November 2, 2008 by dr s venkatesan
Which is the most important factor that determines thrombolysis failure in STEMI ?
- Thrombus load .
- Drug efficiency
- Time delay
- Presence of a mechanical lesion
- Hemodynamic instability
Answer : 3 .(Though all 5 factors operate )
Failed thrmbolysis occur in about 40-50% after streptokinase and slightly less with TPA and TNK-TPA . Delayed arrival and late thrombolysis are most common cause of failed thrombolysis. As the time flies , the myocardium gets damaged and the intra coronary thrombus gets organised .Both these processes make delayed thrombolysis a futile exercise.
Not all STEMI patients have large thrombus burden. There need to be a critical load of thrombus for thrombolytic to be effective
Some may have a major mechanical lesion in the form of plaque fissure, prolapse and it simply blocks the coronary artery mechanically like a boulder on the road . The poor streptokinse or the rich Tenekteplace ! nothing can move this boulder .The only option here is emergency PCI .
How will you know when the patient arrives in ER with STEMI whether his/ her coronary artery is blocked with soft thrombus or hard mechanical boulder ?
It is impossible to know.That’s why primary PCI has a huge advantage. But still thrombolysis is useful as some amount of thrombus will be there in all patients with STEMI.Lysing this will provide at least a trickle of blood flow that will jeep the myocardium viable and enable us to take for early PCI.
Final message
The commonest cause for thrombolytic failure is the time of administration and the degree of underlying mechanical lesion . So it does not make sense to blame streptokinase always !
Posted in Cardiology -Interventional -PCI, cardiology- coronary care, Infrequently asked questions in cardiology (iFAQs) | Tagged bmj, cardiology, coronary, drsvenkatesan, failed thrombolysis, jacc, lancet, nejm, nstemi, stemi, streptokinase, tenekteplace, thrombolysis, tpa | Leave a Comment »
November 2, 2008 by dr s venkatesan
Hypertension is considered a major cardiovascular risk factor.Hypertension can have multiple physiological and pathological effects on heart . The common response to raised arterial pressure is the hypertrophy of the left ventricle ( LVH). This can increase the risk of heart failure in few ( Mainly diastolic failure) It is a leading cause for stroke and less often a coronary event.
What links Hypertension and coronary artery disease

Coronary artery disease is almost synonymous with atherosclerosis. There is no separate entity called hypertensive coronary artery disease. But HT can accelerate the process of atherosclerosis. It is widely understood, hypertension can cause physical endothelial damage and functional impairment of endothelial function.The physical damage ie enothelial disruption , or erosion is a very uncommon phenomenon . So currently there is sufficient clinical experience HT is considered dangerous for coronary artery only if it is with the company of diabetes and hyperlipidemia. (This will seem controversial as it is against the findings of iconic Framingham trial!)
What the medical community refers to hypertension , may not be really so inside for the coronary arteries.
The relationship between brachial cuff blood pressure and the intra coronary pressure has very little linear relationship. So one should recognise it is the intra coronary hypertension that has a immediate impact on the coronary events. Now only , we are beginning to understand the complexities of the relationship between HT and CAD. If we analyse a series of individuals HT per se is not a very serious risk factor for CAD* , but it is a number one risk factor for stroke.
Why HT in isolation often result in stroke , rather than a MI ?
While HT is notoriously common to result intracerebral hemorrhage, the same HT would not cause intramyocardial bleeds . Why ?
What is protecting the myocardium against this complication ?
The exact mechanism is not clear.Acute surges of blood pressure can increase the risk of stroke many times but rarely precipitate a coronary event( But may cause a LVF) . The reasons could be the coronary endothelial shearing stress is less than the cerebral blood vessels.Both cerebral and coronary circulation has auto regulatory mechanism . The coronary auto regulation is more robust in that it does not allow intra coronary pressures to reach critical levels .There is no clinically relevant intra myocardial hemorrhage reported even during malignant hypertension.
*But a high intra coronary pressure can sometimes result in spontaneous coronary dissection and plaque fissure .Lipid mediated injury is vey much facilitated in a high pressure environment.
Has Controlling blood pressure to optimal levels , reduced the overall CAD morbidity and mortality ?
The answer is yes, ( But not an emphatic yes ! ) Some studies had been equivocal. It is very difficult to say , how much benefit is attributable to BP reduction per se and how much is attributable to indirect effect on atherosclerosis prevention.
Hypertension during ACS
High blood pressure during an episode of unstable angina or STEMI can increase the myocardial oxygen demand and worsen the ischemia. It requires optimal control with nitroglycerine ( Preferably ) or beta blocker and ACE inhibitors.Even though HT is commonly associated with ACS, one can not be sure the ACS is preciptated by HT. Many times the sympathetic surge during an ACS keeps the blood pressure high.It is a common experience the blood pressure suddenly dropping to normal or hypotensive levels once the pain and anxiety is controlled.
Hypertension during thrombolysis
High blood pressure is a relative contraindication for thrombolysis.It need to be emphasised here, It is the the fear of stroke that make it contraindicated .The heart can tolerate thrombolytic agents delivered at high BP .In fact logically , hemodynamically and also practically it is obseved , thrombolytic agents administered at relatively high blood pressure (140-160 systolic) has better thrombolysis than a patient who is lysed at 100mmhg.
The coronary pressure head which contain the thrombolytic agent (streptokinase and others ) need to have pressure jet effect on the thrombus.So the mean coronary perfusion pressure becomes a critical determinant of success of thrombolysis.
It is a paradox of sorts , very high blood pressures are a relative contraindication for thrombolysis and at the same time normal pressure patients fare less well to thrombolysis.
Final message
Hypertension continues to be a major cardiovascular risk factor.It has direct and indirect effects on the heart.Generally HT is more of a risk factor for stroke than CAD.A slightly high BP ( Just around the upper limits of normal or just above it ) has a hemodynamic advantage during thrombolysis.(Class C evidence )
Posted in Cardiology -Interventional -PCI, cardiology -Therapeutics, cardiology- coronary care, Infrequently asked questions in cardiology (iFAQs) | Tagged acs, auto regulation, bmj, coronary angiogram, coronary risk factor, failed thrombolysis, hypertension, intra cerbral hemmorhage, intra coronary hypertension, intra coronary pressure, jacc, lancet, left ventricualr hypertrophy, myocardium, nejm, nstemi, stemi, streptokinase, stroke, systemic hypertension. cva, thrombolysis | Leave a Comment »
October 31, 2008 by dr s venkatesan
What is herd behavior ?
It is a behavioral pattern where in animals and humans in large numbers , tend to behave in the same way at the same time without application of mind .
Herd behavior in human societies
Herd behaviour describes how individuals in a group can act together without planned direction. The term pertains to the behaviour of animals in herds, flocks, and schools, and to human conduct during activities such as stock market bubbles and crashes, street demonstrations, sporting events, episodes of mob violence and even everyday decision making, judgement and opinion forming. This is very much applicable to medical profession also.(Ref:Wikipedia)
Herd behaviour in animals and human how they are different ?
“surprise ! surprise ! There is very little difference noted , according to Hamilton”
A group of animals fleeing a predator shows the nature of herd behavior. In the often cited article “Geometry For The Selfish Herd,” evolutionary biologist W. D. Hamilton said each individual group member reduces the danger to itself by moving as close as possible to the center of the fleeing group. Thus the herd appears to act as a unit in moving together, but its function emerges from the uncoordinated behavior of self-seeking individuals.
Among humans for example when panicked individuals confined to a room with two equal and equidistant exits, a majority will favor one exit while the minority will favor the other.
Medical professionals as a herd

The practicing habits of medical professionals move , symmetrically as a herd . When a top journal or a opinion leader utters something every one tend to move in that direction .
If a herd leader says a particular treatment is great, every one will say yes . If he says nay every one will say nay !
No one will really question the direction they move ? Unless the correction occurs from within the herd. No external forces usually are effective.Herding is also benefitial many times as rapid propogation of scientific facts needs such behavior ,but it needs constant scrutiny.
Herd behavior example 1 : The most typical example is the drug prescribing pattern of anti hypertensive agents over the past half century.The movement from diuretics to beta blocker , from beta blockers to calcium blockers and to ACE inhibitor and again to diuretic , then to ARBs and currently shying strongly away from beta blockers, in between have a brief encounter with alpha blockers and finally back to diuretics.
If a particular physician by his insight , had clinged onto diuretics ( Away from the herd ) for over three decades he is a real exemption , although branded old timed and unscientific , he has been the most scientific medical professional indeed !
Herd mentality example 2 : Every one says so ! so it must be true ! Hormone replacement therapy good or bad goes with the leader of the herd .
Herd mentality example 3: Very few cardiologists will be ready to agree the fact that , simple digoxin and diuretic ,ACEI, beta blocker, administration could be as effective as the costly cardiac resynchronisation therapy in atleast some of patients with wide QRS cardiac failure ( As we know up to 30 % wide QRS CHF population do not respond to CRT)
Defying Herd mentality resulted in major break throughs in medicine
When every one was saying beta blocker was harmful in CHF one person from Briton defied it ( Wagenstein, and now beta blockers are the mainstay in the management of CHF! )
There are hundreds of treatment modalities popularised by such herd behavior
Who is the watch dog , whether science is moving in the correct direction ?
Read this land mark article how medical research can be distorted by such learned behavior and how scientific research should not be done .
Click on the image .

This post is not intended to hurt anyone . It reflects , human beings are not fully evolved yet , in the onging process of evolutionary biology.
Posted in cardiology-ethics | Tagged annals of internal medicine, bmj, cardiology, drsvenkatesan, ethics in medicine, herd behavior, lancet, medicine, nejm | Leave a Comment »
October 20, 2008 by dr s venkatesan
The superior aspect of coronary sinus and a portion of the left atrium share a common wall .Embryological defects in this area result in a communication between left atrium and coronary sinus. This defect descriptively called as unroofed coronary sinus .This entity is most commonly associated with persistent left SVC. Extreme form of unroofing is some times termed as absent coronary sinus.

How to diagnose it ?
A high degree of anticipation is necessary in all patients with ASD or LSVC. A dilated coronary sinus in routine echocardiography warrants full investigation. A contrast echocardiography with agitated saline injection in left cubital vein will clinch the diagnosis as contrast enters LA after opacifying the dilated coronary sinus. During right heart catheterisation catheter course entering coronary sinus and advancing into LA through the fenestrations (Unroofing) will confirm the defect.
How do you classify unroofed coronary sinus ?
The morphologic type of URCS was classified as Kirklin and Barratt-Boyes
Type I, completely unroofed with LSVC;
Type II, completely unroofed without LSVC;
Type III, partially unroofed midportion;
Type IV, partially unroofed terminal portion
What is the clinical relevance of this entity ?
This entity should be suspected in every patient with persistent LSVC, ( and LSVC should be suspected in every patient with ASD). The hemodynamics is that of an ASD but if sufficient mixing of LSVC blood and LA blood takes place the child will have mild cyanosis.Some times when the coronary sinus is totally absent it will present as a typical dusky ASD picture which can closely mimic a TAPVC clinically.
Surgeons have a greater role in recognising and treating this entity. A typical repair will be done like this
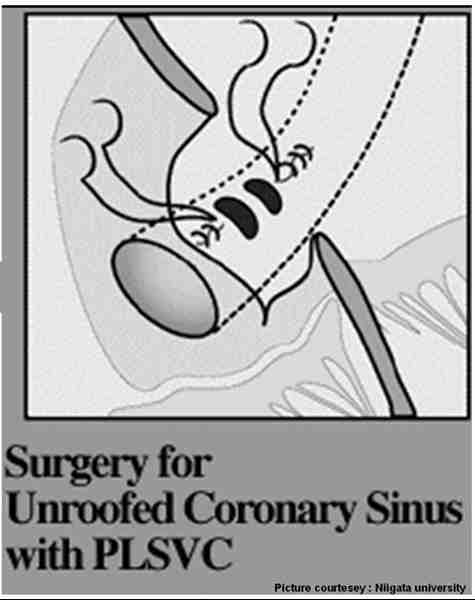
Links to some of interesting articles on this topic
Raghib circulation 1965
Posted in cardiology -congenital heart disease, cardiology congenital heart disese | Tagged ATRIAL SEPTAL DEFECT, cardiology, congenital heart disese, contrast echocardiography, CORONARY SINUS, coronary sinus asd, cyanosis in asd, dilated coronary sinus, drsvenklatesan, madras medical college, PERSISTENT LEFT SVC, ucla, unroofed coronary sinus | 1 Comment »
October 19, 2008 by dr s venkatesan
Acute coronary syndrome (ACS) is currently classified as STEMI and NSTEMI.This classification came into vogue primarily to triage patients for thrombolysis eligibility , as ST elevation is the only criteria for thrombolysis.The earlier term non q MI is largely used to denote the present day NSTEMI. In the past q MI was referring to transmural MI non q MI to non transmural pathologically.(Of course , now we know the relationship between q waves and transmurality is not good )
So when can we still use term non q MI ?
These terminologies of STEMI and NSTEMI are made on admission at the emergency room. ACS being a dynamic entity these patients can have rapidly changing ST shifts , from depression to elevation and vice versa. Fresh T wave changes can also occur .Q waves may or may not develop , depending upon the damage sustained to the myocardium and the efficacy of thrombolysis / PCI. So it should be emphasised here STEMI, NSTEMI , q MI , non q MI are the descriptions of the same group of patients in different time frames. The common mode of evolution of STEMI is to q MI and NSTEMI into non q MI. Cross overs can occur.
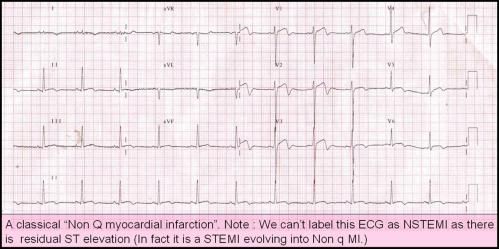
The problem here is NSTEMI getting converted into STEMI is quiet common and has no nomenclature issues . But when STEMI down grades into NSTEMI there is apparent nomenclature incompatibility .This category of patients have no other labelling option other than “A STEMI evolving into non q MI”. Because one can’t label STEMI evolving into NSTEMI as many of them will have a residual ST elevation as well.
What is the final message ?
The term non q MI is still relevant and is used at discharge , in a patient with STEMI when he or she evolves without a q wave .In the setting of unstable angina , NSTEMI has largely replaced the term non q MI either on admission or at discharge.
Before I close
The important point to remember here is NSTEMI getting converted into STEMI is an adverse outcome and in fact, it is a complication and the patient should get an immediate thrombolysis or PCI , while a STEMI getting converted into non Q MI is generally a major therapeutic success.( Effective salvaging and preventing q waves )
//
Posted in Cardiology -Interventional -PCI, cardiology- coronary care, Infrequently asked questions in cardiology (iFAQs) | Tagged acc aha, acute coronary syndrome, angina, cardiology- coronary care, circulation, drsvenkatesan, ECG, jacc, madras medical college, nejm, nstemi, st depression, st segment, stemi, unstable angina | 4 Comments »
October 19, 2008 by dr s venkatesan
Human civilisation has met so many challenges.Man kind has enjoyed the benefits of modern medicine for over a century.Now comes the new threat.Threat from within.The onslaught of marketing force has contaminated the medical science .
It is widely recognised commerce is masquereading as science , from stem cell research to futile and costly drugs, and questionable devices and procedures .
How is the medical community responding to this issue ?
Silence is the response ! Why silent ? Are we the part of the problem ? Occasional articles in the Annals of medicine, Lancet, BMJ, or JAMA talk about these issues and nothing happens next .
Click below to read one such article from the recent issue of Annals !

Let us hope the world financial crisis currently we are witnessing , would be good for human health as all futile market driven , enforced medical expenditure goes bust !
Posted in cardiology-ethics, Infrequently asked questions in cardiology (iFAQs) | Tagged annals of internal medicine, bmj, common sense based medicine, drsvenkatesan, ethics, evidence based medicine, fda, hippocrates, jama, lancet, nejm | Leave a Comment »
October 17, 2008 by dr s venkatesan
Non ST elevation Myocardial infarction (NSTEMI) is a major mode of presentation of acute coronary syndrome.
Patients present with clinical unstable angina and elevated cardiac enzymes or troponin.
ECG features can be any of the following.
1.ST depression (70-80%)
2.T wave inversion(10-20%)
3.Both ST depression and T wave inversion
4Post MI NSTEMI -ECG changes variable ( Ironically ,even a residual ST elevation may be present)
5.Normal ECG.
Bulk of the NSTEMI belong to ST depression group.NSTEMI with purely T wave inversion is less common but occurs mainly in perioperative settings, pre existing CAD.NSTEMI with normal ECG is very rare but can occur.
Posted in cardiology- coronary care | Tagged acs, nstemi, stemi, T WAVE INVERSION | Leave a Comment »
October 15, 2008 by dr s venkatesan
Rescue thrombolysis in acute myocardial Infarction
*Venkatesan sangareddi ,Madras medical college,Chennai.India


Back ground Failed thrombolysisin acute myocardial infarction occurs in 30-40% of patients. The incidence of progressive pathological remodelling and cardiac failure is high in these patients. The approach to the patient with failed thrombolysis is generally considered to be catheter based and the outcome is not clear. Bleeding can be troublesome in patients, taken for interventional procedures in the immediate post thrombolytic state. The option of repeat thrombolysis has not been studied widely and is not popular among cardiologists.
Methods:We present our experience with six patients (Age 42-56, M-6, F-0) who were thrombolysed for failed first thrombolysis. All had anterior MI and had received either urokinse or streptokinase (between four to nine hours) after the onset of chest pain. All of them had persistent ST elevation, angina not responsive to maximal doses of IV NTG and beta blockers. The initial thrombolysis was deemed to have failed. Repeat thrombolysis with streptokinase (15 lakhs) was given between 16 and 24 th hour. The clinical outcome following the second thrombolysis was rewarding. It relieved the angina, ST segment elevation came down by 50% and coronary angiogram done at 2-4 weeks showed complete IRA patency in four out of six patients. The factors responsible for failed thrombolysis is complex and multifactorial. A logical explanation from the fundamentals of clinical pharmacology would suggest that a common cause of failure of any drug is due to a inadequate first dose.
Conclusion :We conclude that repeat (Rescue) thrombolysis can be an effective medical intervention for failed thrombolysis in AMI.
Personal perspective
Repeat thrombolysis for failed ( initial ) thrombolysis is still considered a fantasy treatment by most of the cardiologists ! The utility and efficacy of this modality of treatment (Rescue thrombolyis ) , will never be known to humanity , as planning such a study , in a large population would promptly be called unethical by the modern day cardiologists.
While a cathlab based cardiologist take on the lesion head on with multiple attempts , it is an irony , poor thrombolytic agents are given only one shot and if failed in the first attempt, it is doomed to be a failure for ever.Currently, the incidence of failed thromolysis could be up to a whooping 50 % .There has not been much scientific initiative to enhance the efficacy of these drugs.
Common sense and logic would suggest it is the inadequate first dose , improper delivery , pharmacokinetics is the major cause of failure of action of a drug in clinical therapeutics.
If the first dose is not working , always think about another incremental dose if found safe to administer.
Can we increase the dose of thrombolytic agents as we like ? Will it not increase the bleeding risk to dangerous levels ?
This is a clinical trial question.
-
In patients with prosthetic valve thrombosis and acute pulmonary embolism we have safety data of administering of 1 lakh units for an hour for up to 48 hours.
Can the same regimen be tried in STEMI if the initial thrombolysis has failed and emergency intervention is not possible ?
Logic would say yes . Unfortunately we can’t go with logic alone in medicine .We need scientific data ( with or without logic ! ).But now , as we realise common sense is also a integral part of therapeutics It is called as level 3 evidence / expert consensus by AHA/ACC .
Applying mind , to all relevant issues , continuous streptokinase infusion 1 lakh/hour for 24-48 hours in patients with failed thrombolysis can indeed be an option, especially when the patient is sinking and no immediate catheter based intervention possible .This study question is open to all researchers , and may be tested in a scientific setting if feasible.
Posted in Cardiology -Interventional -PCI, cardiology -Therapeutics, My presentations | Tagged acute coronary, cardiogenic shock, cardiologist, drsvenkatesn, europcr, failed thrombolysis, lancet, nejm, nstemi, primary angioplasty, rescue angioplasty, rescue thrombolysis, scai, stemi, streptokinase, tctmd, thrombolysis, tnk tpa, tpa | 1 Comment »
October 11, 2008 by dr s venkatesan
Answer: Do coronary angiogram for all patients who had suffered from an acute myocardial infarction* ( Forget about all those mulitpage ACC/AHA guidelines !).
For an interventional cardiologist , it is often considered a crime to follow a conservative approach !
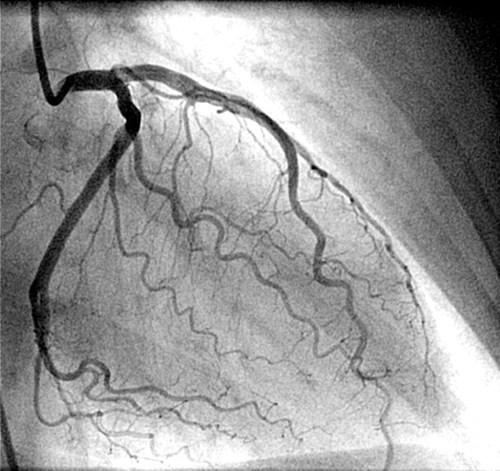
*Caution : This one line guideline is not based on scientific fact but reality based . Ideally one should identify high risk subsets among the patients who had an AMI .Patients who had complications during the MI get immediate CAG. Others need a focused LV function asessment , pre discharge sub maximal excercise stress test or perfusion studies .But this concept has been virtually replaced by pre discharge coronary angiogram for all , in many of the centres in the world.
Posted in Cardiology -Interventional -PCI, cardiology- coronary care, Infrequently asked questions in cardiology (iFAQs) | Tagged acc.aha, acc/aha guidelines for stemi, acute myocardial infarction, cath lab, conservative approach, coronary angiogram, drsvenkatesan, ethics, evidence based cardiology, excercise stress test, guidelines, interventional cardiologist, jacc, jama, lancet, nejm, nstemi, nuclear imaging, pci, pre discharge stress testing, pre discharge tmt, ptca, sestamibi, stemi, stent, streptokinase, sub maximal, thallium, thrombolysis | Leave a Comment »
October 10, 2008 by dr s venkatesan

dr s venkatesan ,venkatesan india , india venkatesan , dr venkatesan, cardiologist india, india cardiologist, indian cardiologist, chennai cardiologist, venkatesan madras,cardiologist madras medical college, venkatesan assistant professor of cardiology, top indian cardiologist, top ten cardiologist india, best cardiologist india, online cardiologist, consultant cardiologist chennai, india’s famous cardiologist,cardiological society of india,
Posted in dr s venkatesan -Personal | Tagged anna nagar, best cardiologist india, boiler plant high school, bphss, cardiological society of india, cardiologist, cardiologist india, cardiologist madras medical college, cardiologist tamilnadu, chennai, chennai cardiologist, coimbatore, coimbatre medical college, consultant cardiologist chennai, dr s venkatesan, dr venkatesan, famous, india, india cardiologist, india venkatesan, india's famous cardiologist, indian cardiologist, interventional cardiologist, kaniyalampatti, latha venkatesan, leading, madras, madras medical college, mani high school, on line heart care, online cardiologist, pudupatti, shreenila venkatesan, top, top indian cardiologist, top ten cardiologist india, venkatesan assistant professor of cardiology, venkatesan india, venkatesan madras, www.drsvenkatesan.com | 2 Comments »
« Newer Posts - Older Posts »












