We know, electrical deaths constitute the bulk of sudden cardiac deaths in MI. Mechanical deaths due to pump failure, muscle rupture , valve leak , also cause significant deaths .(Surprisingly many of the mechanical deaths may also fulfill the sudden death criteria !)
Free wall rupture is invariably a fatal event. Papillary muscle trunk rupture leads to severe LVF and unless intervened sure to result in fatality.
The ones who tear their interventricular septum are some what blessed ! Here , the rupture does not result in instant death as there is no loss of blood , instead , there is an volume over load of right ventricle followed by the left ventricle after a few beats. Hypotension is the rule. Even though this is a major complication there is something about VSR which makes it unique.
Sudden giving way of IVS has a decompressing effect on the ailing left ventricle.This many times bring a temporary relief to LV and if the patient survives the first few hour he is likely to stabilise further . In fact , sudden deaths within 24hours after the onset of VSR is an exception.This defect always gives the cardiologists and surgeon some time to plan the management. We need to use this time judiciously.
The natural history is delicate . Five themes are possible
- Very unstable – Instant death( Fortunately a rare theme )
- Unstable – Deteriorating further
- Unstable to Stable * fit for discharge even without surgery
- Stable from the onset and continue to be stable* .
- Stable to Unstable (Probably the most common theme )
* Pleasant themes occasionally witnessed !)
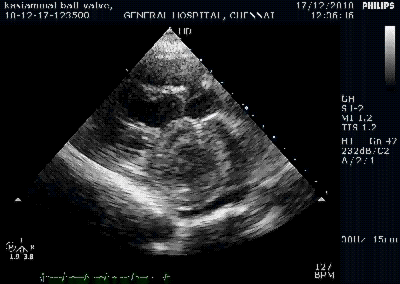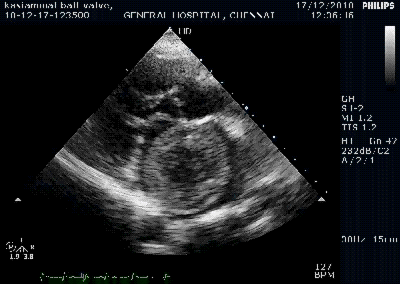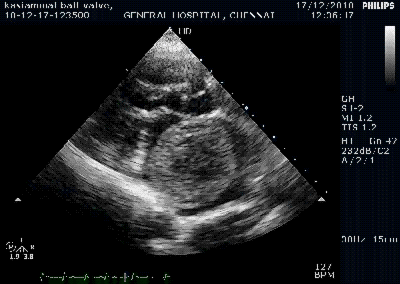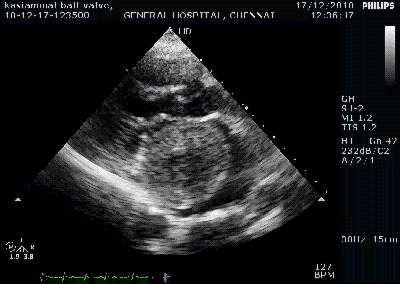
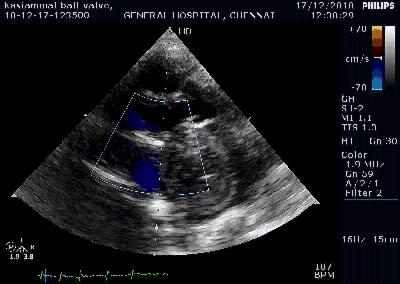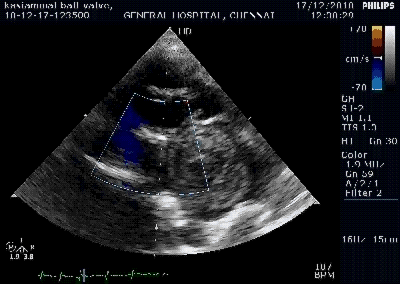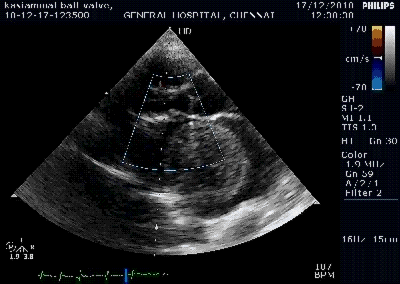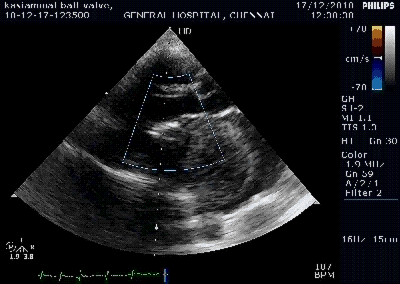
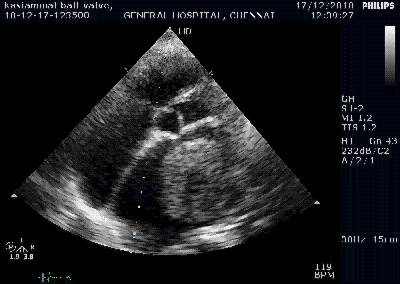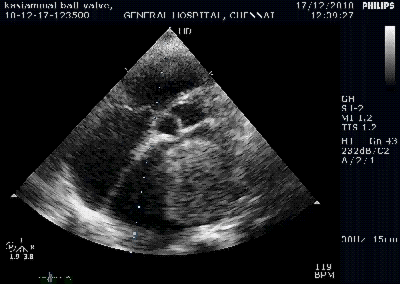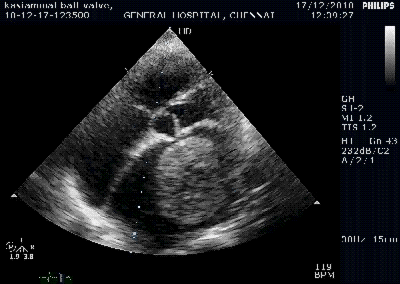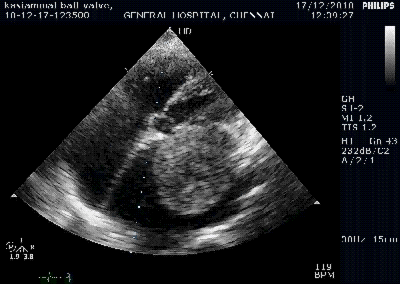
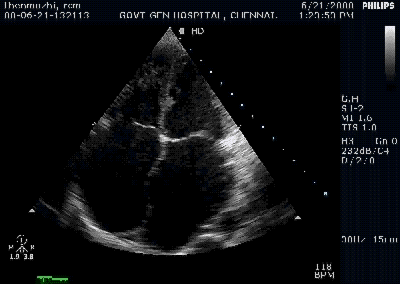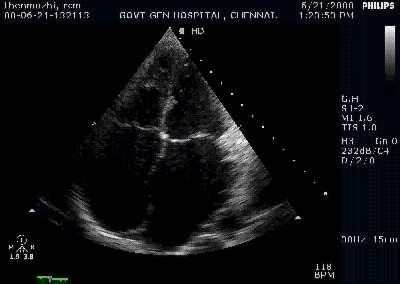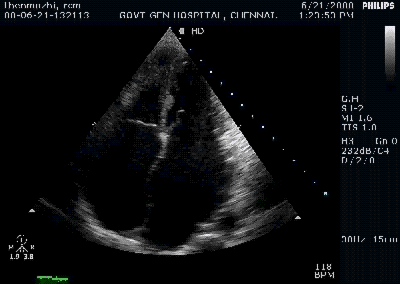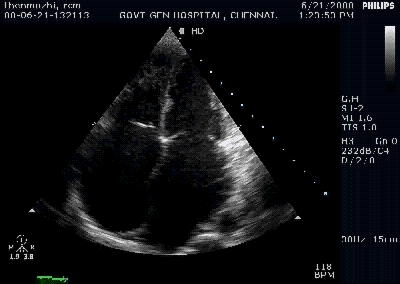
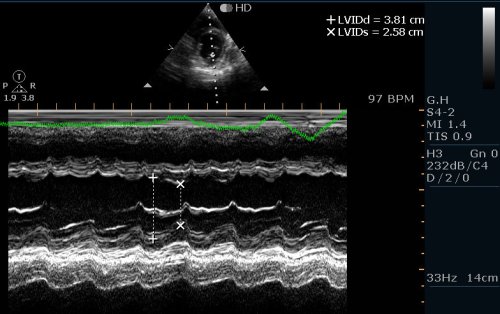
Here is 55 year old women came with extensive anterior MI with lower septal rupture.(She belonged to type 3 of the above scheme)

Note the septal rupture is visible even in 2D Echo
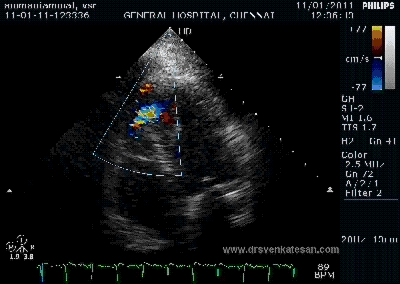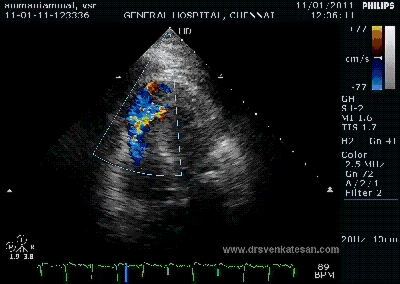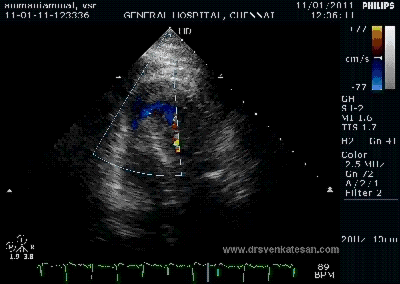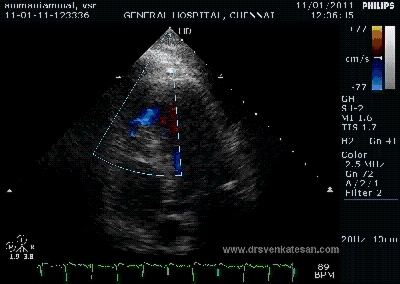
Color flow showing significant shunting from LV to RV.This shunt depends upon the LV contractile function, LVEDP and ofcourse the RV pressure
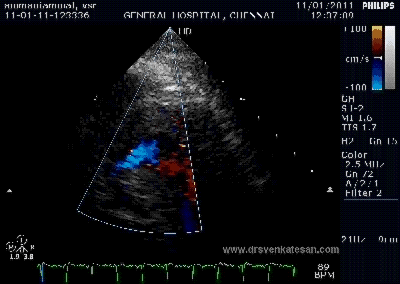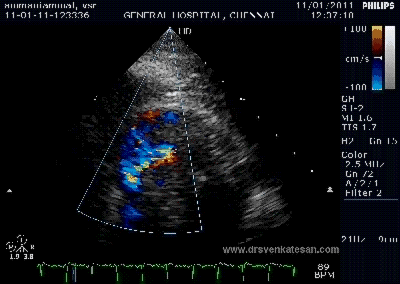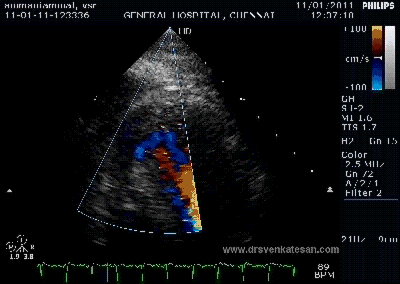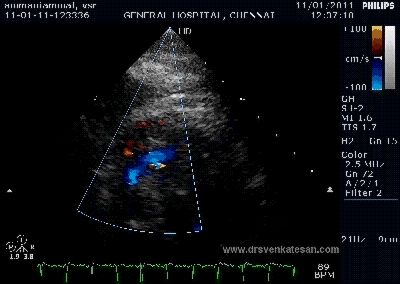
If there is severe RV dysfunction or bi ventricular dysfunction flow across the defect is inconspicuous.Brisk left to right shunting may be an indirect marker for good LV systolic function and absence of significant pulmonary hypertension.Both imply a better outcome.
The main determinant of survival is the underlying LV dysfunction and associated co morbidity(Renal function ) and complications .
Infero -posterior ruptures tend to be complex and may have multiple irregular tracks that makes it difficult to repair.
Investigations
Echo cardiogram is the mainstay .Serial echos should be done to assess the mechanical function and the progress of VSR.Hemodynamic monitoring may be done without injuring the patient .
Medical management
- Often supportive , but effective . Dobutamine infusion can maintain a life for few days.
- Paradoxically , LV dysfunction and elevated LVEDP restricts volume overloading of VSD.
- Associated MR, Arrhythmias need to be taken care of .
Surgeons role
- Very Vital.
- Experience counts.(Individual as well as Institutional )
Timing of surgery
Continues to be a controversy . Surgeons love to operate in a stable patient. But they need to realise , surgery is often needed to stabilise many patients. . The issue of tissue friability is blown out of proportion in the literature .When a life is is at danger we can not worry about friable tissues !
The rule of thumb could be
- Operate as early as possible in unstable patient.
- Post pone surgery in stable patient as late as possible ( Late here means . . .elective non emergent surgery )
Surgical options
- Simple VSR closure without knowing coronary anatomy
- Simple VSR closure after knowing coronary anatomy
- VSR closure with CABG ( total revascularization)
- VSR closure with partial revascularization
In our experience each of the above , has a role in a given patient depending upon the logistic , financial , social and even the available expertise. (A good surgeon in bad Institution !)
Is coronary angiogram mandatory before attempting to close VSR ?
Logically yes. If it is not available just do not bother . But, many times , when issue is saving lives , we can not afford to be too scientific , many lives have been saved by not following such strict protocols .A simple emergency thoracotomy and closure of rupture site (Without even touching the LAD ) can be a distinct and viable option in a selected few .
Role of cardiologists
Contrary to the popular belief the role of cardiologists is minimal , except to prepare the patient and hand over to the surgeon.
Interventional approach to close a VSR is currently be termed as an adventurous option ! The VSRs can assume unpredictable shapes and the tears can be multiple in different planes. The devices , catheters and other hard ware are not specifically made to tackle these issues .An acquired VSR should never be compared with congenital VSD.








 y
y



TRANSFER-AMI study : Transfer with caution . . . bumpy roads ahead !
Posted in Cardiology -Interventional -PCI, cardiology -Therapeutics, Cardiology -unresolved questions, cardiology journal club, cardiology journals, Uncategorized, tagged comments about transfer ami, facilitated pci, FAILED THROMOLYSIS, journal watch transer ami, letters to the editor transfer ami, nejm transfer ami, REACT STUDY, rescue pci, routine early pci, stemi, tenecteplase failure, time window for pulmoanry thromolysis, TRANSFER -AMI STUDY on January 14, 2011| Leave a Comment »
Preamble
The much published TRANSFER -AMI study has few important queries to ponder about.It was supposed to test the role of routine PCI following thrombolysis. In other words it compared rescue only strategy with routine strategy.The caveat is , even among failed thrombolysis, the rescue strategy has not convincingly proven superior to medical management (if the time is lapsed ) as much of the damage is done .
Will the investigators share their experience ?
Finally
Why the title of the paper says it is about “Routine angioplasty” and the conclusion emphasizes it is indeed “high risk subsets ofangioplasty” (While the study itself involves a 92 % least risk Killip class 1 ) . Why this double dose of confusion ? (Is it deliberate ! Which i think is unlikely )
NEJM please take note of this . . .
All that glitters are not natural glitter . . .some are made to glitter !
Rate this:
Read Full Post »