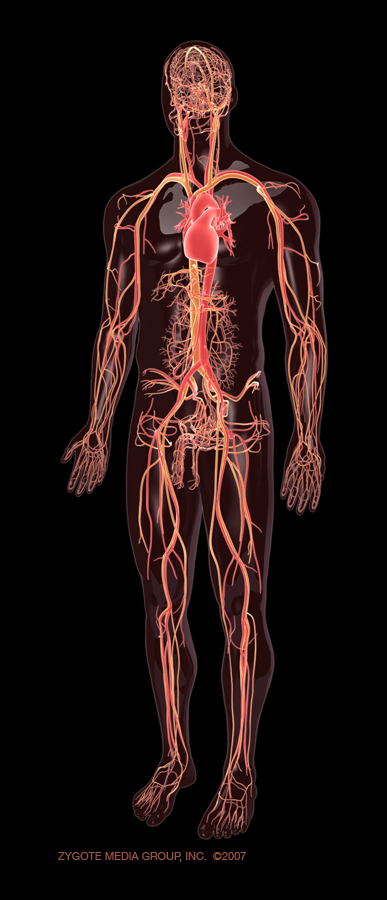 A normally functioning circulatory system is vital for our survival . We have about 6000 ml of blood, circulating all over the body in an approximate time of 15-20 seconds.The pressure at which this blood moves across the body is called the blood pressure . Hypertension or simply , high blood pressure is an undesirable hemodynamic disturbance in human circulatory system.Systemic hypertension is the most common type of hypertension. The blood pressure is primarily dependent on the status of the blood vessel(vascular resistance) and cardiac contractility. This regulation is under many neural and hormonal factors.Further the blood pressure varies depending upon the blood vessel calibre, and the local milieu.There is a progressive drop in blood pressure from major arteries to the small arteries .The pressure drop is maximum across the arterioles to reach the venules .The venous circulation has the lowest pressure, it ends up at right atrium with a mean pressure of 0- 5mmhg.
A normally functioning circulatory system is vital for our survival . We have about 6000 ml of blood, circulating all over the body in an approximate time of 15-20 seconds.The pressure at which this blood moves across the body is called the blood pressure . Hypertension or simply , high blood pressure is an undesirable hemodynamic disturbance in human circulatory system.Systemic hypertension is the most common type of hypertension. The blood pressure is primarily dependent on the status of the blood vessel(vascular resistance) and cardiac contractility. This regulation is under many neural and hormonal factors.Further the blood pressure varies depending upon the blood vessel calibre, and the local milieu.There is a progressive drop in blood pressure from major arteries to the small arteries .The pressure drop is maximum across the arterioles to reach the venules .The venous circulation has the lowest pressure, it ends up at right atrium with a mean pressure of 0- 5mmhg.
Importance of regional variation of blood pressure.
It should be realised , each organ has it’s own regulated blood pressure.The brain perfuses by the intracerebral pressure .The lungs decide how much should be the pulmonary arterial pressure.The kidney not only controls it’s own pressure but also has a major regulatory role in systemic pressure by rennin angiotensin system.The examples are numerous, portal system has it’s unique pressure controlling hepatic hemodynamics. The retinal blood vessels regulate intra ocular pressure. While the human circulatory system has a wide variation of blood pressure across the breadth and length of vascular system, it is ironical a single snap shot BP with a brachial cuff is used to define the normality and if it is normal every thing is thought to be hunky dory !
It is widely acknowledged now , aging of humanity is nothing but aging of our vascular system
So we should have new parameters to assess individual organ’s vascular health as well as the currently popular systemic vascular health.The single important factor that determine coronary endothelial damage is the intra coronary pressure.It is never taken into account in any of the cardivascular mortality studies. This is the prime reason for the widely prevalent conflict in the cardiology literature , namely : Controlling systemic blood pressure has poor correlation with cardiovascular outcome. Many of the so called normotensive individuals have serious hemodynamic injury in their coronary arteries.This was made apparent in the ASCOT LLA study , in which patients with near normal blood pressure also benefited from statin therapy , implying endothelial damage could occur at any level of systemic blood pressure.
What is the normal intracoronary pressure ? When do you diagnose intracoonary hypertension?
The normal intracoronary pressure is around 40mmhg . Intra coronary hypertension as a clinical entity is yet to be recognised . There is no defintion available for intracoronary HT , intracerebral hypertension as well.
It’s still a long way to go , for the cardiology and neurology community to assess non invasively intracoronary pressures and intra cerebral arterial pressure to prevent coronary events ant strokes.
Final message
Simple risk prediction using brachial cuff blood pressure is a grossly unscientific method (Sorry, i really mean it ) to assess one’s vascular health.There has been few attempts like vascular endothelial health assessment by fore arm blood flow , central aortic pressure (Instead of brachial cuff pressure) as an index for risk predictment and assessment for hypertension is suggested.
Posted in Cardiology - Clinical, cardiology -Therapeutics, cardiology- coronary care, Infrequently asked questions in cardiology (iFAQs) | Tagged aging, blood pressure, bmj, cardiac output, drsvenkatesan, intra cerbral hypertension, intra coronary hypertension, jacc, jama, kaplan, lancet, nejm, peripheral vascular resistance, renal hypertension, systemic hypertension, venous system | Leave a Comment »
November 11, 2008 by dr s venkatesan
Angina pectoris , classically occur on exertion and gets relieved on rest .This is called typical chronic stable angina as described by Heberden (CSA ) . Unstable angina(UA), the term originally described by Noble O Fowler in early 1970s. ( Also being referred as intermediate coronary syndrome , preinfarction angina etc).The definition for unstable angina has evolved over the years and currently refers to .
1.All new onset angina of any degree* Some include severe angina only ! New onset angina of very mild degree on exertion could be the onset of the first episode of stable angina.
2.Rest angina of more than >30 mts not relieved by taking sublingual nitroglycerine.
3.All Post MI angina
4.Any angina in patients who have been stented by PCI.
How to recognise a patient who is shifting from stable angina to UA ?
UA is to be suspected when a patient develops.
5.More frequent episodes than usual
6.Angina occurring at lesser level of exertion than before
7.Angina radiating to new site ( Example : Chest pain radiating to jaw rather than to the usual left arm or vice versa)
Why the first episode of angina is given a special status and often considered critica ?
Angina is the clinical expression of myocardial ischemia.The course of the first episode of angina , can not be predicted.It could be a the beginning of a chronic disease process, or it could be a progressive coronary occlusion as in unstable angina /NSTMEI , or the onset of even a STEMI.
In contrast a patient with chronic stable angina has a predictable chest pain , at a particular level of exertion, radiation to same site, same character, and the patient knows for sure the pain would promptly dissappear when he takes rest or nitroglycerine tablets.
What is the underlying pathology in UA ?
Generally it is very rare for a stable plaque to produce a serious episode of unstable angina .It requires an unstable plaque* to precipitate an unstable angina !
Unstable plaque refers to any plaque which is eroded, fissured, ruptured or hanging eccentrically , with
an active thrombus.
What is the significance of post PCI angina?
It is an irony, any angina following PCI is to be considered unstable as sudden occlusion of stent is quiet common.This is a paradox of sorts as one would wonder in a patient with CSA who undergoes PCI with stenting of left anterior descending coronary artery (LAD) all his subsequent episodes of angina will be labelled as UA even if a stable angina occur in his other coronary artery.And these patients would go for early invasive approach and potentially inappropriate interventions even if they are at low risk !
Is all angina at rest can be termed as unstable angina ?
No, but many times , rather most of the times cardiologist believe all rest angina to be unstable.
What are the situations where stable angina can occur at rest?
An episode of angina during mental stress, or post prandial* state are very common in patients with CSA. This gets relieved after the stress. Some times patients with CSA during episodes of fever may get angina at rest .These are considered variants of stable angina.
Post prandial angina , may be considered by some as unstable
How often a diagnostic confusion occur between CSA and UA ?
Generally, this issue is rarely addressed in cardiology literature , for the simple reason it is never considered an issue at all !
According to Canadian cardiovascular society grade 4 stable angina is almost similar to unstable angina , as it denotes angina occurs with minimal effort or even at rest. In fact CCSC grade 4 should be termed as UA.
Can ECG be useful to identify stable angina from unstable angina ?
ECG will some times come to our rescue when one is confused between stable and unstable angina even though resting ST depression can occur in both stable and unstable angina . Statistically , if ST depression is noted during an episode of angina it is more likely to be UA rather than CSA. . Apart from ECG , Troponin T or I levels may be elevated in some of the patients with unstable angina. Rarely stable angina can also show elevated troponin.
In patients with systemic hypertension and LVH or cardiomyopathy resting ST depression may not indicate UA
So differentiation between, stable and unstable angina even though appear simple and straight forward, it requires a diligent appraisal of history , physical examination (Aortic stenosis /HCM may cause stable angina) and ECG, enzyme evaluation.
Final message
In any coronary care unit , admissions with initial diagnosis of ACS/UA/NSTEMI , subsequently turn out to be simple stable coronary artery disese . This error happens because the chest pain or ECG changes are aggravated by non cardiac factors like a mental stress or a post operative stress or fever etc.
There could be another school of thought, that is to err on the side of safety, and manage all rest angina as UA .But the hazards of unwarranted therapy might exceed the risks of leaving these patients alone.
In this context ,there is a need for a new definition for unstable angina .
One ideal version could be . . .
- Any angina , of any degree which is caused mainly by the supply side defect (By a acute thrombotic /disruptive plaque occluding the coronary lumen with a imminent danger of myocardial infarction is to termed as real UA.
- All post MI and post PCI angina are unstable angina
- Rest angina which occurs due to increased demand situations need not be labelled as unstable angina for the simple reason there is neither an active plaque nor a fresh thrombus likely in these patients. They rarely develop recurrent angina or MI . The mechanism of angina at rest here is most often due to a tachycardia and resultant increase in MVO2 .(myocardial oxygen consumption) .Currently they are called as secondary unstable angina.In fact , anti thrombotic drugs are misused in these situations as they satisfy the criteria of UA/NSTEMI.
Posted in Cardiology - Clinical, Cardiology -Interventional -PCI, cardiology -Therapeutics, cardiology- coronary care, Infrequently asked questions in cardiology (iFAQs) | Tagged acc.aha, angina grading, angina pectoris, beta blockers, braunwwald, canadian cardiovascualr society classifcation, cardiology, ccsc, chronic stable angina, drsvenkatesan, heberdeen, intermediate coronary syndrome, jacc, jama, lancet, nejm, nstemi, post infarct angina, post pci angina, ptca, rest angina, stable angina, stemi, unstable angina | 1 Comment »
« Newer Posts - Older Posts »















 A normally functioning circulatory system is vital for our survival . We have about 6000 ml of blood, circulating all over the body in an approximate time of 15-20 seconds.The pressure at which this blood moves across the body is called the blood pressure . Hypertension or simply , high blood pressure is an undesirable hemodynamic disturbance in human circulatory system.Systemic hypertension is the most common type of hypertension. The blood pressure is primarily dependent on the status of the blood vessel(vascular resistance) and cardiac contractility. This regulation is under many neural and hormonal factors.Further the blood pressure varies depending upon the blood vessel calibre, and the local milieu.There is a progressive drop in blood pressure from major arteries to the small arteries .The pressure drop is maximum across the arterioles to reach the venules .The venous circulation has the lowest pressure, it ends up at right atrium with a mean pressure of 0- 5mmhg.
A normally functioning circulatory system is vital for our survival . We have about 6000 ml of blood, circulating all over the body in an approximate time of 15-20 seconds.The pressure at which this blood moves across the body is called the blood pressure . Hypertension or simply , high blood pressure is an undesirable hemodynamic disturbance in human circulatory system.Systemic hypertension is the most common type of hypertension. The blood pressure is primarily dependent on the status of the blood vessel(vascular resistance) and cardiac contractility. This regulation is under many neural and hormonal factors.Further the blood pressure varies depending upon the blood vessel calibre, and the local milieu.There is a progressive drop in blood pressure from major arteries to the small arteries .The pressure drop is maximum across the arterioles to reach the venules .The venous circulation has the lowest pressure, it ends up at right atrium with a mean pressure of 0- 5mmhg.
