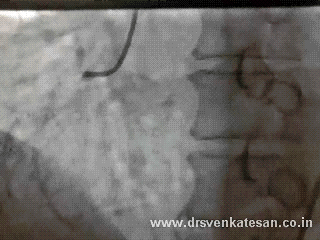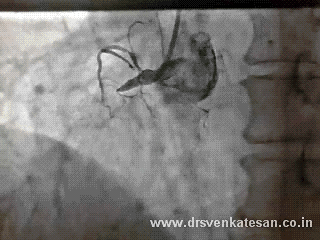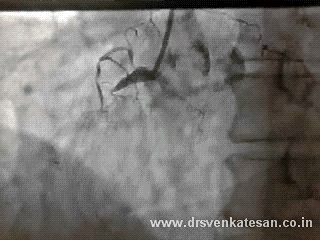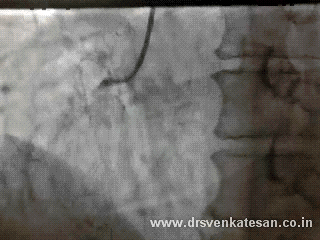
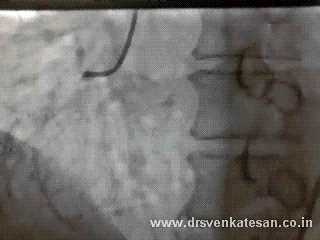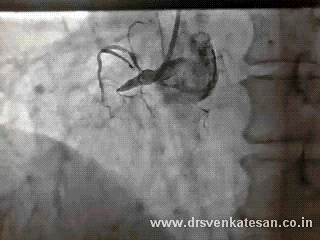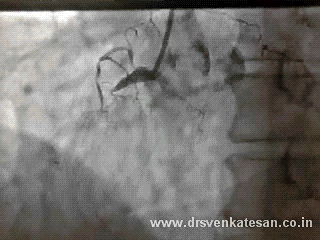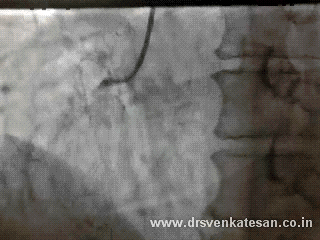
Acute STEMI is the numero uno of all medical emergencies. Hundreds of life are lost every few hours in our planet.Significant chunk of them do not even reach the hospital alive . While the emergency crew has many vital responsibilities , the cardiologist job starts only after the patient reaches the hospital . Hence the ambulance crew need to act much more sharper. Please remember even the skills of the driver will have a direct impact on the myocyte survival.
The symptom to first medical ( or second hospital ) contact could be as vital as a primary PCI procedure itself . A 3 minute traffic jam can kill 3 thousand myocytes ! One could imagine the importance of decision making process here.
Distance from the point of contact to PCI lab , the anticipated delay , intensity of traffic matters .
Is it not funny , to realise when we have a reperfusing agent on hand , within the ambulance and the vehicle stuck in the traffic jam waiting to reach a reperfusion room situated 50 km down the high way !
( One may wonder why can’t we thrombolyse every one routinely in the ambulance and do the PCI later in . . . But surprisingly this concept simply does not work !)
When we realise , even in a well developed country like Netherlands , time to shift to cath lab is a big issue (Read the following article ) we will never ever know , how much of myocardium is consumed by traffic jams in a country like India , where the traffic scenarios can be more chaotic than a VF !
Events that unfold following a STEMI are crucial
It begins with chest pain recognition.
Call for first help Spouse/Family doctor /Neighbor
Call for 911/108 . Ambulance arrival time and boarding
Administration of Aspirin + clopidogrel*
Meanwhile spontaneous thrombolysis will begin in most of them !
A promptly administered Aspirin and clopidogrel a shot of heparin and a lytic agent within 30 minutes is distinctly possible and may be more effective at a fraction of cost.
Highway thrombolysis
Even though current studies still . . .do not favor primary PCI over thrombolyiss in the first hour , most of the cardiologist do show some favoritism towards pPCI for some unknown reasons.
So by default , many of the ill fated STEMI patients enter an unrealistic hemodynamic race in the deadly highways and urban lanes our country !
For every minute that goes by , the patient not only loses his muscle but also the golden opportunity to get salvaged by the thrombolytic agents .
Since , a delay beyond one hour eliminates the indication of thrombolysis (if a cath lab is available in the vicinity ) many times traffic delays convert a potential hyperacute thrombolysis into a say . . . 3-6 hour old PCI .(Should we feel happy about it ?)
Here , we need to know TIMI 2 flow achieved easily by thrombolytic agents is quiet effective in preventing myocyte death.
Fast track shift to PCI
Helicopter drop over cath lab -( Distant dream ? or better to be in dreams ) It has been noticed even a helicopter was squarely beaten by the thrombolysis in terms of early and timely reperfusion.
Fast -Slow track PCI ? (Like fast slow AVNRT !)
Unexpected delays on road , in many countries financial issues /Insurance sanction etc contribute to the time delay significantly . What starts as a fast track protocol peters out into slow race (Late primary PCI ) and may even end in a grinding halt.(No primary PCI )
Worse still . . . some of these patients are made unsuitable for thrombolysis as well !
Final message
Management of STEMI is gradually becoming a team effort. The emergency crew , the command , the destination hospital all need to be alert and proactive. When the initial anticipated delay is getting prolonged , get the ground staff in cath lab ready for an emergency landing .
A word of advice for the ambulance crew .Involve them more in the decision making as they are in a better position to calculate the possible delay. If delays are anticipated propose a thrombolytic order and get clearance from the command and administer the lytic agent as early as possible.
It is highly likely , restoration of TIMI 2 flow right in the middle of national highways is much . . . better than a TIMI 3 flow that is going to come later . . .in a distant cath lab .
Finally use the common sense liberally before you act . . . unfortunately it has become the most elusive sense for man kind !
References :
Here is a study that gives a fresh insight into this enigmatic issue of pre-hospital thrombolysis vs primary PCI