October 19, 2008 by dr s venkatesan
Acute coronary syndrome (ACS) is currently classified as STEMI and NSTEMI.This classification came into vogue primarily to triage patients for thrombolysis eligibility , as ST elevation is the only criteria for thrombolysis.The earlier term non q MI is largely used to denote the present day NSTEMI. In the past q MI was referring to transmural MI non q MI to non transmural pathologically.(Of course , now we know the relationship between q waves and transmurality is not good )
So when can we still use term non q MI ?
These terminologies of STEMI and NSTEMI are made on admission at the emergency room. ACS being a dynamic entity these patients can have rapidly changing ST shifts , from depression to elevation and vice versa. Fresh T wave changes can also occur .Q waves may or may not develop , depending upon the damage sustained to the myocardium and the efficacy of thrombolysis / PCI. So it should be emphasised here STEMI, NSTEMI , q MI , non q MI are the descriptions of the same group of patients in different time frames. The common mode of evolution of STEMI is to q MI and NSTEMI into non q MI. Cross overs can occur.
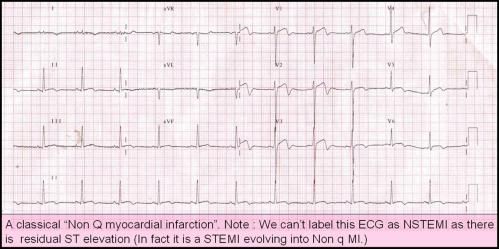
The problem here is NSTEMI getting converted into STEMI is quiet common and has no nomenclature issues . But when STEMI down grades into NSTEMI there is apparent nomenclature incompatibility .This category of patients have no other labelling option other than “A STEMI evolving into non q MI”. Because one can’t label STEMI evolving into NSTEMI as many of them will have a residual ST elevation as well.
What is the final message ?
The term non q MI is still relevant and is used at discharge , in a patient with STEMI when he or she evolves without a q wave .In the setting of unstable angina , NSTEMI has largely replaced the term non q MI either on admission or at discharge.
Before I close
The important point to remember here is NSTEMI getting converted into STEMI is an adverse outcome and in fact, it is a complication and the patient should get an immediate thrombolysis or PCI , while a STEMI getting converted into non Q MI is generally a major therapeutic success.( Effective salvaging and preventing q waves )
//
Posted in Cardiology -Interventional -PCI, cardiology- coronary care, Infrequently asked questions in cardiology (iFAQs) | Tagged acc aha, acute coronary syndrome, angina, cardiology- coronary care, circulation, drsvenkatesan, ECG, jacc, madras medical college, nejm, nstemi, st depression, st segment, stemi, unstable angina | 4 Comments »
October 19, 2008 by dr s venkatesan
Human civilisation has met so many challenges.Man kind has enjoyed the benefits of modern medicine for over a century.Now comes the new threat.Threat from within.The onslaught of marketing force has contaminated the medical science .
It is widely recognised commerce is masquereading as science , from stem cell research to futile and costly drugs, and questionable devices and procedures .
How is the medical community responding to this issue ?
Silence is the response ! Why silent ? Are we the part of the problem ? Occasional articles in the Annals of medicine, Lancet, BMJ, or JAMA talk about these issues and nothing happens next .
Click below to read one such article from the recent issue of Annals !

Let us hope the world financial crisis currently we are witnessing , would be good for human health as all futile market driven , enforced medical expenditure goes bust !
Posted in cardiology-ethics, Infrequently asked questions in cardiology (iFAQs) | Tagged annals of internal medicine, bmj, common sense based medicine, drsvenkatesan, ethics, evidence based medicine, fda, hippocrates, jama, lancet, nejm | Leave a Comment »
October 17, 2008 by dr s venkatesan
Non ST elevation Myocardial infarction (NSTEMI) is a major mode of presentation of acute coronary syndrome.
Patients present with clinical unstable angina and elevated cardiac enzymes or troponin.
ECG features can be any of the following.
1.ST depression (70-80%)
2.T wave inversion(10-20%)
3.Both ST depression and T wave inversion
4Post MI NSTEMI -ECG changes variable ( Ironically ,even a residual ST elevation may be present)
5.Normal ECG.
Bulk of the NSTEMI belong to ST depression group.NSTEMI with purely T wave inversion is less common but occurs mainly in perioperative settings, pre existing CAD.NSTEMI with normal ECG is very rare but can occur.
Posted in cardiology- coronary care | Tagged acs, nstemi, stemi, T WAVE INVERSION | Leave a Comment »
October 15, 2008 by dr s venkatesan
Rescue thrombolysis in acute myocardial Infarction
*Venkatesan sangareddi ,Madras medical college,Chennai.India


Back ground Failed thrombolysisin acute myocardial infarction occurs in 30-40% of patients. The incidence of progressive pathological remodelling and cardiac failure is high in these patients. The approach to the patient with failed thrombolysis is generally considered to be catheter based and the outcome is not clear. Bleeding can be troublesome in patients, taken for interventional procedures in the immediate post thrombolytic state. The option of repeat thrombolysis has not been studied widely and is not popular among cardiologists.
Methods:We present our experience with six patients (Age 42-56, M-6, F-0) who were thrombolysed for failed first thrombolysis. All had anterior MI and had received either urokinse or streptokinase (between four to nine hours) after the onset of chest pain. All of them had persistent ST elevation, angina not responsive to maximal doses of IV NTG and beta blockers. The initial thrombolysis was deemed to have failed. Repeat thrombolysis with streptokinase (15 lakhs) was given between 16 and 24 th hour. The clinical outcome following the second thrombolysis was rewarding. It relieved the angina, ST segment elevation came down by 50% and coronary angiogram done at 2-4 weeks showed complete IRA patency in four out of six patients. The factors responsible for failed thrombolysis is complex and multifactorial. A logical explanation from the fundamentals of clinical pharmacology would suggest that a common cause of failure of any drug is due to a inadequate first dose.
Conclusion :We conclude that repeat (Rescue) thrombolysis can be an effective medical intervention for failed thrombolysis in AMI.
Personal perspective
Repeat thrombolysis for failed ( initial ) thrombolysis is still considered a fantasy treatment by most of the cardiologists ! The utility and efficacy of this modality of treatment (Rescue thrombolyis ) , will never be known to humanity , as planning such a study , in a large population would promptly be called unethical by the modern day cardiologists.
While a cathlab based cardiologist take on the lesion head on with multiple attempts , it is an irony , poor thrombolytic agents are given only one shot and if failed in the first attempt, it is doomed to be a failure for ever.Currently, the incidence of failed thromolysis could be up to a whooping 50 % .There has not been much scientific initiative to enhance the efficacy of these drugs.
Common sense and logic would suggest it is the inadequate first dose , improper delivery , pharmacokinetics is the major cause of failure of action of a drug in clinical therapeutics.
If the first dose is not working , always think about another incremental dose if found safe to administer.
Can we increase the dose of thrombolytic agents as we like ? Will it not increase the bleeding risk to dangerous levels ?
This is a clinical trial question.
-
In patients with prosthetic valve thrombosis and acute pulmonary embolism we have safety data of administering of 1 lakh units for an hour for up to 48 hours.
Can the same regimen be tried in STEMI if the initial thrombolysis has failed and emergency intervention is not possible ?
Logic would say yes . Unfortunately we can’t go with logic alone in medicine .We need scientific data ( with or without logic ! ).But now , as we realise common sense is also a integral part of therapeutics It is called as level 3 evidence / expert consensus by AHA/ACC .
Applying mind , to all relevant issues , continuous streptokinase infusion 1 lakh/hour for 24-48 hours in patients with failed thrombolysis can indeed be an option, especially when the patient is sinking and no immediate catheter based intervention possible .This study question is open to all researchers , and may be tested in a scientific setting if feasible.
Posted in Cardiology -Interventional -PCI, cardiology -Therapeutics, My presentations | Tagged acute coronary, cardiogenic shock, cardiologist, drsvenkatesn, europcr, failed thrombolysis, lancet, nejm, nstemi, primary angioplasty, rescue angioplasty, rescue thrombolysis, scai, stemi, streptokinase, tctmd, thrombolysis, tnk tpa, tpa | 1 Comment »
October 14, 2008 by dr s venkatesan
The greatest discovery in medicine is “ common sense” and
“democracy”.
The greatest medical discovery is the realization that medicine is an constantly evolving science. It needs lot of knowledge to know our ignorance . Common sense has probably saved more lives and reduced suffering in this world than any other single discovery. Note this glaring irony ! It has required a large multi national long term follow up study (INTERHERT) to prove exercise and physical activity is good for health. Whatever science is teaching us it is we, with our sixth sense have to act appropriately .It is the only defense against the potential exploitation against man kind by various forces.
Another great development is the freedom of expression and democracy in medicine, for which journals like BMJ, Internet are striving hard . . .
Dr .S.Venkatesan ,Assistant professor of cardiology . Madras medical college Chennai , India
Click on the title to view the article and all nominations .


Posted in cardiology-ethics, Uncategorized | Tagged Add new tag, bmj, COMMON SENSE, ethics, INTERHEART | Leave a Comment »
October 11, 2008 by dr s venkatesan
Answer: Do coronary angiogram for all patients who had suffered from an acute myocardial infarction* ( Forget about all those mulitpage ACC/AHA guidelines !).
For an interventional cardiologist , it is often considered a crime to follow a conservative approach !
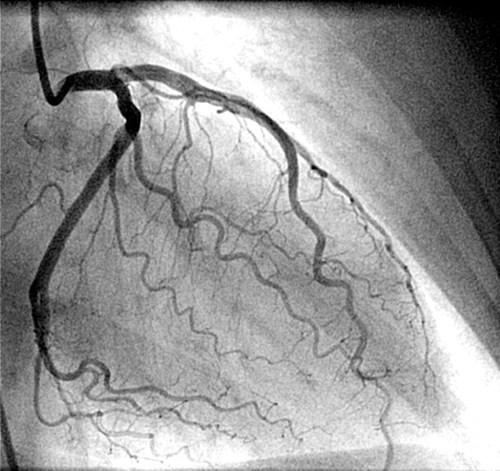
*Caution : This one line guideline is not based on scientific fact but reality based . Ideally one should identify high risk subsets among the patients who had an AMI .Patients who had complications during the MI get immediate CAG. Others need a focused LV function asessment , pre discharge sub maximal excercise stress test or perfusion studies .But this concept has been virtually replaced by pre discharge coronary angiogram for all , in many of the centres in the world.
Posted in Cardiology -Interventional -PCI, cardiology- coronary care, Infrequently asked questions in cardiology (iFAQs) | Tagged acc.aha, acc/aha guidelines for stemi, acute myocardial infarction, cath lab, conservative approach, coronary angiogram, drsvenkatesan, ethics, evidence based cardiology, excercise stress test, guidelines, interventional cardiologist, jacc, jama, lancet, nejm, nstemi, nuclear imaging, pci, pre discharge stress testing, pre discharge tmt, ptca, sestamibi, stemi, stent, streptokinase, sub maximal, thallium, thrombolysis | Leave a Comment »
October 10, 2008 by dr s venkatesan

dr s venkatesan ,venkatesan india , india venkatesan , dr venkatesan, cardiologist india, india cardiologist, indian cardiologist, chennai cardiologist, venkatesan madras,cardiologist madras medical college, venkatesan assistant professor of cardiology, top indian cardiologist, top ten cardiologist india, best cardiologist india, online cardiologist, consultant cardiologist chennai, india’s famous cardiologist,cardiological society of india,
Posted in dr s venkatesan -Personal | Tagged anna nagar, best cardiologist india, boiler plant high school, bphss, cardiological society of india, cardiologist, cardiologist india, cardiologist madras medical college, cardiologist tamilnadu, chennai, chennai cardiologist, coimbatore, coimbatre medical college, consultant cardiologist chennai, dr s venkatesan, dr venkatesan, famous, india, india cardiologist, india venkatesan, india's famous cardiologist, indian cardiologist, interventional cardiologist, kaniyalampatti, latha venkatesan, leading, madras, madras medical college, mani high school, on line heart care, online cardiologist, pudupatti, shreenila venkatesan, top, top indian cardiologist, top ten cardiologist india, venkatesan assistant professor of cardiology, venkatesan india, venkatesan madras, www.drsvenkatesan.com | 2 Comments »
October 10, 2008 by dr s venkatesan
One of the greatest physicians of all time, I have come across , is my professor Dr.T.K.Ganesan from Coimbatore medical college.

A man who taught medicine to generations of doctors.During those years (1980-1990) learning medicine was simple and also not contaminated with commerce . Dr TKG made it so lively .He infused passion in the subject.

Myself and Dr K.A.Sambasivam (Son in law of DrTKG at his residence in Coimbatore )
* Dr K.A .Sambasivam was my class mate during both my under and post graduation . He is now a senior Interventional cardiologist in GKNM Hospital Coimbatore .
This post will be updated.
Posted in dr s venkatesan -Personal | Tagged coimbatore medical college, dr s venkatesan, dr t k ganesan, professor t.k ganesan | 1 Comment »
October 9, 2008 by dr s venkatesan
During acute ischemia the most immediate requirement for the heart is
A.Blood
B.Oxygen
C.Glucose
D.High energy ATPs
E.Free fatty acid
Answer : A will be considered by most , as correct answer . A can provide B to E . But it is also a fact heart can survive without A.
Myocardium requires energy first ! it does not in fact bother about from where it is coming at the time of crises.It may be right if you restore the coronary blood flow all other components (B-E) are made available to the heart .
The heart can survive off the coronary circulation with only chemical support during cardiac surgery and also a during heart transplantation explanted donor heart survives on a ice box during transit and till it is transplanted into the recipient heart
But ironically we spend much of our energy and efforts in restoring blood flow.One need to spare a thought about the quality of blood also . This is especially important in the setting of ischmia where a metabolic centric approach will add further benefit.

Energy based approach to ischemia : Is it relevent ?
Heart is a fascinating mechano biological organ pumping millions of gallons of blood .Fuel for this is self generated on a continuous basis from the circulation blood .So the key to human survival is the coronary blood flow that supplies the fuel and nutrients to the heart. When this key supply line is under threat during acute coronary syndrome cardiologist have the only option of restoring the compromised blood supply by any means . But during chronic ischemia there is no urgency. There has always been an option of enriching the blood with energisers like ATPs, glucose, hemoglobin etc .Providing energy support to the failing heart has never captured the imagination of cardiac physicians until recently.Still most are skeptical about the concept of biochemical ischemia.
Click to download full PPT presentation
Metabolic manipulation of CAD( Will be available shortly)
Posted in Cardiology - Clinical, Cardiology -Interventional -PCI, cardiology -Therapeutics, cardiology- coronary care, Infrequently asked questions in cardiology (iFAQs) | Tagged acs, angina, atp, biochemical ischemia, cardiac failure, chronic stable angina, coronary, fatty acid, glucose, ischemia, ketoacid, metabolic modulation, mitochondrial energetics, myocardial energetics, ranalozine, trimetazidine, unstable angina | Leave a Comment »
October 9, 2008 by dr s venkatesan
Humans have roughly 5 to 6 liters of blood at any given time in their body . Out of this*
50% (2500ml) is located in the systemic venous compartment.
18% is within the pulmonary circulation participating in the vital oxygenation
12% (500-600ml) is within the cardiac chambers.
8% is in the arterial tree of the body.
5% is within the capillaries.
2% is in the aorta.
* Source : Best & Taylor Physiological basis of medical practice 1966, 8th edition
What is the implication of this predominantly venous distribution of blood at rest ?
- A competent venous tone is essential for the human beings to maintain the erect posture.
- Bulk of the cause of syncope in humans is due to peripheral mechanism like loss of vascular tone and resultant venous pooling.
- The concept of venous reservoir is so important in emergency situations like hypotension as simple elevation of legs is equivalent to infusing 500 -800 ml of intravenous saline .
- Similarly during acute left ventricular failure trunk elevation and legs dangling down can reduce the pulmonary congestion very significantly and reduce pulmonary capillary wedge pressure (LVEDP)
Autonomic dysfunction and venous insufficiency
Autonomic dysfunction and resultant orthostatic hypotension is directly related to venous reservoir dysfunction.Increasing effective circulatory volume by elastic stockings or administration of mineralocorticosteroids like fludrocortisone (.5mg/day ) can be useful in this condition
Posted in Cardiology - Clinical, cardiology -Therapeutics, Infrequently asked questions in cardiology (iFAQs) | Tagged autonomic dysfunction, blood volume, bmj, capillary, cardiac output, cardiology, drsvenkatesan, effective circulatory volume, fludrocortisone, heart, Hemodynamics, lnacet, lvedp, nejm, ortho static hypotension, pcwp, physiology of circulation, pulmonary edema, syncope, venous circulation, venous insufficiency, venous pooling | Leave a Comment »
« Newer Posts - Older Posts »











